The researchers analyzed different stages of CSU by examining the shape and pattern of these skin eruptions. They employed three key methods: mathematical modeling to simulate the condition, laboratory experiments conducted outside living organisms (in vitro) to observe cellular behaviors, and the analysis of clinical data gathered from patients.
This combined approach helped them better understand the various pathological states of CSU.
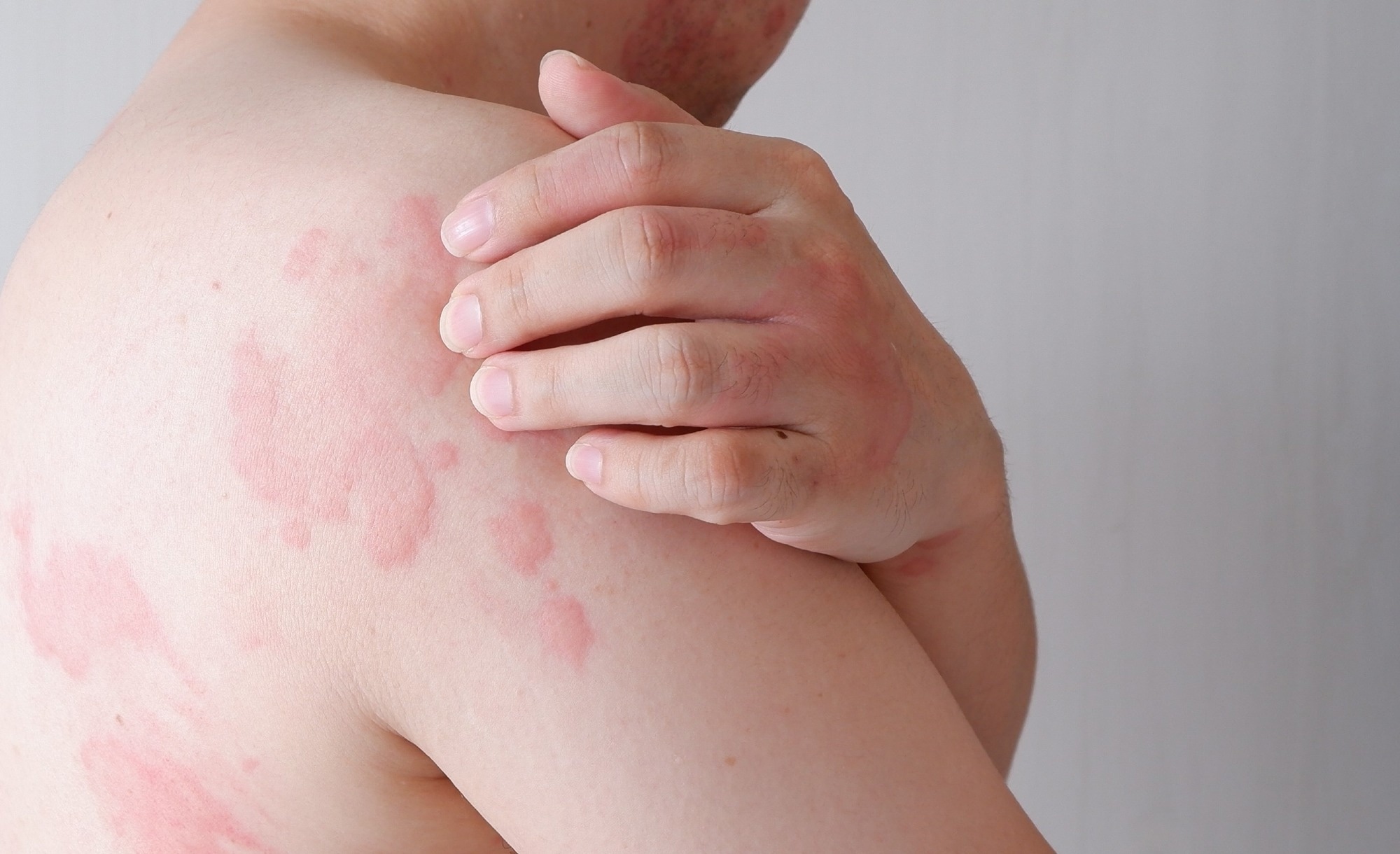 Study: Mathematical-based morphological classification of skin eruptions corresponding to the pathophysiological state of chronic spontaneous urticari. Image Credit: wisely/Shutterstock.com
Study: Mathematical-based morphological classification of skin eruptions corresponding to the pathophysiological state of chronic spontaneous urticari. Image Credit: wisely/Shutterstock.com
Background
Currently, there are no experimental animal models for human skin diseases. Thus, the mechanism governing their pathogenesis in vivo remains unclear, which, in turn, has made it challenging to find and establish curative treatments for diseases such as CSU.
Nonetheless, red-colored skin eruptions, known as wheals, characterize CSU and are of various shapes.
They appear and disappear daily for up to weeks or decades, severely impacting the quality of life of affected CSU patients. Yet, the causes and consequences of CSU pathology remain largely understudied.
About the study
In the present study, researchers collected wheal images of 105 CSU patients who sought skin treatment at Hiroshima University Hospital between January 1, 2000, and April 15, 2022.
Six allergic skin disease specialists (dermatologists) classified the morphology of wheels of each patient into two main classes, boundary and area patterns, and further into five specific patterns, viz., broken-annular, annular, circular, geographic, and dot patterns, as seen in the in silico experiments.
Based on the eruption geometry (EGe) criteria, dermatologists calculated the reliability SB, that is, the number of doctors who chose the patient sample as one of the types in the EGe criteria divided by the number of dermatologists (=6), derived using the vote-counting method.
To obtain results with higher reliability, they also calculated reliability (SS) defined as SS = [SB of type selection] × [SB of class selection].
The network structure of this study focused on the four factors playing a key role in the in vivo pathophysiological network of CSU.
These were (i) concentration of histamine released from basophils ([HB]), (ii) TF expression on vascular endothelial cells ([TF]), (iii) coagulation factors leaked from blood vessels ([C]), and (iv) histamine released from mast cells ([HM]). Furthermore, this model integrated the intravascular and extravascular dynamics observed in CSU.
Results
The new mathematical model for chronic spontaneous urticaria (CSU) developed in this study successfully categorized CSU eruptions into five distinct groups. Each group is characterized by unique signatures in histamine levels, basophils, mast cells, and coagulation factors.
The model's classification accuracy reached 87.6% agreement with the assessments of six dermatologists. This level of agreement was statistically verified to be significant and not due to random chance, as evidenced by the P-value.
Additionally, the data, marked by high reliability (denoted as SS), indicated that geographic and circular eruption patterns were more common compared to boundary patterns. This suggests that area patterning is a prevalent molecular mechanism found across various patients and types of urticaria.
Furthermore, network analysis revealed that while the coagulation status likely determines the boundary pattern of wheals, spontaneous histamine release from mast cells is a factor in wheals' diverse size and outline.
The study found that tissue factor (TF) and mast cells had a notably higher association with the networks studied, suggesting that their behavior could influence the shapes of chronic spontaneous urticaria (CSU) eruptions.
It was also observed that the degradation or activation of TF played a significant role in defining the features of boundary and area patterns in CSU eruptions.
The research highlighted a specific association between high TF activation and the area pattern (as opposed to the boundary pattern) in their theoretical analysis. This finding leads to a recommendation for future studies to validate this association experimentally, particularly through the measurement of coagulation biomarkers like PF1 + 2 and D-dimer.
Additionally, the study suggests that the relationship of the wheel pattern in CSU to biomarkers indicative of autoimmunity—which activate mast cells and basophils—requires further investigation.
The authors also noted that the dynamics of intracellular gap formation, influenced by the TF switch, are crucial in the development of eruption patterns and the onset of wheal formation.
Lastly, the study proposes that spontaneous histamine release from mast cells might be a key factor differentiating between CSU's broken and annular annual patterns.
Conclusions
In this study, researchers followed a stepwise approach to extract the geometrical properties of skin eruptions from CSU patients, link these to the parameter values of the conceptual CSU mathematical model, and structurally prove all sequential pathophysiological steps involved in the CSU development in silico.
The study model also revealed that TF and histamine released from mast cells were critical in generating diverse eruption patterns among CSU patients.
Thus, in the future, EGe criteria could prove to be a great tool of practical application for clinicians determining eruption patterns of CSU patients.
Moreover, this mathematical modeling approach may apply to a variety of other skin diseases characterized by the formation of geometric morphology, such as psoriasis, erythema gyratum repens, tinea corporis, erythema multiforme, and autoimmune bullous disease.
Journal reference:
-
Matsubara, D., Yanase, Y., Kunieda, T., Takahagi, S., & Hide, M. (2023). Mathematical-based morphological classification of skin eruptions corresponding to the pathophysiological state of chronic spontaneous urticaria. Communications Medicine, 3(1), 1-11. doi: https://doi.org/10.1038/s43856-023-00404-8. https://www.nature.com/articles/s43856-023-00404-8