Millions of women throughout the world struggle with infertility. Oxidative stress (OS) plays a vital role in the pathophysiology of female infertility.
OS occurs due to an imbalance between the formation of antioxidant defenses and reactive oxygen species (ROS), subsequently leading to cellular damage. In a recent Antioxidants study, scientists review existing literature to assess the relationship between OS and female infertility.
 Study: The Silent Threat to Women’s Fertility: Uncovering the Devastating Effects of Oxidative Stress. Image Credit: Tinydevil / Shutterstock.com
Study: The Silent Threat to Women’s Fertility: Uncovering the Devastating Effects of Oxidative Stress. Image Credit: Tinydevil / Shutterstock.com
The effect of OS on female fertility
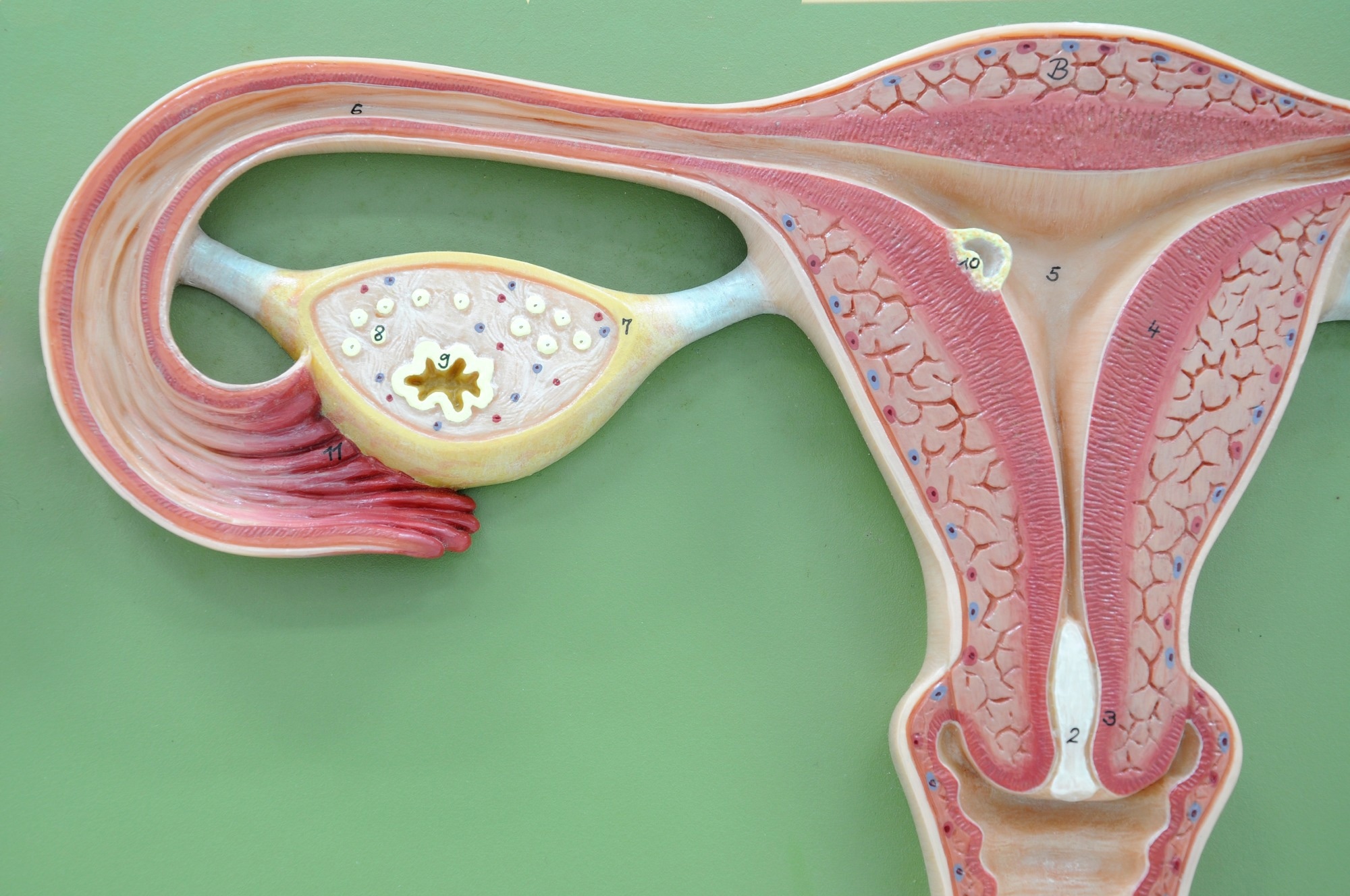
The key components of the female reproductive system are the fallopian tubes, ovaries, cervix, and uterus. Oocytes, granulosa cells, cumulus cells, and endometrial cells are crucial sources of ROS in the female reproductive system. ROS induce a chain reaction that directly affects DNA, RNA, lipids, proteins, and carbohydrates in the cell.
Previous studies have shown that an exhausted antioxidant system negatively affects the female genital tract. OS damages oocytes and follicles in the female reproductive system, thereby disrupting implantation, damaging the endometrium, and affecting endocrine function.
Cell damage can trigger OS, which leads to lipid peroxidation, membrane disruption, loss of adenosine triphosphate (ATP) energy, and protein formation disorders. Lipid peroxidation reduces the fluidity and permeability of the oocyte membrane, which ultimately limits its ability to be fertilized. Additionally, protein oxidation caused by OS inhibits oocyte development.
Several studies have indicated that OS interferes with embryonic development by altering gene expression. Furthermore, ROS-induced DNA damage restricts embryonic development by producing chromosomal abnormalities. OS also contributes to implantation failure.
OS-induced reproductive impairments lead to altered ovulation patterns, oocyte maturation, and steroidogenesis, each of which accelerates the natural process of apoptosis in granulosa cells. These conditions can lead to the development of polycystic ovarian syndrome (PCOS), endometriosis, and unexplained infertility, as well as hypertension, preterm birth, and intrauterine growth restriction (IUGR).
Maternal age plays a significant role in female infertility. By the age of 44, women experience reduced estrogen levels, thus implying reduced protection against oxidative damage to the endometrium.
In these situations, hormone replacement therapy (HRT) could be used to alleviate the effect of OS. Paternal age also influences fertility by negatively affecting gamete and semen quality and causing oxidative DNA damage.
Oxidative abnormalities have been associated with negative lifestyle behaviors such as alcohol consumption, recreational drug use, and smoking, as well as obesity and malnutrition. Endocrine-disrupting chemicals (EDCs) like phthalates also affect female reproduction by inducing OS.
Obesity affects female fertility by altering hormonal balance and menstrual cycles. The production of ROS due to obesity affects vasodilation and blood flow to reproductive organs, which may affect fertility. The hormonal imbalances induced by obesity also impair ovulation patterns and contribute to the development of PCOS development, which leads to female infertility.
The underlying mechanisms that link obesity with female infertility are complex and multifactorial. Some mechanisms that have been implicated in this relationship include insulin resistance, inflammation, and alterations in adipokine secretion. Malnutrition also affects female reproduction, as malnourished women are more likely to have impaired endothelium-dependent vasodilation, which induces OS.
Therapies to mitigate OS in the female reproductive system
Three different approaches are currently available to treat OS-induced damage to the female reproductive system, which include antioxidants, lifestyle modification, and drug interventions. Lifestyle modifications, including a healthy diet, stress management, and regular exercise, can reduce the adverse effects of OS.
Mitochondrial function was found to be improved through regular physical activity, which ultimately reduces OS levels and imparts a positive effect on fertility. Maintenance of healthy body weight through regular exercise and a balanced diet also supports fertility and reproductive health.
An antioxidant-rich diet containing fruits and vegetables can limit the production of ROS and prevent cellular damage. Vitamins A, C, and E, as well as bioactive compounds like polyphenols, are also well-known antioxidants found in many fruits and vegetables.
Endogenous antioxidants such as glutathione and glutathione peroxidase (GPx) maintain the levels of exogenous antioxidants like vitamins A, C, and E. Thus, a well-balanced diet with sufficient exogenous antioxidants maintains the overall antioxidant balance needed to stabilize ROS.
Antioxidant supplements have been shown to improve endometrial blood flow, reduce insulin resistance and hyperandrogenism, as well as support prostaglandin production and steroidogenesis. Each of these conditions facilitates a woman’s ability to conceive.
A previous study has indicated that antioxidant intake increases embryo implantation rates, improves oocyte and follicle quality, and reduces pregnancy loss in women undergoing assisted reproductive technology (ART). A recent study reported improvements in pregnancy rates in women using ART therapies and vitamin E supplementation.
One of the key antioxidants that have a major role in infertility is coenzyme Q10 (CoQ10). CoQ10 increases ovarian reserve, ovulation rates, and oocyte quality in women who undergo ART therapy.
Vitamin C supplementation also improves fertility in women with PCOS. Anti-inflammatory and antioxidant drugs, such as metformin and melatonin, can also be used to reduce OS.