The increased infectiousness and faster transmission of severe acute respiratory syndrome 2 (SARS-CoV-2) variants, along with the resistance towards masking and vaccinations, have made it difficult to predict the trajectory of the pandemic. In the United States, the Delta variant disrupted the low number of cases observed in the summer and caused a higher surge of infections than initially anticipated.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
The researchers write:
“The projections indicate that even with substantial vaccination coverage, the increased transmissibility of new variants like Delta can continue to challenge our ability to control this pandemic.”
Their findings suggest low vaccination uptake will extend the pandemic’s presence for the rest of the year. States with low vaccination rates are likely to be most affected by rising COVID-19 cases and hospitalizations. The research team recommends that states increase vaccine efforts and reinstitute measures such as indoor masking to limit transmission further.
Getting more people vaccinated will likely mitigate Delta’s impact, preventing approximately 1.5 million COVID-19 cases and 21,000 deaths.
How they did it
The COVID-19 Scenario Modeling Hub used data available from July 3, 2021, to predict the trajectory of state and national cases, hospitalizations, and deaths in the United States for the next 6 months.
Four scenarios were constructed that considered low and high vaccination hesitancy levels, vaccination efficacy for SARS-CoV-2, and lower (40%) or higher (60%) transmissibility from the Delta variant compared to the Alpha variant.
High Delta transmission and low vaccination uptake
If the Delta variant is 60% more transmissible than Alpha, COVID-19 cases, hospitalizations, and deaths are predicted to increase throughout the summer and reach their peak in mid to late September 2021.
In the “most pessimistic scenario,” high Delta transmission and low vaccination coverage will drive a peak of 414,000 weekly COVID-19 cases and 5,900 weekly deaths nationwide. The model projects there will be a total of 7,554,000 cases and 96,000 deaths from July 2021 to January 2022.
High Delta transmission but high vaccination uptake
Modeling results suggest that having 80% of the country vaccinated by January 1, 2022, will help weaken Delta’s impact on the nation. At Delta’s peak, vaccination coverage translates to 17% fewer cases and 22% fewer deaths per week. Compared to a 70% vaccination coverage, a national vaccination rate of 80% should result in 20% fewer cases and 22% fewer deaths from July to January of next year.
States at risk for a surge of COVID-19 cases
The researchers predict 10 states — Louisiana, Hawaii, Nevada, Arkansas, Missouri, Florida, Utah, Georgia, Alabama, and Mississippi — will have the most significant number of COVID-19 cases in the nation. From July 3, 2021, these states had about 52% of their eligible population vaccinated with at least one dose.
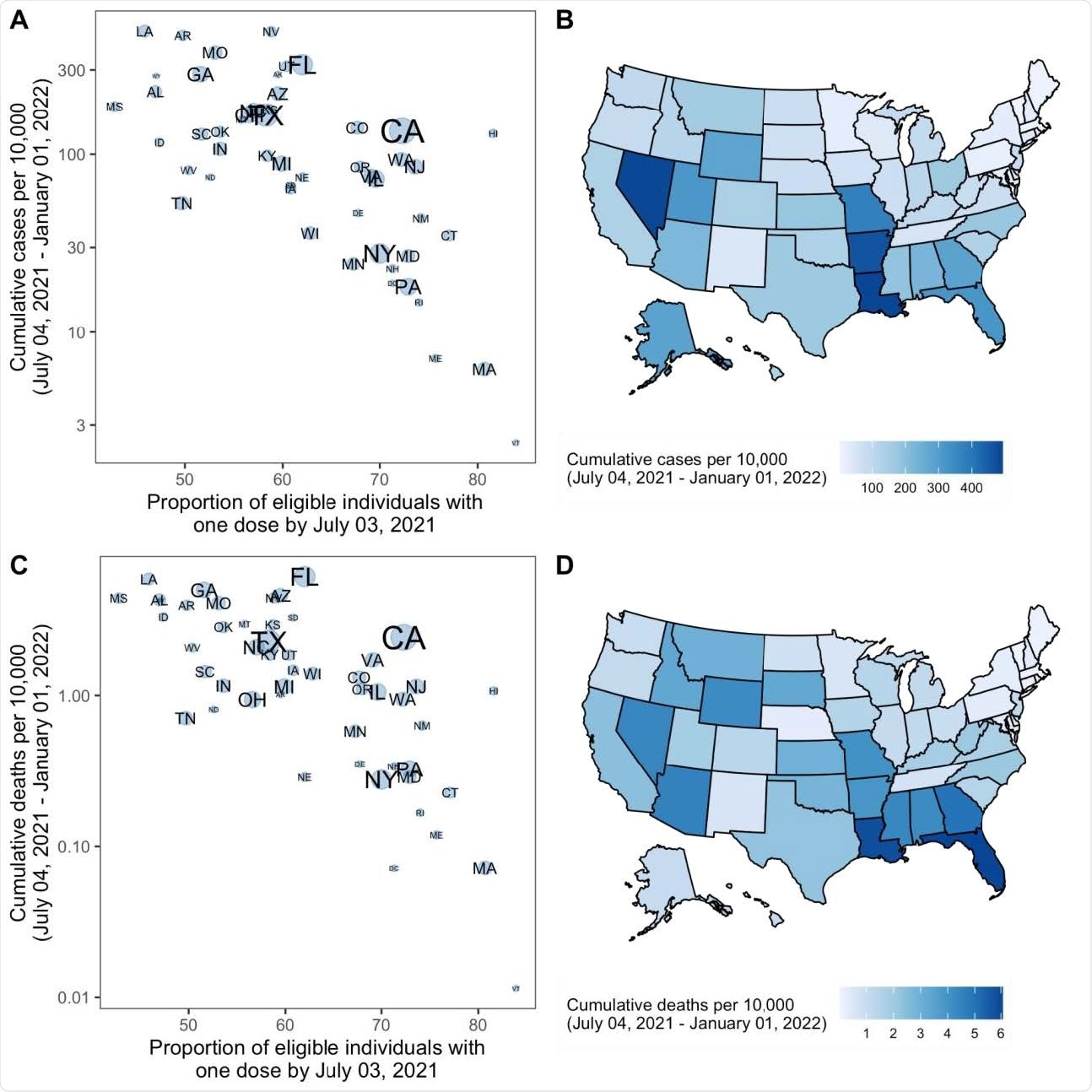
Projected cumulative cases and mortality in the most pessimistic scenario (low vaccination, high variant transmissibility) and current vaccination coverage by state — United States, July 4 2021–January 1, 2022. (A) Correlation between cumulative projected cases per 10,000 population during the 6-month period and proportion of the eligible population vaccinated with at least one COVID-19 vaccine dose by July 3, 2021, by state. Circle sizes represent population size. (B) Cumulative projected cases per 10,000 population during the 6-month period, by state. (C) Correlation between cumulative projected deaths per 10,000 population during the 6-month period and proportion of the eligible population vaccinated with at least one COVID-19 vaccine dose by July 3, 2021, by state. Circle sizes represent population size. (D) Cumulative projected deaths per 10,000 population during the 6-month period, by state.
In contrast, states such as Massachusetts, Minnesota, Rhode Island, Pennsylvania, North Dakota, Wisconsin, Vermont, Maine, Tennessee, and New York are projected to have the lowest number of COVID-19 cases. These states have approximately 71% of their 12 years and older population with at least one vaccine dose.
High vaccination rates were associated with lower COVID-19–related deaths overall.
“The impact of vaccination is already being observed: in the ten states with the largest projected resurgence there has been a 9% reduction in the observed case fatality ratio (CFR) comparing August-December 2020 and January-July 2021; in the ten states with the least projected resurgence a 21% reduction in CFR has been observed. During the projection period, we project reductions of 15% and 14%, as compared to August-December 2020,” explained the researchers.
Since July 31, 2021, some states had already exceeded the study’s estimates on weekly and cumulative COVID-19 cases. For example, of the 10 states predicted to have the highest number of cases, 7 have already experienced a rapid case growth beyond the researcher’s worst-case scenario.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Truelove S, et al. Projected resurgence of COVID-19 in the United States in July—December 2021 resulting from the increased transmissibility of the Delta variant and faltering vaccination. medRxiv, 2021. doi: https://doi.org/10.1101/2021.08.28.21262748, https://www.medrxiv.org/content/10.1101/2021.08.28.21262748v2
- Peer reviewed and published scientific report.
Truelove, Shaun, Claire P. Smith, Michelle Qin, Luke C. Mullany, Rebecca K. Borchering, Justin Lessler, Katriona Shea, et al. 2022. “Projected Resurgence of COVID-19 in the United States in July—December 2021 Resulting from the Increased Transmissibility of the Delta Variant and Faltering Vaccination.” ELife. June 21, 2022. https://elifesciences.org/articles/73584. https://elifesciences.org/articles/73584.