The worldwide impact of the COVID-19 pandemic led to an unprecedented effort to develop vaccines against severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection on a timescale that has never been imagined before. Even as some vaccines have begun to be administered on a large scale, scientists and governments are coming up against a difficult obstacle. This is the existence of vaccine hesitancy and unwillingness among the general population. A new study published on the preprint server medRxiv* in December 2020 explores this phenomenon and the implications for public health.
The researchers examined studies dealing with vaccine attitudes in large samples (1,000 or more subjects) of the population on a nationally representative framework. In order to cover the available data in a systematic manner, they conducted both a review and a meta-analysis to find the proportion of the population with the following attitudes: willing to accept the vaccine, unsure, or unwilling to take it when it becomes available.
They obtained 28 samples, covering over 58,600 people from 13 countries. Most were from the US, the UK, and Canada, with the rest from European countries, China and Australia. The data covered the period from June to October 2020.
Pooled data from the March-October period indicates that about 73% would accept the vaccine, while ~14% would refuse it. About 22% said they were unsure. This option was not available in all studies, however, and its presence affected the number of ‘willing’ responses significantly.
In other words, without this option, about 83% indicated their willingness, but when it was given, only about 64%. The proportion of ‘unwilling’ people did not change to any significant extent, however.
The 18 studies covering March to May had a 79% proportion of ‘willing’ responses and 12% ‘unwilling’, which decreased to 60% and 20%, respectively, in the ten studies covering June to October. The number of ‘unsure’ responses did not vary with time. The change in this trend was not correlated with the country being sampled.
The findings suggest that the percentage of willing and unwilling people has been going down and up, respectively, as the pandemic dragged on.
However, there was a country-specific difference in the proportion of ‘willing’ responses, with over 90% of Chinese adults reporting their willingness in March-April, compared to 76% in France. It is worth noting that in September-October, the figures for France and the US were much lower, at around 50%.
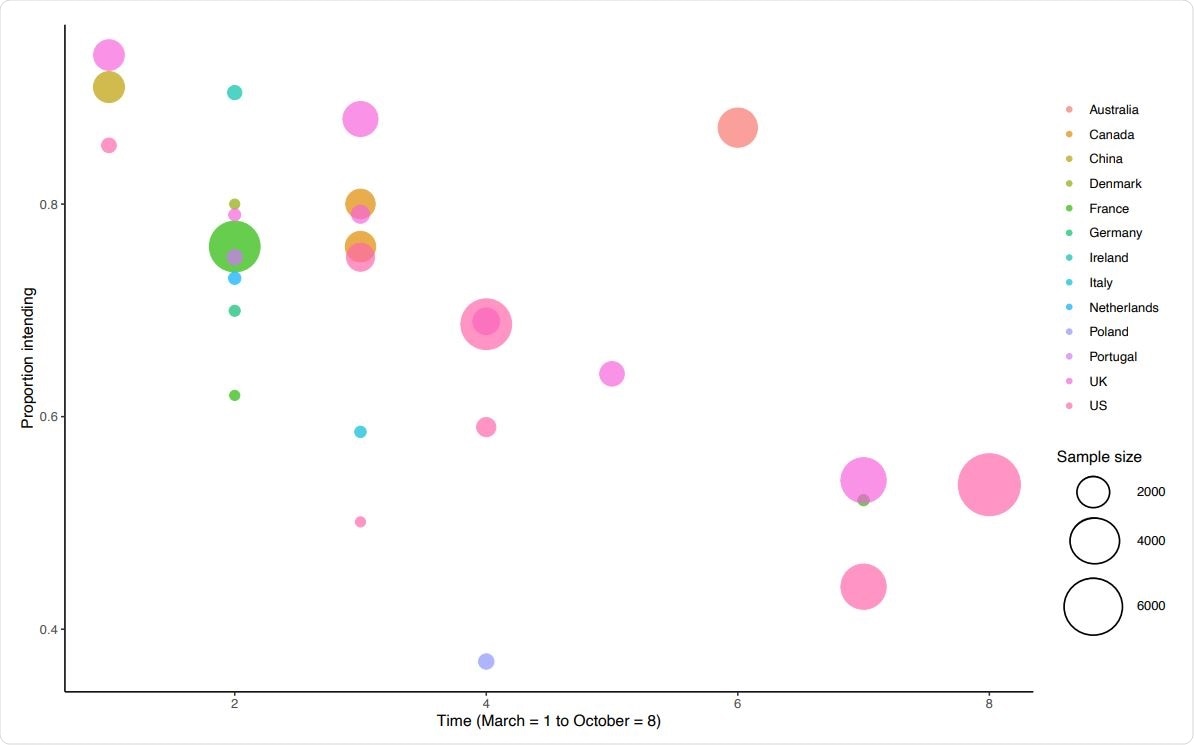
Proportion of populations intending to vaccinate by country and time
Risk Factors for Unwillingness
The risk factors for vaccine unwillingness were being female, younger, less educated, having a lower income, or being part of a minority ethnic group. In 7/11 studies, white people showed a greater willingness, but in four, this was not significant. Higher income showed a positive correlation with willingness in 8/9 studies. Having a comorbidity was a positive factor for willingness in only one study of 5.
In 12/14 studies, willingness was far more likely with older adults. In one study, younger adults were more likely to be willing than middle-aged adults, but not older adults, and in the last, there was no relation with age. Males showed greater willingness to accept the vaccine in 9/14 studies, and people with a higher level of education in half of 14 studies.
What are the Implications?
Thus, with the continued release of disinformation on a huge number of social media sites, trust in government interventions and vaccine safety began to erode. It became clear that vaccine intentions were split between 60% willingness and 20% unwillingness, varying with the sample tested.
The risk factors follow a similar pattern in all the five high-quality studies, indicating that younger people, females, and those with lower education, lower income, or from an ethnic minority, are consistently less likely to be vaccinated. The association with the effects of such misinformation campaigns and with public concerns that vaccine safety is being compromised emphasizes the need to specifically win the public over to the benefits and the safety of the new vaccines. This may require behavioral as well as scientific expertise since the issue is one of trust and acceptability rather than of validated scientific outcomes.
Strangely, individuals with a chronic health condition showed no greater willingness to accept the vaccine despite being at a much higher risk of death from COVID-19. This points to the need to target both poor and marginalized communities and medically vulnerable groups for vaccine acceptance, given that both have already suffered far more than others from the pandemic.
The authors sum up: “Intentions to vaccinate against COVID-19 among the general public when a vaccine becomes available have been declining and this will limit the effectiveness of COVID-19 vaccination programs. Findings highlight the need to improve public acceptability, trust and concern over the safety and benefit of COVID-19 vaccines and target vaccine uptake in disadvantaged groups who have already been disproportionately affected by the pandemic.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources