During the coronavirus disease 2019 (COVID-19) pandemic, healthcare resources for non-COVID care were minimized to accommodate and handle the increasing number of patients diagnosed with COVID-19.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
According to the World Health Organization (WHO), cardiovascular and cardiac diseases are the leading cause of death globally. Even before the pandemic, high mortality due to cardiovascular diseases majorly contributed to the slowdown of life expectancy gains in several Organization for Economic Co-operation and Development (OECD) member countries.
Amidst the COVID-19 crisis, the WHO drew attention to the impact of COVID-19 on healthcare services for patients with non-communicable diseases (NCDs), which were severe and involved multiple clinical areas, including cardiac diseases. Subsequently, cardiac care was considered the worst affected by the COVID-19 pandemic, thus making it challenging for the healthcare workers to continue cardiac care, as well as establish and maintain novel models of care alongside seeking ways to strengthen referrals and care pathways to avert worsened outcomes for patients with acute cardiac conditions.
Study design
In a recent review published on the medRxiv* server, a team of researchers analyzed 94 papers related to the delivery of healthcare services. This literature reported the varying degrees to which the COVID-19 pandemic has affected all phases of the hospital care pathways, including admission, diagnosis, treatment, outpatient care, and outcomes for patients with cardiac diseases across 109 OECD members countries.
To gather all the relevant data for the study, the researchers conducted extensive searches on the MEDLINE and Embase databases. With the help of a medical research librarian, the search strategy was improvized and adapted to both databases, who finally compiled a comprehensive search on March 17, 2021.
The final search strategy used the following keywords or search terms and their synonyms: COVID-19, pandemic, chronic disease, performance indicator, non-communicable disease, healthcare quality, healthcare delivery, healthcare utilization, and other closely related terms.
Studies using empirical data on the use of health services, studies describing health outcomes during the COVID-19 pandemic, cohort studies, case-control, case reports, systematic reviews, surveys, and meta-analyses were analyzed in the current study. Certain review articles were excluded, such as editorials and commentaries, prediction models, and clinical case reports.
Study findings
The study findings showed that hospital admission numbers dropped significantly across all included articles, although patients arrived later in the hospital in a worse clinical condition. There could be two possible explanations for this including an inclination towards healthcare avoidance caused by apprehension of getting infected with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) in the hospital, or an actual reduction in cardiac diseases during the pandemic due to reduced air pollution or changes in physical activity during the lockdown period.
Patients were discharged from the hospital after a short length of the stay due to the shortage of hospital beds or to minimize the risk of patients’ exposure to the virus. Many patients also canceled elective procedures and surgeries.
Consequently, there was a significant decrease in outpatient activity and a decrease in the number of diagnostic and treatment procedures. The reduction in outpatient care volume was due to performance indicators reporting on in-patient visits, which is already an underestimation of the actual outpatient care given in the hospitals.
Interestingly, the use of telehealth services and acute coronary syndrome (ACS) treatment pathway times increased. Together, these observations indicated that the hospital delivery of cardiac care was less accessible during the COVID-19 pandemic. Eventually, worse clinical outcomes and an increase in mortality rates were reported during the COVID-19 pandemic. These reported changes in mortality only reflected short-term mortality rates of up to 30 days.
The increased use of telehealth services showed that innovative measures were being taken during the pandemic to avoid the risk of SARS-CoV-2 infection and that health systems quickly adapted to reach out to patients with other means than in-person consultations. Although little is known about the quality of care provided by telehealth services, strengthening its use in the long term to provide continuity of care could be beneficial.
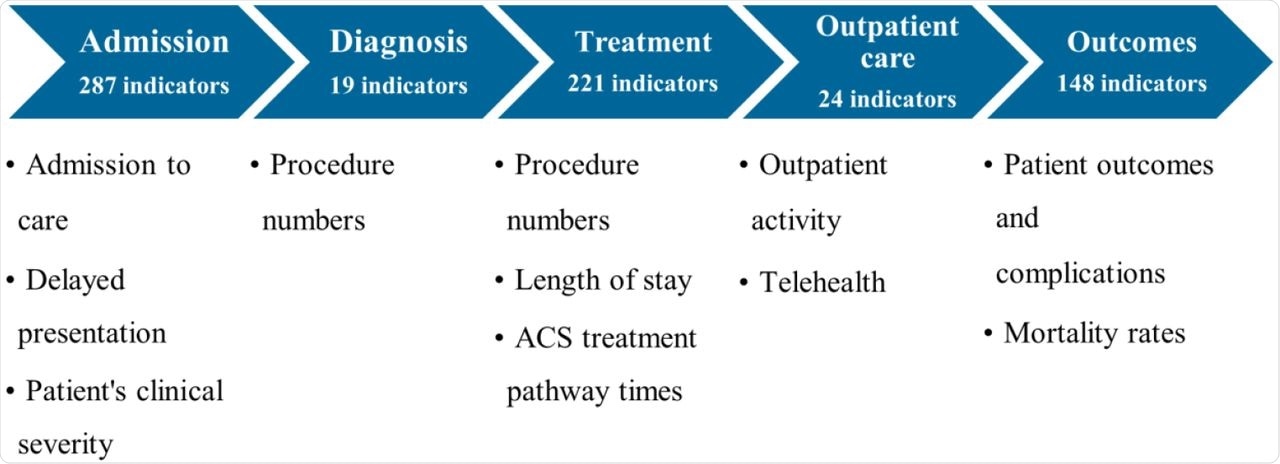 Categorization of indicators according to different phases of the hospital cardiac care pathway.
Categorization of indicators according to different phases of the hospital cardiac care pathway.
Study limitations
According to the authors, this is the first scoping review that outlines the impact of the COVID-19 pandemic on hospitals’ cardiac care pathways in OECD countries. As a scoping review, the current study included articles using different methodologies, indicators, indicators’ definitions, and comparison periods, with heterogeneous characteristics and indicators, thus making it hard to compare data reliably. Therefore, a systematic review with meta-analyses should also be performed.
The current study highlights the challenges faced by all divisions of the hospital care pathway for patients with cardiac diseases during the COVID-19 pandemic. The results indicate that these divisions faced immense pressure in continuing the hospital services delivery process for cardiac care during the pandemic. These results can help safeguard the continuity of care during other crises in the future and plan the recovery of care for patients with cardiac diseases.
Conclusions
To conclude, more research on the ways to monitor changes in hospital care systems during a pandemic is needed to guide the decisions of healthcare systems and policymakers during future crises. This would ensure the optimal use of existing health information infrastructure and continuing essential care, based on an international standardized set of indicators similar to the one suggested by the International Training Network for Healthcare Performance Intelligence Professionals (HealthPros) in July 2020. The current study recommends having a uniformly accepted set of clear definitions or indicators to use during future pandemics.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
de Lange, M., Carvalho, A. S., Fernandes, O. B., et al. (2021). The impact of the COVID-19 pandemic on hospital services for patients with cardiac diseases: a scoping review. medRxiv. doi:10.1101/2021.12.01.21267100. https://www.medrxiv.org/content/10.1101/2021.12.01.21267100v1.
- Peer reviewed and published scientific report.
Lange, Mats de, Ana Sofia Carvalho, Óscar Brito Fernandes, Hester Lingsma, Niek Klazinga, and Dionne Kringos. 2022. “The Impact of the COVID-19 Pandemic on Hospital Services for Patients with Cardiac Diseases: A Scoping Review.” International Journal of Environmental Research and Public Health 19 (6): 3172. https://doi.org/10.3390/ijerph19063172. https://www.mdpi.com/1660-4601/19/6/3172.