The coronavirus disease 2019 (COVID-19) pandemic has brought down the global economy to its knees. It has also adversely impacted the general population's psychology, in particular in children and adolescents. Some may be inflicted with pre-existing and somatic problems. In such cases, the complications are little known. Previous findings hint at positive as well as negative consequences on mental and social health.
It is known that during the COVID-19, there are increased rates of anxiety, depression, and decreased psychological well-being in the adult general population, with the adult psychiatric patients having worse symptoms. However, some studies in children report these observations and the converse of it - reduced mental problems and even improved well-being.
In this context, Josjan Zijlmans and Lorynn Teela et al. investigate the mental and social health of children and adolescents with pre-existing mental or somatic problems (pediatric or psychiatric) during the COVID-19 pandemic lockdown. The study published on the preprint server medRxiv* compares their global health, peer relationships, symptom levels of anxiety, depression and anger, and sleep-related impairment to the general population of children and adolescents.
The researchers examined the potential associated factors, including COVID-19 specific factors such as having an affected friend or relative. They also took into account changes in the home atmosphere due to the first Dutch COVID-19 lockdown and reported qualitative data on children's experiences of the COVID-19 regulations.
The team found that the pediatric samples reported the least problems on all health measures.
They observed significant differences in mental and social health between three child and adolescent samples during this period and identified COVID-19-related factors influencing mental and social health.
In the Netherlands, the first COVID-19 lockdown came into practice on March 15th, 2020. Except for parents in essential professions, children were restricted within homes, with no schooling, daycare, sports, or leisure facilities. All the lockdown measures were implemented to mitigate the infection spread. However, young children (<12 years) were, allowed to play outside with their friends.
Under these circumstances, the researchers undertook this study - the measurement window was between the end of April and early May 2020. Parents and their children completed a sociodemographic questionnaire, and the COVID-19-related questions presented to them online. The team collected the data through research websites of the KLIK PROM portal developed specifically for each group (www.corona-survey.nl, https://www.hetklikt.nu/, and www.corona-studie.nl).
The study cohort included: psychiatric sample had 249 children participate, the pediatric sample had 90 children participate, and the general population sample had 844 children participate.
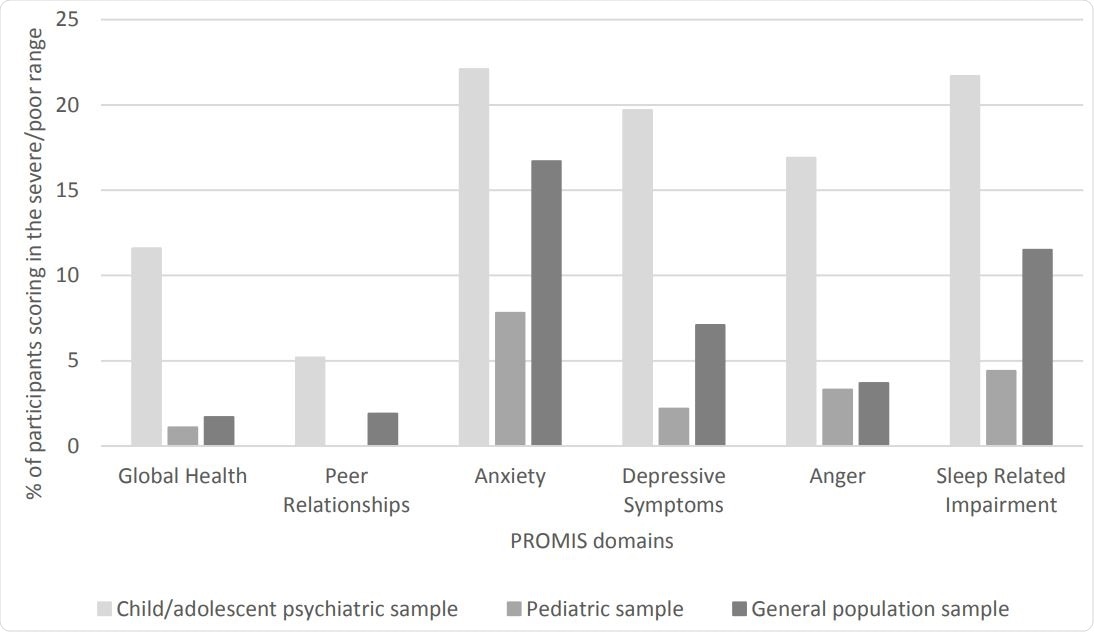
Percentage of participants scoring in the severe/poor range (>1.5 SD)* on PROMIS domains for all samples.
The researchers assessed the mental and social health between the groups via the Patient-Reported Outcomes Measurement Information System (PROMIS) domains: Global Health, Peer Relationships, Anxiety, Depressive Symptoms, Anger, and Sleep-Related Impairment.
They found that the pediatric sample had the least problems (except for Global Health), whereas the psychiatric sample had reported significantly more problems than the general population sample (except for Anxiety and Peer Relationships).
They also found that for COVID-19-specific variables, an adverse change in the parental work situation is significantly associated with more anxiety, more depressive symptoms, more anger, and more sleep-related impairment. They report that a parent having a friend or relative infected with COVID-19 is also significantly associated with higher anxiety.
Interestingly, when they studied the atmosphere at home before and during COVID-19, they found no difference between children from the psychiatric and pediatric samples. In comparison, they note that the children in the general population report a worse atmosphere.
Looking at daily life with COVID-19 regulations, only the general population children report boredom. The children and adolescents from the pediatric and psychiatric sample report difficulties keeping social-distance (e.g., hard to keep distance in daily life, not allowed to hug, and getting warnings from other people). A small number of children also reported positively.
As expected, this study shows that children with pre-existing psychiatric problems show most problems in mental and social health. However, the researchers caution that inferences and conclusions based on these observations can not be complete.
Pandemic-related mental and social disorders may lead to increased levels of anxiety, depression, and post-traumatic stress. Because children with mental problems and chronic somatic conditions are known to be at risk for psychosocial problems, the current study is important to examine the mental and social health of this vulnerable population during the COVID-19 lockdown, and the discussion opens up wider avenues.
Here, the researchers assess the mental and social health of a broad population of children with pre-existing conditions (psychiatric or pediatric) during the first COVID-19 lockdown in the Netherlands. They compare their global health, peer relationships, symptom levels of anxiety, depression and anger, and sleep-related impairment to the general population of children and adolescents.
"This study contributes to a 'call for action for mental health science' by Holmes et al. 37, who argue that this type of research should be one of the main priorities in research during the COVID-19 pandemic."

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Mental and social health of children and adolescents with pre-existing mental or somatic problems during the COVID-19 pandemic lockdown, Josjan Zijlmans, Lorynn Teela, Hanneke van Ewijk, Helen Klip, Malindi van der Mheen, Hyun Ruisch, Michiel Luijten, Maud van Muilekom, Kim Oostrom, Jan Buitelaar, Pieter Hoekstra, Ramon Lindauer, Arne Popma, Wouter Staal, Robert Vermeiren, Hedy van Oers, Lotte Haverman, Tinca Polderman, medRxiv 2020.12.15.20248237; doi: https://doi.org/10.1101/2020.12.15.20248237, https://www.medrxiv.org/content/10.1101/2020.12.15.20248237v1
- Peer reviewed and published scientific report.
Zijlmans, Josjan, Lorynn Teela, Hanneke van Ewijk, Helen Klip, Malindi van der Mheen, Hyun Ruisch, Michiel A. J. Luijten, et al. 2021. “Mental and Social Health of Children and Adolescents with Pre-Existing Mental or Somatic Problems during the COVID-19 Pandemic Lockdown.” Frontiers in Psychiatry 12 (July). https://doi.org/10.3389/fpsyt.2021.692853. https://www.frontiersin.org/articles/10.3389/fpsyt.2021.692853/full.