Researchers in Europe have found no evidence to support previous reports that the use of drugs that target the renin-angiotensin-aldosterone system (RAAS) increases susceptibility to coronavirus disease 2019 (COVID-19). The research is published in the European Heart Journal.
The causative agent in COVID-19 - severe acute respiratory syndrome coronavirus (SARS-CoV-2) - uses angiotensin-converting enzyme 2 (ACE2) to infect host cells.
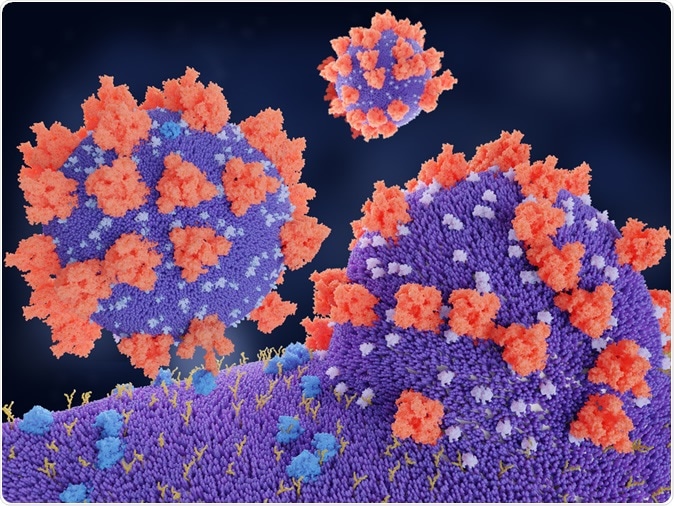
Coronaviruses penetrating in human cell. Binding of the coronavirus spike protein(red) to an ACE2 receptor (blue) leads to the penetration of the virus in the cell. Illustration Credit: Juan Gaertner / Shutterstock
Concerns have therefore arisen that the use of drugs that target the RAAS, such as angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs) may increase blood levels of ACE2 and the risk of COVID-19 among patients with cardiovascular disease.
However, the current study, which looked at ACE2 blood concentrations in samples taken from thousands of heart failure patients across eleven European countries, found that patients taking these drugs did not have higher blood levels of ACE2.
"Our findings do not support the discontinuation of these drugs in COVID-19 patients as has been suggested by earlier reports," says study leader and professor of cardiology, Adriaan Voors, from the University Medical Center (UMC) Groningen, The Netherlands.
The researchers also found that men had higher blood levels of ACE2 than women, which they say could account for why men are more susceptible to death from COVID-19.
What the study cannot confirm
However, the researchers acknowledge that they did only measure ACE2 levels in plasma and not the concentration in tissues such as lung tissue.
"High levels of ACE2 are present in the lungs and, therefore, it is thought to play a crucial role in the progression of lung disorders related to COVID-19," says Voors.
The study also does not provide conclusive evidence on the impacts RAAS inhibitors have among patients with COVID-19 since the study was confined to patients with heart failure who did not have COVID-19.
What did the study involve?
The study included an index cohort made up of 1,485 men (average age 69 years) and 537 women (75 years), which aimed to test the team's hypotheses, and a validation group made up of 1,123 men (74 years) and 575 women (76 years).
The team assessed various factors that can influence ACE2 levels, including the use of ACE inhibitors, ARBs, and mineralocorticoid receptor antagonists (MRAs), the presence of chronic obstructive pulmonary disorder, and any history of a coronary artery by-pass graft or atrial fibrillation.
What did the study find?
Among the index participants, there was no association between ACE2 plasma levels and the use of any of the three drugs. Among those in the validation group, the use of ACE inhibitors and ARBS was in fact, associated with decreased ACE2 levels. However, the use of MRAs was weakly associated with higher ACE2 levels.
The researchers say that, to the best of their knowledge, theirs is the first comprehensive study investigating the link between drugs targeting the RAAS and plasma ACE2 levels among cardiovascular patients.
"We found no evidence that ACE inhibitors and ARBs were linked to increased ACE2 concentrations in plasma. In fact, they predicted lower concentrations of ACE2 in the validation cohort, although we did not see this in the index cohort," says Voors.
He adds that it is not clear what the effects of using MRAs are on ACE2 levels since the weak association observed in the validation group was not observed in the index group:
"Our findings do not suggest that MRAs should be discontinued in heart failure patients who develop COVID-19. They are a very effective treatment for heart failure, and the hypothetical effects on viral infection should be weighed carefully against their proven benefits."
Men had higher levels of ACE2 than women
The study found that being male was the factor most strongly associated with a raised ACE2 level.
Since the concentration of ACE2 is particularly high in the testes, the team thinks this may explain why levels are higher among men and why susceptibility to COVID-19 is greater among men.
"These data might explain the higher incidence and fatality rate of COVID-19 in men, but do not support previous reports suggesting that ACE inhibitors or ARBs increase the vulnerability for COVID-19 through increased plasma ACE2 concentrations," concludes the team.
In an associated editorial, Gavin Oudit (University of Alberta, Canada) and Marc Pfeffer (Harvard Medical School, USA) say: "When faced with the rapidly expanding COVID-19 pandemic and in the absence of definitive data, the results of Sama et al obtained in heart failure patients in the pre-COVID-19 period offer supporting evidence to continue ACE inhibitors or ARBs in patients at risk for SARS-CoV-2 infection."
Source:
Journal reference: