Fifth disease or erythema infectiosum (EI) is a typically mild disease caused by the parvovirus B19. This virus may be responsible for a spectrum of disease of which EI is the mildest. In susceptible individuals, it may cause joint pain, hydrops in the fetus and even fetal death, and severe anemia. Its disease range may be still undiscovered as the virus is being found to be present in many conditions which are not causally linked to it so far.
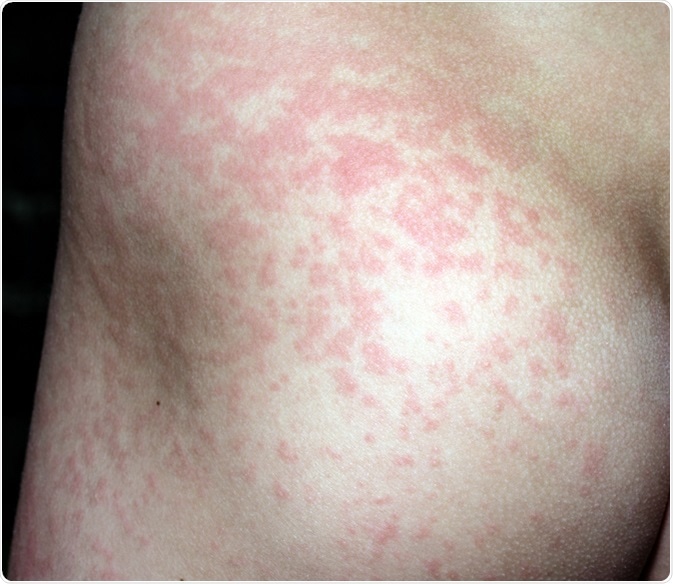
The rash from fifth disease on a child. Image Credit: weakiva / Shutterstock
Parvovirus B19 is a common virus and can cause community-wide infection, irrespective of gender, age, socioeconomic status, ethnicity or country. In healthy adults, B19 causes EI as well as acute-onset joint pain which symmetrically affects multiple joints.
In individuals who have a hemolytic disease, the known tropism of B19 to the precursor cells in the red blood cell series in the bone marrow leads to failure of red cell production and temporary severe anemia, called transient aplastic anemia or crisis.
If an individual is immunocompromised, and the virus is not cleared from the body in a timely fashion, the persistent B19 infection may lead to pure red cell aplasia or to chronic anemia.
In fetuses too, the inability of the immature immune system to eliminate the virus causes severe infection and destruction of the erythroid precursors. The result is fetal death, severe edema of the fetus (hydrops fetalis) due to cardiac failure, or anemia at birth.
The virus usually spreads by air droplets which are breathed in, and the greatest transmission is during the week before symptoms set in. The B19 virus has an incubation period between 4 and 21 days.
Erythema infectiosum
The symptoms of fifth disease in children include fever, red rash over the cheeks as if they had been slapped, and after 4-14 days, the onset of a network-like rash all over the body which is itchy and can last for up to 3 weeks.
The preceding or prodromal symptoms are often so mild as to be overlooked, and include fever, headache, running nose and nausea. The rash consists of pink macular lesions with central fading that causes the typical lacy appearance. The rash is often short-lived but may recur, perhaps after exposure to sunlight or heat. Sometimes the patient complains of pruritus, or scaling or vesiculation of the affected skin.
In adults, the disease does not always cause a rash but does result in arthropathy much more frequently (30% and 60% in males and females respectively). This is especially seen among middle-aged females, is acute in onset, and symmetrical, involving more than one joint. The following peripheral joints are most often affected: the knuckles (75%), knee joints (65%), wrists (55%), and ankles (40%), but without any erosive lesions of the joint. Half of the patients with chronic joint disease due to long-term B19 infection are diagnosed with rheumatoid arthritis as per the American Rheumatoid Association criteria. This resolved without permanent swelling or mobility restriction of the affected joints and hence B19 infection is not considered a precursor of chronic inflammatory arthritis at present.
While only about one in ten infected children has joint pain, almost one in five children who had arthritis of recent onset tested positive for recent B19 infection (by IgM antibodies).
The rash and the joint manifestations are probably due to immune complex deposition in various tissues. Both are prone to wear off spontaneously.
Complications of Fifth Disease
While EI itself is self-limited, some groups of individuals cannot tolerate the temporary disruption of red cell synthesis that occurs at this time.
These include:
- Those with blood disorders associated with more rapid red cell destruction (hemolytic disorders) such as hereditary spherocytosis and sickle cell disease require a high rate of red cell production to compensate. In this group, the B19 infection may precipitate severe anemia or even transient aplastic anemia.
- Fetuses in the womb have a 30% risk of infection transmitted from the mother, and this leads to infection of the fetal liver where most fetal red blood cells are formed between 11-23 weeks, causing severe anemia and possibly myocarditis, and resulting in heart failure. This condition is called (non-immune) hydrops fetalis, and 5-9% of fetuses die in utero due to this condition, especially in the second trimester (hepatic phase of red blood cell formation). While non-immune hydrops fetalis is a rare condition, 15-20% of these patients owe it to B19 infection.
- Immunocompromised individuals, such as those with AIDS, may develop a persistent B19 infection.
- Children may develop subclinical or obvious drops in their platelet count. This can cause an acute and drastic drop in the platelet count. The condition was found to respond well to immunoglobulin but not to high doses of steroids, which led to chronic thrombocytopenia. The mechanism is suppression of the bone marrow megakaryocytes by the NS1 protein, though these are not tropic for the virus.
- Transient erythroblastopenia of childhood, or TEC, is seen in children of 3-4 years with a low red cell and reticulocyte count, and whose bone marrow shows a reduction in erythroid precursors.
- Immune-mediated neurological symptoms, such as seizures, have been reported in patients with B19 antibodies.
- Chronic pure red cell aplasia may result from B19 infection in immunocompromised patients whose defect lies in bone marrow insufficiency, leading to failure of neutralizing antibody reactions to clear the virus from the blood. Some such conditions include acute lymphatic or myeloid leukemia, chronic myeloid leukemia, lymphoblastic lymphoma, Wilm’s tumor, HIV, and chemotherapy.
Further Reading
Last Updated: Oct 9, 2018