The coronavirus disease (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) commonly results in mild coronavirus disease (COVID-19) characterized by fever, cough, and shortness of breath. However, in some patients, it progresses to a severe infection resulting in respiratory failure, cardiovascular disorders, and thromboembolism (blockage of blood vessels due to formation of blood clots).
The uncontrolled inflammatory response is a hallmark feature of severe COVID-19 infection. Presently, it is treated using immunosuppressants like corticosteroids and by inhibiting the cytokine interleukin-6 (IL-6), which stimulates the immune response using tocilizumab.
COVID-19 is currently being monitored by evaluating the levels of inflammatory markers such as albumin, C-reactive protein (CRP), lymphocyte abundance, Interleukin (IL)-6, and D-dimer which is produced by fibrin degradation. Evaluation of both the inflammatory and physiological state of the patients with severe COVID-19 is necessary for a complete understanding of their condition.
Metabolomics is the comprehensive study of metabolites within cells, tissues, or body fluids and is a representation of the molecular phenotype of an organism. Metabolites and their interactions within a biological system is called metabolome which tends to change during various physiological and pathological states.
In a new study posted to the medRxiv* server scientists from Weil Cornell University and Stony Brook University in New York attempted to identify the metabolic and immune markers associated with severe COVID-19 disease using high-throughput targeted nuclear magnetic resonance (NMR) spectroscopy and high-dimensional flow cytometry. This will facilitate risk stratification, monitoring, and therapeutic interventions in COVID-19 patients.
Metabolic changes in COVID-19 infected patients
Metabolic species, specifically lipids, have been found to be important in viral infections. Apart from playing a role in vital functions in the host like energy supply, molecular trafficking, and signaling, lipids are also essential for pathways in viral pathology.
Changes induced by SARS-CoV-2 in the host's metabolism may result in altered levels of metabolites like glucose and lipids. These changes in metabolite levels may cause a favorable environment for viral infections by altering intracellular signaling and the immune response in the body. Thus, the metabolome of COVID-19 patients may serve as a biomarker to evaluate infection severity.
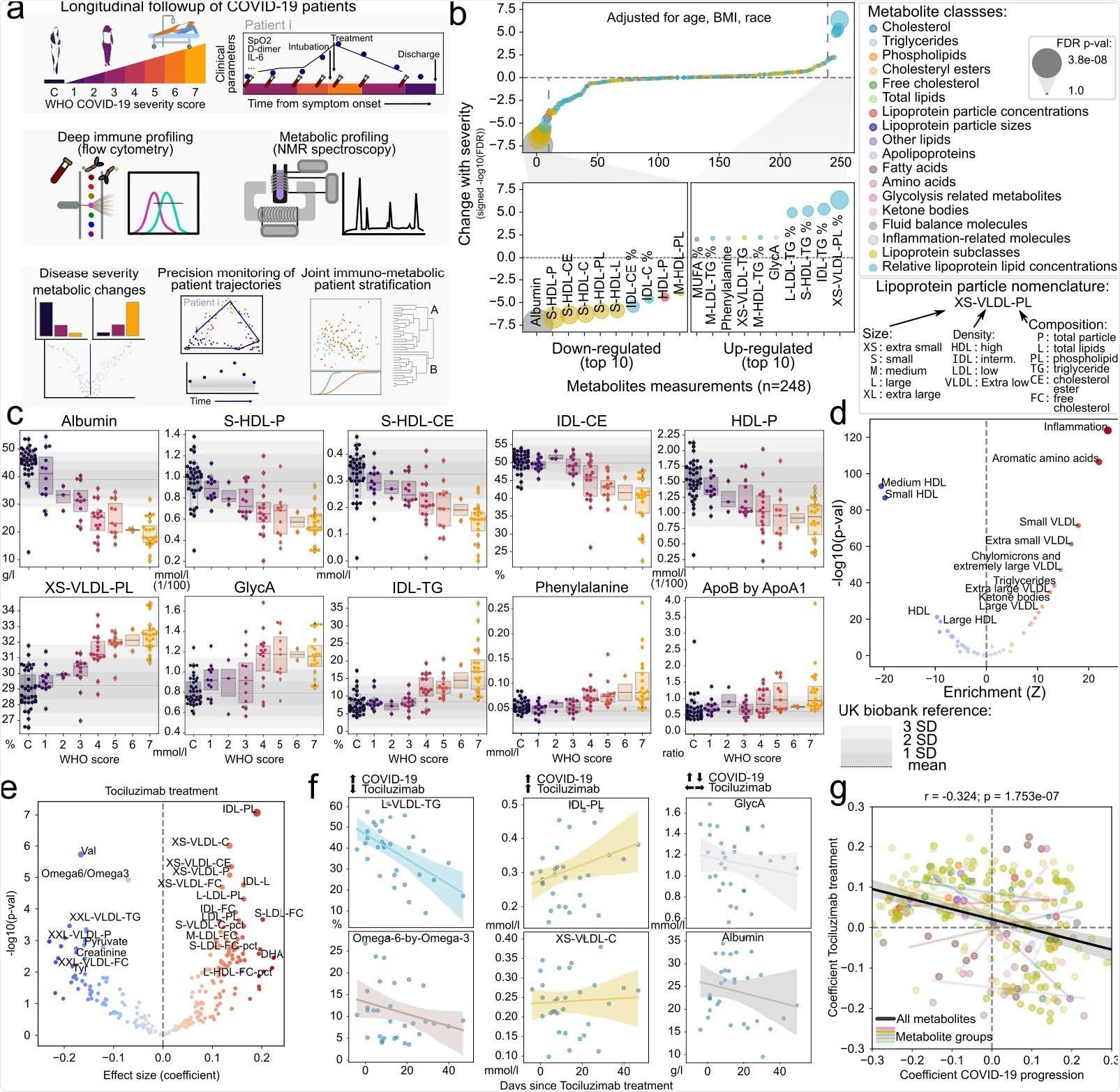
Discovery of metabolic biomarkers of COVID-19 severity and treatment. a) Schematic description of the patients under study, data types collected and approaches for their analysis. b) Association of metabolite abundance with COVID-19 severity for all 248 metabolic species (upper panel). The lower panel illustrates the 10 metabolites most associated with disease severity for each direction. c) Distribution of metabolite abundance for the metabolites most associated with COVID-19 severity depending on the sample WHO score classification. The grey horizontal dashed line represents the mean abundance of the metabolite in over 150,000 individuals from the UK biobank cohort and grey bars represent the standard deviation from the mean. d) Enrichment analysis of metabolites changing with COVID-19 severity in functional terms. e) Association of metabolite abundance with the time since tocilizumab treatment. The coefficient values refer to the change per day in relation to the mean. f) Abundance of metabolites with discordant (left), concordant (center) or indifferent (right) change between COVID-19 severity and tocilizumab treatment for treated patients. g) Comparison of the coefficients of change in COVID-19 severity (x-axis) and effect of tocilizumab treatment over time (y-axis). Each point is a metabolite colored by its class identity as in b). The black regression line indicates the overall trend between all metabolites, while the colored regression lines indicate the trend for each group of metabolites as in panel b).

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Metabolic profiling of COVID-19 patients using NMR
Longitudinal NMR metabolomics was performed on 75 patients who either had an acute infection or were recovering from COVID-19. The patients were categorized based on the World Health Organization disease severity scale (WHO score). Of the 75 patients, 35 (47%) had low to mild disease, and 30 (40%) had moderate to severe disease.
Serum samples were collected from the COVID-19 patients included in the study and from healthy COVID-19 negative patients who were treated as controls. Targeted high throughput NMR-based detection of metabolites was performed on the collected serum samples. The analysis detected metabolites associated with COVID-19 infections, including lipids, fatty acids, apolipoproteins, amino acids, ketone bodies. Metabolites like albumin, creatinine were also detected.
Metabolic changes that correlated with COVID-19 severity and treatment was identified
COVID-19 disease severity based on WHO score was correlated with the metabolites identified through NMR spectroscopy. Fifty-six metabolites, most of which belonged to lipid and lipoprotein categories, showed significant association with disease severity. Among the metabolites that were altered in severe COVID-19 patients, it was observed that increased triglyceride content and VLDL was associated with severe COVID-19. Similarly, a decrease in HDL levels, percentage of cholesterol/cholesteryl esters in HDL, and IDL were also associated with severe infections.
Analysis was further performed to identify the metabolite groups segregated based on their biophysical properties and physiological roles associated with COVID-19 severity. Increased levels of inflammatory markers, amino acids and triglycerides were observed in severe COVID-19. In general, increased severity correlated with a decrease in lipoprotein density and increase in size.
The study also analyzed if routine clinical biomarkers for COVID-19 like lactate dehydrogenase (LDH), aspartate aminotransferase (AST) and alanine aminotransferase (ALT) were associated with disease severity. It was found that only LDH showed a significant correlation with disease severity.
Metabolic changes associated with Tocilizumab treatment
Tocilizumab is recommended for COVID-19 patients with severe disease exhibiting high levels of inflammatory markers and increasing oxygen demand. In the study population, ten patients had received Tocilizumab therapy. Analysis of the metabolites in serum samples from these patients identified numerous altered metabolites that may be associated with Tocilizumab therapy. The study revealed an increase in VLDL particles and their free and esterified cholesterol content. Further, it was observed that there was a decrease in valine levels, triglyceride content of VLDL, and the ratio of omega 6 to omega 3 polyunsaturated fatty acids (PUFA). Some of the metabolites that were altered in patients with severe COVID-19 were not affected in tocilizumab-treated patients.
The study also identified a pattern in the metabolite levels that corresponded with patients with mild COVID-19. This is suggestive of the fact that Tocilizumab treatment may have reversed some of the adverse effects in the metabolism of patients with severe COVID-19.
Stratification and monitoring of COVID-19 patients using metabolomics and joint immune – metabolic profile
The study attempted to track clinical trajectories of patients based on metabolic data to facilitate the identification and monitoring of high-risk patients for severe disease and adverse outcomes.
The metabolome data was correlated with disease severity, adverse outcomes and timeline of disease progression. Increased rates of metabolic changes may be due to the combined effect of COVID-19 infection, treatment administered, and the host response.
The analysis found that increased rates of metabolic changes with time may be associated with worse outcomes. Over time, the patterns of metabolite change in COVID-19 patients can be utilized to perform real-time monitoring of disease progression.
The metabolic alterations in COVID-19 patients may be mediated by immune effectors, which may also play a role in regulating enzymes involved in lipid metabolism. Correlation between COVID-19 patient's metabolomics data from NMR spectroscopy and immune profiles from flow cytometry were further explored.
Positive associations where metabolites and immune components vary in the same direction and negative associations wherein they vary in opposite directions were identified.
Patients were stratified into groups based on their distinct clinical parameters and joint immune-metabolic profile based on the relationship between the NMR and flow cytometry data.
For example, the patients stratified into the mild disease group could be identified by their BMI, liver enzymes levels, and lipoprotein triglyceride content.
In the case of a group of patients with severe disease, the patients whose samples were collected at an early stage of symptom onset (early severe disease) showed a distinct profile compared to patients whose samples were collected later (late severe disease).
The early severe disease group had high levels of immunoglobulins G and M, which decreased at later stages of disease. High levels of creatinine levels characterized the late severe disease group.
COVID-19 patients can be stratified based on their clinical characteristics, metabolomics, and joint immune–metabolic profile to facilitate real-time monitoring, risk prediction, and early intervention.
COVID-19 patient's metabolomic and joint immune-metabolic profiles may serve as tools for better treatment outcomes
The findings from the present study suggest that:
- In COVID-19 patients, distinct metabolic changes occur, which can be correlated with disease severity.
- The alterations in the lipid metabolism and levels of lipoproteins and fatty acids observed in severe COVID-19 infection may be associated with the adverse cardiovascular outcomes and thrombotic events observed in these patients.
- IL-6 inhibitor Tocilizumab partially reverses the adverse outcomes in severe COVID-19 patients. This suggests that metabolic changes in these patients may be due to cytokine-mediated modulation of metabolic enzymes, energy consumption by cytokine-producing cells or action of immune cells on tissues in the body.
- Metabolomics and joint immune-metabolic profiles may serve as tools to stratify and monitor high-risk patients for early intervention promoting better health outcomes.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Sources:
Journal references:
- Preliminary scientific report.
Rendeiro, A. F. et al. Metabolic and immune markers for precise monitoring of COVID-19 severity and treatment. 2021.09.05.21263141 https://www.medrxiv.org/content/10.1101/2021.09.05.21263141v1
- Peer reviewed and published scientific report.
Rendeiro, André F., Charles Kyriakos Vorkas, Jan Krumsiek, Harjot K. Singh, Shashi N. Kapadia, Luca Vincenzo Cappelli, Maria Teresa Cacciapuoti, Giorgio Inghirami, Olivier Elemento, and Mirella Salvatore. 2022. “Metabolic and Immune Markers for Precise Monitoring of COVID-19 Severity and Treatment.” Frontiers in Immunology 12 (January). https://doi.org/10.3389/fimmu.2021.809937. https://www.frontiersin.org/articles/10.3389/fimmu.2021.809937.