Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) RNA has been detected in air samples of coronavirus disease (COVID-19) wards, depicting airborne dissemination of the virus.
The UK repurposed several general wards into specialized intensive care units (ICUs) during the COVID-19 pandemic when hospitals faced a lack of beds. However, these wards did not have the capacity for frequent air changes.
Despite healthcare workers using appropriate personal protective equipment (PPE) with the capacity to filter medium and large size droplets, viral transmission from patients to hospital staff is commonplace—attributed to the inhalation of viral particles in small (< 5µM) aerosols. Furthermore, nosocomial infections continue to plague healthcare systems; reducing the risk of SARS-CoV-2 airborne transmission can enhance safety for healthcare workers and patients.
Studies have found that improved ventilation coupled with ultraviolet (UV) light sterilization is a better preventive measure than respiratory protective equipment. It was proposed that portable air filtration systems—capable of combining high-efficiency particulate filtration and UV light sterilization—may be an achievable solution for warding off respiratory SARS-CoV-2.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Setting
University of Cambridge researchers conducted a study in two repurposed COVID-19 units in Addenbrooke’s Hospital, Cambridge, UK, between January and February 2021. During this time, the alpha variant (lineage B1.1.7) accounted for >80% of the circulating SARS-CoV-2. This study, posted to the medRxiv* preprint server, aimed to provide evidence of the removal of SARS-CoV-2 and microbial bioaerosols using portable air filters with UV sterilization.
The study was conducted in a repurposed ‘surge ward’ and ‘surge ICU.’ The surge ward managed patients requiring simple oxygen therapy or no respiratory support, wherein no aerosol-generating procedures were performed. An AC1500 HEPA14/UV sterilizer was installed in this ward.
Patients in the surge ICU were managed through invasive and non-invasive respiratory support with non-invasive mask ventilation, high flow nasal oxygen or invasive ventilation via endotracheal tube or tracheostomy. A Medi 10 HEPA13/UV sterilizer was installed in this ward.
The air filters were fixed prior to the initiation of the three-week study. In the second week, the air filters were switched on and run continuously for 24 hours per day providing approximately 5-10 room-volume filtrations per hour.
The study entailed a crossover evaluation with the primary goal of detecting SARS-CoV-2 in various size fractions of air samples from the surge ward and surge ICU with and without air filtration, with UV sterilization.
To detect the presence of airborne SARS-CoV-2 and other microbial bioaerosols National Institute for Occupational Safety and Health (NIOSH) two-stage cyclone aerosol samplers and multiplex qPCR assays were employed.
Mann-Whitney U-test was used to compare the difference in the number of pathogens detected when the air filter was on and off – with statistical significance being inferred when p values were ≤0.05.
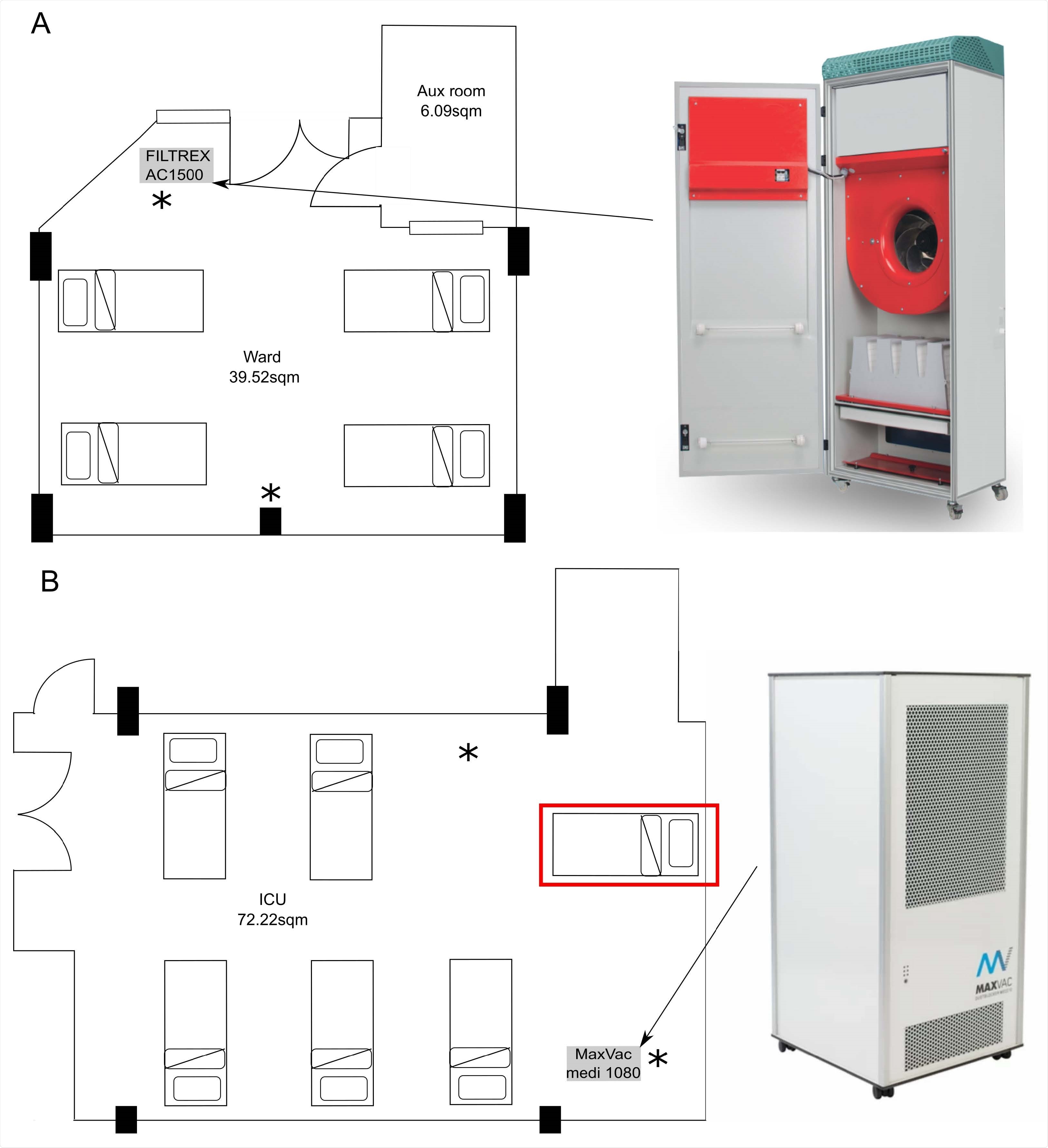
Location of the air filters and room layout. A) Layout of the room on the ‘surge’ ward with four beds. B) Layout on the ‘surge’ ICU with six beds including the addition of the additional bed to increase occupancy (labelled with rad box). Locations of the NIOSH air samplers indicated by *. The air filters were installed in the marked locations and set to operate at 1000 m3/hour. The rooms volumes are approximately 107 m3 and 195m3 respectively. Fresh air was not supplied or extracted in these areas.
Effectiveness of the air filter in the ward
In the first week, when the air filter was not active, SARS-CoV-2 could be detected on all five sampling days in both medium and large (>4μM particle size) particulate fractions, but not on the small (<1μM) particulate filter.
In the second week, when the air filter was switched on and run continuously, SARS-CoV-2 RNA was not detected in any of the sampling fractions. Thereafter, sampling was repeated with an inactive air filter. SARS-CoV-2 RNA was detected in medium and large particulate fractions on three out of five days of sampling, along with multiple viral, bacterial and fungal pathogens.
In contrast, when the air filter was operational, only yeast was detected. Additionally, microbial bioaerosols decreased significantly.
Effectiveness of air filter in ICU
Meanwhile, the ICU elicited limited evidence of airborne SARS-CoV-2 on weeks one and three (filter off) but detected SARS-CoV-2 RNA in a single sample in the medium particulate fraction on week two (filter on). Use of the air filtration device significantly (p=0.05) reduced microbial bioaerosols even in the ICU.
Discussion
Recent data from studies indicate that exertional respiratory activity—such as those in COVID-19 patients—increases the release of 1-4 μM respiratory aerosols. However, conventionally defined ‘aerosol-generating procedures’ such as high flow nasal oxygen and non-invasive ventilation reduce aerosol generation during exertion. This study concurs with such data, postulating that precautions may be more important in the wards.
The low burden of SARS-CoV-2 in ICU can be due to multiple factors – a higher level of aerosol PPE used, patients, being in later stages of the disease – where viral replication is less pronounced, higher viral loads in the lower rather than upper respiratory tract in critically ill patients and use of a respiratory device that reduces aerosol generation.
In the ICU, reduction in microbial bioaerosols with a functional air filtration system indicates that the device was equally effective.
While multiple building codes propose air filtration to reduce the transmission of airborne diseases, these have not been updated taking COVID-19 into consideration.
This presents the first report depicting the successful removal of airborne SARS-CoV-2 in hospital settings using combined air filtration and UV sterilization technology.
The observations confirm that air filtration devices may help in reducing the risk of hospital-acquired SARS-CoV-2.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
The removal of airborne SARS-CoV-2 and other microbial bioaerosols by air filtration on COVID-19 surge units Andrew Conway Morris, Katherine Sharrocks, Rachel Bousfield, Leanne Kermack, Mailis Maes, Ellen Higginson, Sally Forrest, Joannna Pereira-Dias, Claire Cormie, Timothy Old, Sophie Brooks, Islam Hamed, Alicia Koenig, Andrew Turner, Paul White, R. Andres Floto, Gordon Dougan, Effrossyni Gkrania-Klotsas, Theodore Gouliouris, Stephen Baker, Vilas Navapurkar, medRxiv, 2021.09.16.21263684; doi: https://doi.org/10.1101/2021.09.16.21263684, https://www.medrxiv.org/content/10.1101/2021.09.16.21263684v1
- Peer reviewed and published scientific report.
Conway Morris, Andrew, Katherine Sharrocks, Rachel Bousfield, Leanne Kermack, Mailis Maes, Ellen Higginson, Sally Forrest, et al. 2021. “The Removal of Airborne Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) and Other Microbial Bioaerosols by Air Filtration on Coronavirus Disease 2019 (COVID-19) Surge Units.” Clinical Infectious Diseases, October. https://doi.org/10.1093/cid/ciab933. https://academic.oup.com/cid/article/75/1/e97/6414657.