Skip to:
Acute respiratory distress syndrome (ARDS) is a potentially fatal condition where the lungs cannot provide enough oxygen to the body's vital organs.
The condition, otherwise known as acute lung injury, adult respiratory distress syndrome, increased-permeability pulmonary edema, and noncardiogenic pulmonary edema, is often a complication of another disease. The condition may affect adults and children, often characterized by fluid buildup in the small air sacs or alveoli in the lungs. The fluid accumulation makes it hard for oxygen to get into the bloodstream.
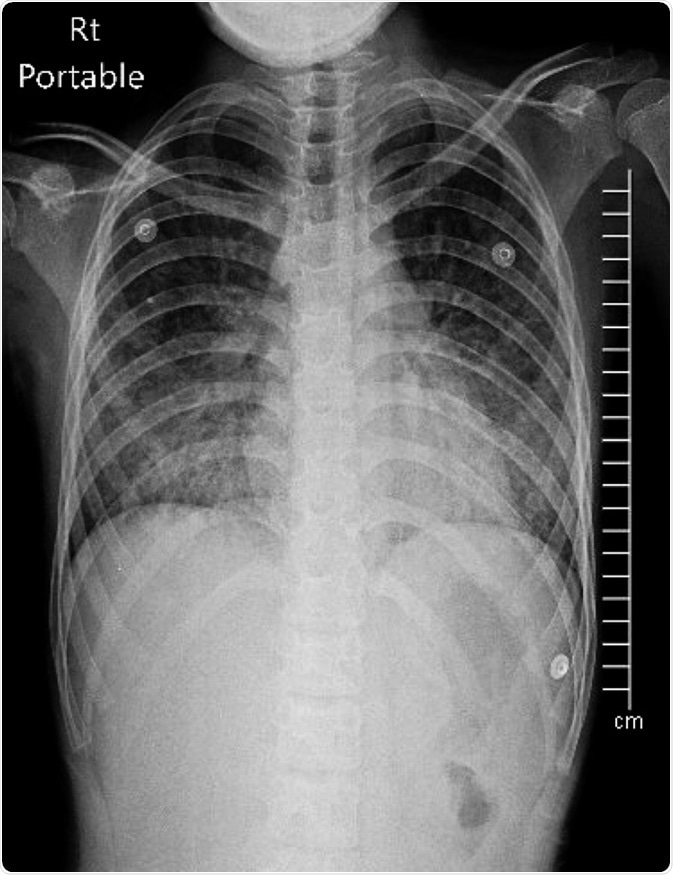
Acute respiratory distress syndrome on Chest X-ray PA upright. Image Credit: Chalie Chulapornsiri / Shutterstock
What causes ARDS?
The most common causes of ARDS are pneumonia, sepsis, aspiration, and severe trauma. The mortality rate is from 40 to 50 percent.
Severe pulmonary or systemic infections, following trauma, severe burns, pancreatitis, near-aspiration events, drug reactions, multiple blood transfusions, inhalation injuries, and infection are common causes of ARDS. ARDS is mainly a complication of another illness.
How does ARDS form?
The main mechanical cause of ARDS is when fluid leaks from the capillaries in the lungs into the alveoli. Typically, a protective membrane wards of fluid from entering the air sacs. However, due to a severe injury or illness, the membrane suffers damage, leading to fluid leakage.
Sepsis is a life-threatening condition caused by the body’s response to an infection, causing widespread infection of the bloodstream. Severe pneumonia may also cause ARDS. Other causes include inhalation of vomit or near-drowning episodes, head, chest or other significant injuries, and severe burns.
Signs and symptoms of ARDS
ARDS symptoms typically appear between one and three days after the trauma, injury, or severe pneumonia. It may become life-threatening when there is widespread inflammation of the lungs, which may begin in just one lung, but eventually, it would affect both.
When the fluid accumulates in the alveoli, they lose their ability to oxygenate the blood and eliminate carbon dioxide. Patients with ARDS may start having severe shortness of breath, muscle fatigue, general weakness, low blood pressure, rapid and shallow breathing, drowsiness or confusion, feeling faint, dry and hacking cough, headaches, and fever.
In severe cases, the lungs may become heavy and unable to expand, with patients requiring mechanical ventilation due to respiratory failure. With ARDS, other organs may fail to work properly, leading to multiorgan failure, affecting the heart, kidneys, liver, bloodstream, and brain.
Flu and Acute Respiratory Distress Syndrome (ARDS) - Mayo Clinic
Related conditions
Symptoms of other disorders can be similar to those of ARDS, or in most cases, these conditions lead to ARDS. Severe acute respiratory syndrome (SARS) is a respiratory disease first reported in China in 2002. A coronavirus caused the SARS outbreak, which starts with body aches and mild respiratory symptoms. Between two and seven days, SARS patients often develop a severe cough and difficulty breathing, which may then lead to ARDS.
Other conditions caused by coronaviruses may also cause ARDS, such as Middle East Respiratory Syndrome (MERS) and the currently spreading SARS-CoV-2 coronavirus disease (COVID-19). Just like SARS, these conditions begin with mild respiratory symptoms that may progress to ARDS.
.jpg)
Novel Coronavirus SARS-CoV-2: This scanning electron microscope image shows SARS-CoV-2 (round gold objects) emerging from the surface of cells cultured in the lab. SARS-CoV-2, also known as 2019-nCoV, is the virus that causes COVID-19. The virus shown was isolated from a patient in the U.S. Credit: NIAID-RML
Another cause of ARDS is pneumonia, which is the infection of the lungs. The common signs and symptoms include cough, fever, sputum production, chills, and fluid accumulation in the space surrounding the lungs. Bacteria, viruses, and other pathogens may cause infection of the lungs.
Diagnostic tests for ARDS
In patients with ARDS, doctors may recommend diagnostic tests to determine the severity of the condition, including a chest X-ray, sputum culture to identify the pathogen involved, arterial blood gases, and blood culture.
Oxygen levels are monitored, and the doctors will note for the presence of respiratory distress. In chest X-rays, patients with ARDS may show fluid-filled air sacs, while upon auscultation, the doctor will notice “wet” breathing sounds.
Treatment for ARDS
The most common treatment for ARDS is oxygen therapy to provide the needed oxygen for the organs to function correctly. However, the recommended treatment is addressing the cause of ARDS. In some cases, patients may require mechanical ventilation and admittance to an intensive care unit (ICU). The prognosis of the condition depends on the treatment of the underlying disorder, such as pneumonia or infection.
Complications may also arise from ARDS, including nerve and muscle damage in those who survive the condition. However, in some cases, patients may die as a result of the underlying condition, rather than ARDS itself.
ARDS can develop at any age, including older people and children. In treating ARDS, supplying oxygen is the primary way to address the problem while doctors figure out how to manage the underlying condition. Treatments help prevent serious or fatal complications, such as organ failure and organ damage.
Diffuse alveolar damage (DAD)
Diffuse alveolar damage (DAD) is the lesion that underlies and is responsible for most acute respiratory distress syndrome (ARDS). DAD can follow a large number of precipitating events, including infection, sepsis, trauma, shock, toxic inhalants, drug toxicity, burns, and others. DAD begins with an acute exudative phase characterized by the presence of interstitial and intra-alveolar edema, hyaline membranes, and interstitial inflammation. The mortality rate is high. In those patients who survive, there may be a restitution of normal lung structure and function. Some survivors develop chronic fibrotic lung disease of varying severity.

Diffuse alveolar damage (DAD) The lung on the left is diffusely consolidated and pale in appearance. The lung on the right is from another case; it exhibits no significant abnormality and is included for comparison. Credit: Yale Rosen / Flickr
References:
Further Reading
Last Updated: Jan 20, 2021