Researchers at GlaxoSmithKline (GSK) in Italy and Belgium say the coronavirus disease 2019 (COVID-19) pandemic is transforming the world of vaccinology by accelerating vaccine development and the availability of powerful technologies.
The team says the pandemic has fast-forwarded the development of technologies such as synthetic RNA vaccines and viral vectors by at least a decade.
Rino Rappuoli and colleagues hope that these accelerated developments, along with advances in the field of immunotherapy, might help to tackle some of the challenges that loom in the post-COVID world, such as newly emerging pathogens, antimicrobial resistance, chronic infections, and cancer.
“For instance, RNA vaccines and viral vectors may be designed to encode not only antigens but also molecules able to reactivate the dormant immune system,” they write.
.jpg)
Technological advances that merged to develop a COVID-19 vaccine
COVID-19 paints a gloomy picture of a world without vaccines
The COVID-19 pandemic has painted a disturbing picture of what the future might look like in the absence of vaccination.
“Fortunately, new technologies, the pace of understanding new and existing pathogens, and the increased knowledge of the immune system allow us today to develop vaccines at an unprecedented speed,” says Rappuoli and the team.
In a perspective piece published in the Proceedings of the National Academy of Sciences, the researchers discuss the progress made in genome-based vaccine development and some of the challenges that lie ahead where such vaccines could play an increasingly important role.
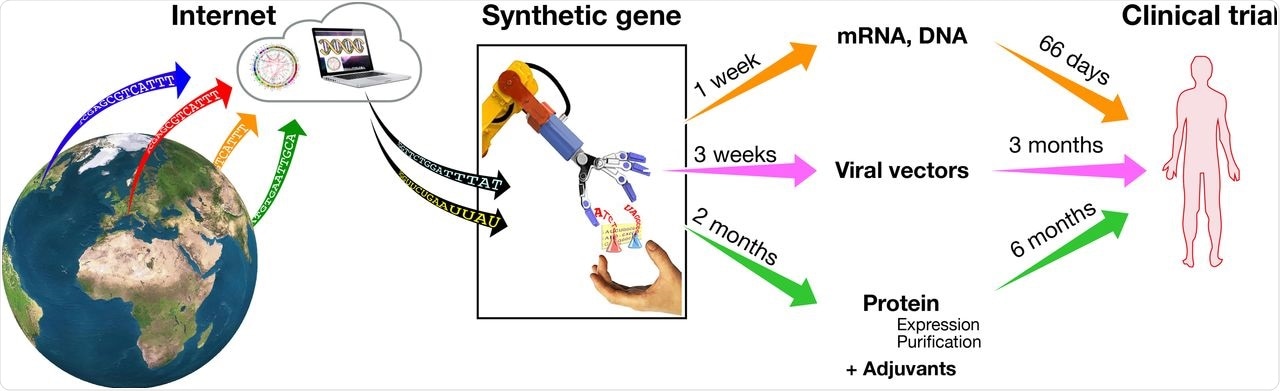
COVID-19 vaccines in development and their timeline to clinical testing in humans
Progress with genome-based vaccines began in 2013
Progress was first made with synthetic, genome-based vaccines in 2013 when researchers produced an RNA vaccine against an emerging and potentially pandemic H7N9 influenza virus.
For the first time, a fully synthetic viral vaccine was produced in vitro without culturing the virus. Instead, the genome sequence available in public databases available on the internet was used.
These so-called “internet-based vaccines,” which are developed using shared genomic information, bypass the need to transport, access, and grow the native virus.
“Fortunately, the H7N9 influenza virus did not transmit efficiently between humans, and, although it caused a few hundred cases during the next few years, it did not cause a pandemic, limiting the use of these vaccines only to clinical trials,” writes Rappuoli and colleagues.
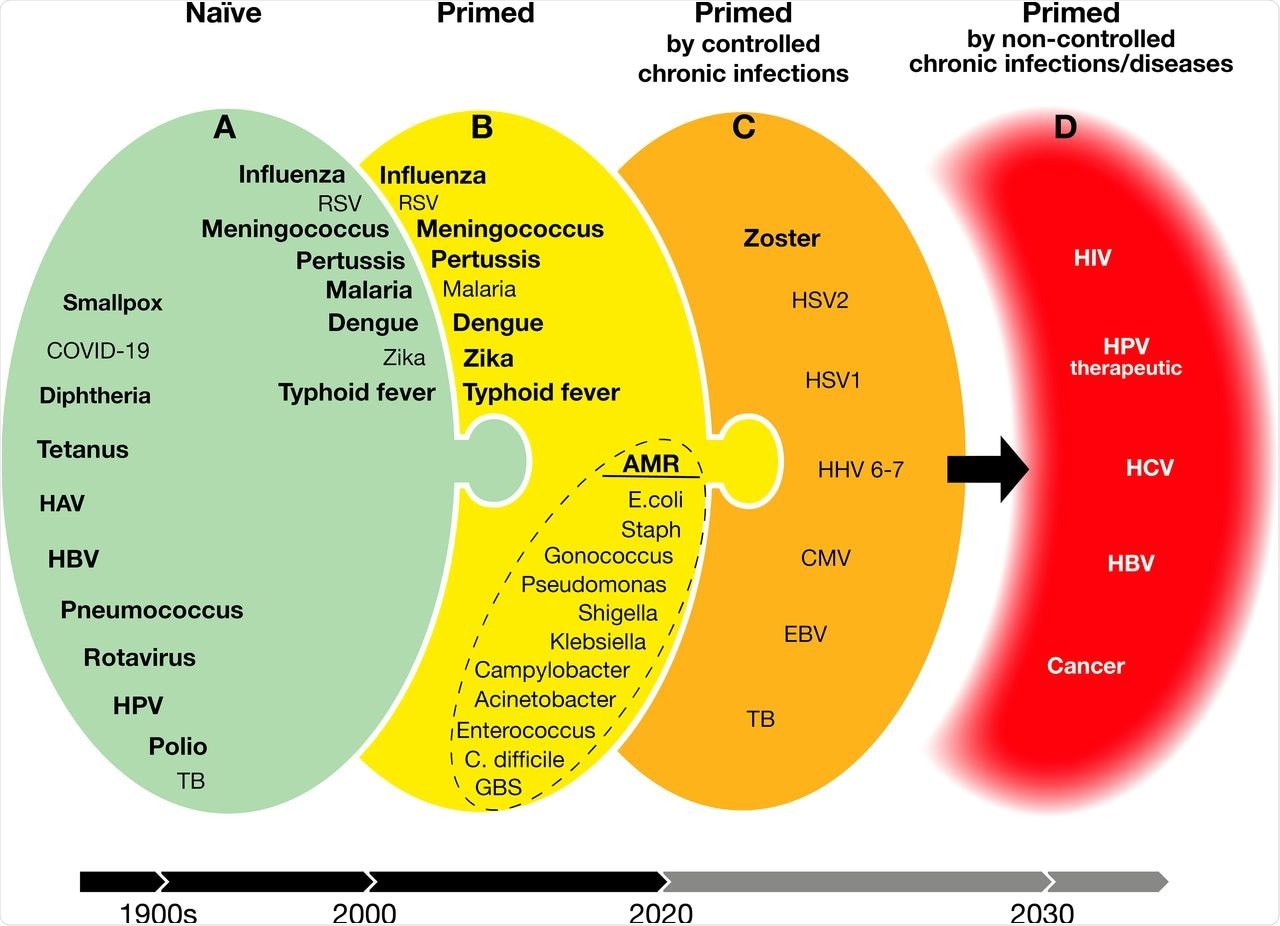
Vaccines developed addressing naïve, previously exposed, and chronic infections. Green (A) are vaccines available or doable with existing technologies. Bold, available vaccines. Yellow (B) and orange (C) are doable vaccines with increasing challenges for today’s technologies. Red (D) are targets for which we do not yet have the scientific knowledge and technologies. HAV, hepatitis A virus; HBV, hepatitis B virus; HPV, human papillomavirus; TB, tuberculosis; RSV, respiratory syncytial virus; AMR, antimicrobial resistance; E. coli, Escherichia coli; Staph, Staphylococcus aureus; C. difficile, Clostridium difficile; GBS, group B Streptococcus; HSV1, herpes simplex virus 1; HSV2, herpes simplex virus 2; HHV, 6-7 human herpes viruses 6 and 7; CMV, cytomegalovirus; EBV, Epstein-Barr virus; HIV, human immunodeficiency virus; HCV, hepatitis C virus.
Labs worldwide had the ability to make genomic vaccines before COVID-19
By the time the genomic sequence for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) – the agent responsible for COVID-19 – was made publicly available on the internet in January 2020, most laboratories worldwide were already able to make vaccines from synthetic genes.
Several approaches are used to make COVID-19 vaccines, but here, the researchers focus on three main types of internet-based vaccines that are undergoing massive developmental acceleration: synthetic RNA vaccines, viral vectors, and adjuvanted protein-based vaccines.
Synthetic RNA vaccines are the quickest of the three to develop. A fully synthetic gene, which is cloned in a plasmid vector, serves as a template for in vitro synthesis of the RNA vaccine.
For viral vectors, a synthetic gene encoding the viral spike protein that SARS-CoV-2 uses to infect cells is inserted into a virus that has been engineered to not replicate in humans. After being grown in culture, the virus is delivered into the body via vaccination, delivering the synthetic gene to cells.
In the case of protein-based vaccines, a synthetic gene encoding the spike protein or its receptor-binding domain is used to engineer mammalian, viral or plant cells that produce the protein. This recombinant protein is then purified and mixed with adjuvants to create a vaccine.
Challenges faced in the post-COVID world
The researchers say the accelerated development of these RNA and viral vectors has meant these platforms are now available not only for emerging infections but also for other looming public health threats the post-COVID world will have to face.
For example, bacteria that are resistant to antibiotics pose a significant public health threat, with people potentially vulnerable to recurrent infection with pathogens such as Escherichia coli, Staphylococcus aureus, Clostridium difficile, Klebsiella pneumoniae, and Pseudomonas aeruginosa.
This antimicrobial resistance (AMR) is effectively a slowly evolving pandemic that is predicted to have devastating effects on public health and the economy globally over the next two decades, says Rappuoli and the team.
However, vaccines could help to tackle AMR, they add: “We have enough technologies and empirical knowledge to develop new vaccines for AMR.”
Chronic infection and cancer
In some cases, the immune system is completely defeated by pathogens such as HIV or conditions such as cancer and the body is left prone to chronic infection. The immune system is unable to control the pathogen or cancer cells, which are then free to replicate indefinitely.
“So far, we have not been able to make successful vaccines against these diseases, and we do not have the scientific knowledge to make them,” say the researchers.
However, immunotherapy research has shown that in the case of cancer, the defeated immune system is characterized by dormant regulatory T cells that can be activated using certain antibodies.
“The success of immunotherapy in the field of cancer and the increased understanding of mechanistic features of the defeated immune system suggest that, in the near future, vaccination may also be able to conquer cancer and chronic diseases,” writes Rappuoli and colleagues.
“It is possible that evolution of the new technologies fast-tracked for COVID-19 (RNA vaccines, viral vectors, and protein-based vaccines with potent adjuvants) combined with the learning coming from immunotherapy will be the answer for some of the new challenges of modern society such as emerging infections, AMR, chronic infections, and cancer,” concludes the team.