More than a year into the coronavirus disease (COVID-19) pandemic, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), scientists continue to work towards better understanding how the virus spreads. Though the virus is known to spread by respiratory droplets, the role of surface contamination in viral transmission remains unclear.
Researchers in Canada aimed to determine the burden of SARS-CoV-2 in the air and on surfaces in the rooms of patients hospitalized with COVID-19. To this end, the researchers found higher surface contamination to be present in the rooms of patients who were at early stages of the disease, as well as those with hypoxia, multiple comorbidities, and higher SARS-CoV-2 ribonucleic acid (RNA) concentrations in their nasopharyngeal swabs.
The study, which appeared on the pre-print server medRxiv*, suggests that air and surfaces may pose a limited risk after being hospitalized for several days due to COVID-19.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
How is SARS-CoV-2 transmitted?
SARS-CoV-2 primarily spreads through the inhalation of respiratory droplets expelled when an infected person coughs, sneezes, speaks or breathes.
The World Health Organization (WHO) reports that the transmission of SARS-CoV-2 can happen through direct, indirect, or close contact with an infected person through infected secretions like saliva, respiratory secretions, or respiratory droplets.
Respiratory droplet transmission occurs when a person is in close contact of at least 1 meter with an infected person with respiratory symptoms. Meanwhile, indirect contact transmission of SARS-CoV-2 occurs when a susceptible host comes in contact with contaminated objects or surfaces, known as fomite transmission.
Understanding the role of surface and air (environmental) contamination in SARS-CoV-2 transmission is vital to prevent viral transmission between patients and healthcare workers in acute care hospitals.
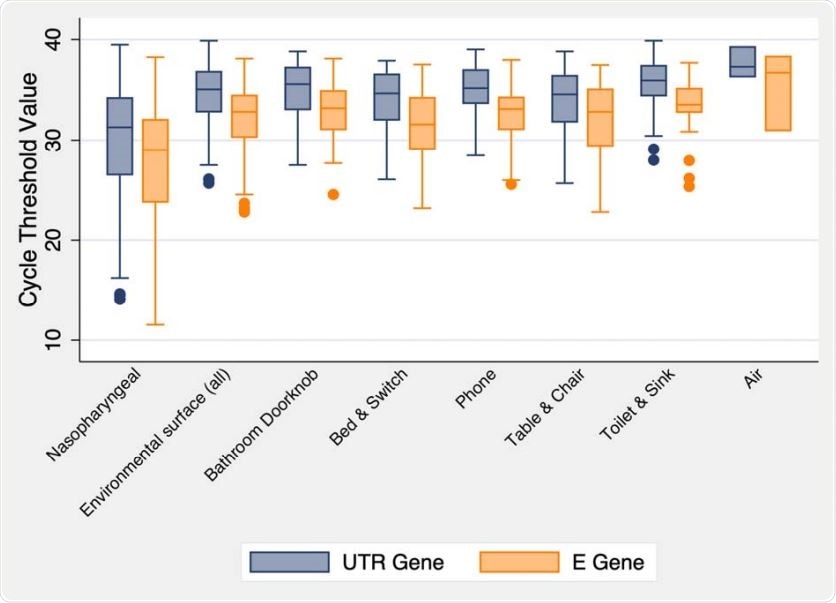
Boxplot summary of the cycle threshold values for the UTR gene (blue) and E gene (green) targets from the SARS-CoV-2 PCR analysis for each sample type investigated for 78 COVID-19 positive patients in Toronto, Canada. Notably, air sampling pumps were calibrated to a flow rate of 3·5 L/min for 2 h; each air sample represents 420 L of air.
Surface and environmental contamination
The current study aimed to determine the burden of SARS-CoV-2 in the air and on surfaces in the hospital rooms of COVID-19 patients.
To arrive at the study findings, the team collected nasopharyngeal swabs, as well as both surface and air samples from the rooms of 78 COVID-19 patients admitted at six acute care hospitals in Toronto between March and May of 2020. The researchers tested the samples for viral RNA and subsequently cultured these samples to check for infectivity. Further, the team compared SARS-CoV-2 whole-genome viral sequences from patient nasopharyngeal swabs and surfaces in their rooms.
The team found SARS-CoV-2 RNA present on both the surfaces and in the air of COVID-19 patient rooms. About 14% of the surface samples from three patients showed viable viruses, thus indicating that exposure to these areas could cause infection.
Further findings revealed that the following factors were associated with the presence of SARS-CoV-2 on surface samples in the hospital rooms of COVID-19 patients:
- Hypoxia upon admission to the hospital
- A cycle threshold of more than 30 in a polymerase chain reaction (PCR)-positive nasopharyngeal swab
- Shorter time from symptom onset to sample date
- Higher Charlson comorbidity score
“The genomic analyses of whole SARS-CoV-2 sequences in the present work confirmed patients were the source of viral contamination of their immediate surroundings in the inpatient setting,” the researchers noted.
Conclusion
Taken together, the researchers of the present study noted that the risk to healthcare workers from exposure to the air and near-patient surfaces in hospital wards is likely limited. However, transmission can still happen since surface contamination is higher when patients are in the early stages of infection, hypoxic, have multiple comorbidities, and have higher SARS-CoV-2 RNA levels.
“Our results suggest that air and surfaces may pose limited risk a few days after admission to acute care hospitals,” the researchers concluded in the study.
The study findings shed light on surface and air contamination in COVID-19 wards. Though the use of personal protective equipment is implemented in these settings, healthcare workers are still at a high risk of infection. Knowing how they become infected is, therefore, crucial to enforce precautions against infection.
However, the study finds that SARS-CoV-2 RNA was detected on a minority of surfaces in COVID-19 patients’ rooms and rarely in air samples. This suggests these sources are unlikely to pose a significant exposure risk in hospitals. The team emphasized that while early detection and isolation of COVID-19 patients are crucial, air and surfaces may still pose a limited risk a few days after admission.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Source:
Journal references:
- Preliminary scientific report.
Kotwa, J., Jamal, A., Mbareche, H. et al. (2021). Surface and air contamination with SARS-CoV-2 from hospitalized COVID-19 patients in Toronto, Canada. medRxiv. doi:10.1101/2021.05.17.21257122. https://www.medrxiv.org/content/10.1101/2021.05.17.21257122v1
- Peer reviewed and published scientific report.
Kotwa, Jonathon D, Alainna J Jamal, Hamza Mbareche, Lily Yip, Patryk Aftanas, Shiva Barati, Natalie G Bell, et al. 2021. “Surface and Air Contamination with Severe Acute Respiratory Syndrome Coronavirus 2 from Hospitalized Coronavirus Disease 2019 Patients in Toronto, Canada, March–May 2020.” The Journal of Infectious Diseases 225 (5): 768–76. https://doi.org/10.1093/infdis/jiab578. https://academic.oup.com/jid/article/225/5/768/6444802.