The ongoing pandemic of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) brought to the attention the pressing public health demand to adequately understand human genetic variation in response to the viral challenge.
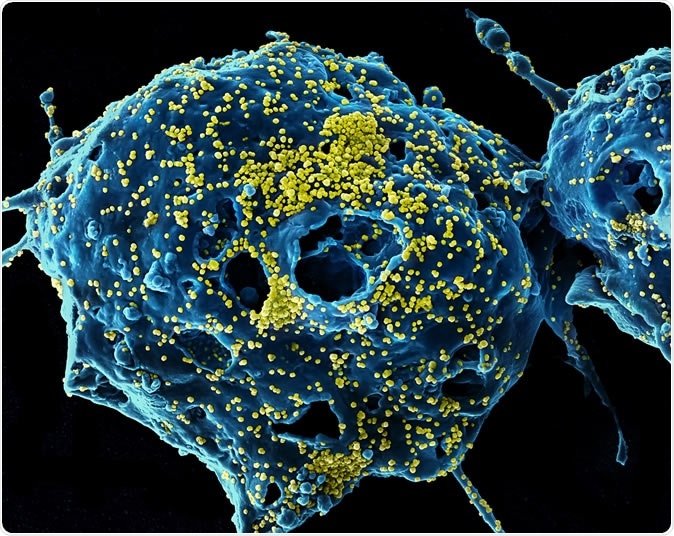
MERS Virus Particles Colorized scanning electron micrograph of Middle East Respiratory Syndrome virus particles (yellow) attached to the surface of an infected VERO E6 cell (blue). Image captured and color-enhanced at the NIAID Integrated Research Facility in Fort Detrick, Maryland. Credit: NIAID

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Humans and viruses have evolved together for millennia, resulting in genetic polymorphisms that guide the host responses to viral infection. Consequently, clinical variation in COVID-19 severity and symptomatic presentation may be a result of differences in host genetic factors related to the immune response.
This is why researchers from the University of California San Francisco, the University of Texas at Austin, and St. Jude Children's Hospital in Memphis (United States) decided to appraise the genetic architecture of host response to viral infection, especially taking COVID-19 into account
In-depth exploration of the host viral response
In this new study, the researchers utilized the data from the UK Biobank population-based cohort in order to evaluate the relationship between host genetics and its viral response. They have analyzed the data of 7,924 participants in total (predominantly of European ancestry).
The goal was to appraise 28 antigens for 16 viruses that have been linked to neurodegenerative diseases and malignancies but also to put the emphasis on the SARS-CoV-2 test in a separate subset of UK Biobank participants.
Accordingly, they have conducted integrative genome-wide and transcriptome-wide analyses of antibody response and positivity to viral antigens. Pleiotropic associations between lead variants affecting antibody levels and several chronic diseases with viral risk factors were explored in depth.
Symptom span explained by HLA genetic variations
Study findings confirm that human leukocyte antigen (HLA) class II and III genes are pivotal host genetic factors implicated in regulating the immune response to diverse viral antigens, with potential implications for complex diseases.
Furthermore, the researchers have also discovered that specific HLA alleles linked to multiple common infections are associated with SARS-CoV-2 positive tests. More specifically, based on 1028 subjects tested for SARS-CoV-2, they have identified seven class II HLA susceptibility alleles (five associated with other viruses).
"Considering genetic variation within the HLA region, our results not only confirm its pivotal role at the interface of host-pathogen interactions, but also highlight the overlap in variants, classical alleles, and genes that mediate these interactions across virus families and antigens", emphasize study authors.
Associations between HLA alleles and SARS-CoV-2 status may indicate a different clinical course with milder infection or asymptomatic status, which led to lower odds of being tested despite exposure.
This is especially valid as data used in this study was collected early in the epidemic when severely ill individuals were prioritized for testing. If true, the associations may be more robust when comparing more severe cases of COVID-19 to asymptomatic carriers.
Influencing the viral receptor
The research also pointed towards the inverse relationship between genetically predicted angiotensin-converting enzyme 2 (ACE2) gene expressions and a positive SARS-CoV-2 testing result. Albeit ACE2 plays a critical role in enabling SARS-CoV-2 cell entry, the virus appears to down-regulate ACE2 expression once inside.
"We suspect that decreased ACE2 expression may reduce viral infection by limiting available receptors for viral entry, and once a cell is infected, the reduced expression may aid SARS-CoV-2", explain study authors.
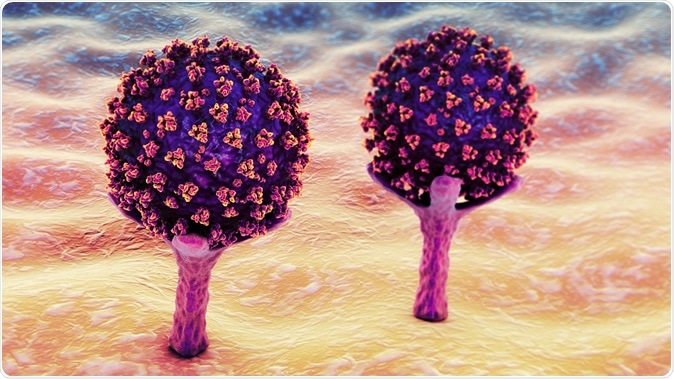
SARS-CoV-2 viruses are binding to ACE-2 receptors on a human cell, the initial stage of COVID-19 infection. Conceptual 3D illustration credit: Kateryna Kon / Shutterstock
Research implications
"Understanding the interplay between host genetic factors and immune response has implications for public health and may facilitate the discovery of novel therapeutics including vaccines," said study authors.
"Upon further elucidation of the risk of infection and COVID-19 severity, our results suggest that HLA typing may be a feasible tool in the SARS-CoV-2 response for identifying at-risk populations and, prioritizing vaccine distribution", they conclude.
Naturally, further research is needed in order to understand the viability of this approach in diverse populations, whereas therapeutic research on ACE2 inhibitors will elucidate what is happening behind the downregulation of SARS-CoV-2 receptors after infection.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Kachuri, L. et al. (2020). The landscape of host genetic factors involved in infection to common viruses and SARS-CoV-2. medRxiv. https://doi.org/10.1101/2020.05.01.20088054.
- Peer reviewed and published scientific report.
Kachuri, Linda, Stephen S. Francis, Maike L. Morrison, George A. Wendt, Yohan Bossé, Taylor B. Cavazos, Sara R. Rashkin, Elad Ziv, and John S. Witte. 2020. “The Landscape of Host Genetic Factors Involved in Immune Response to Common Viral Infections.” Genome Medicine 12 (1). https://doi.org/10.1186/s13073-020-00790-x. https://genomemedicine.biomedcentral.com/articles/10.1186/s13073-020-00790-x