Every day we are inching towards a world where we do not have antibiotics that work due to bacterial antibiotic resistance.
It threatens so many parts of modern healthcare, from treating everyday infections to conducting successful surgery and cancer therapies.
We choose to research antibiotic discovery to try and stop this happening.
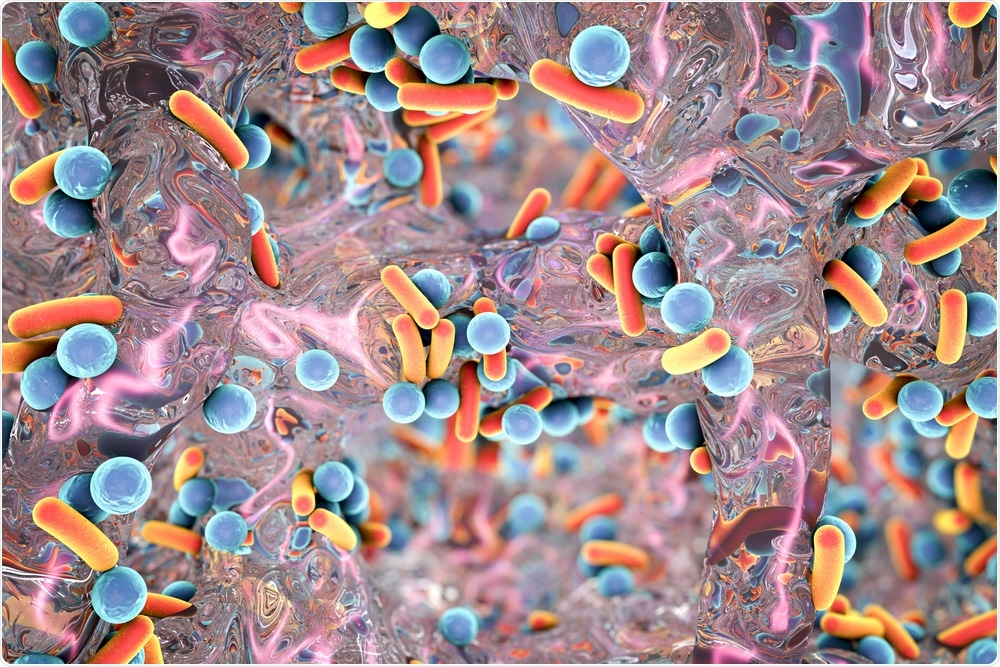
Image Credit: Kateryna Kon/Shutterstock.com
Why is increasing antibiotic resistance a challenge to scientists?
Bacteria are alive. They respond to the environment and evolve to survive, and their survival is based on beating our drugs. It is like a never-ending battle between our drugs and the bacteria.
How does bacteria’s biofilm make treating infections with antibiotics harder?
There are a few reasons. Firstly, a biofilm acts as a physical barrier that our drugs need to get through.
Secondly, inside the biofilm, the bacteria can share nutrients and resources. Finally, some of the bacteria exhibit a persistence phenotype, which effectively means they ‘go to sleep’. And as a lot of our drugs only work when the bacteria is ‘awake’, these bacteria survive.
Then once the antibiotic is no longer there the bacteria ‘wake up’ and establish the infection again.
What are biofilm-associated infections?
Biofilms are sticky aggregates of bacteria – the individual bacteria cover themselves in a protective matrix of polysaccharides, proteins, and DNA. Although the term ‘biofilm’ is not very well known, everyone is likely to have come into contact with one, as they are really common. It is thought that 75% of human infections have a biofilm established in them.
For example, if you have ever had a cut and it becomes all gooey and yellow – that is a cut where a biofilm of bacteria has made a home. They pose a serious issue in chronic wounds common in diabetic ulcers, or catheter-associated infections.

Image Credit: wirakorn deelert/Shutterstock.com
What are natural antimicrobials and what were they used for?
Natural antimicrobials are things that come from nature and can kill bacteria, fungus, parasites, and viruses. Throughout history, they have been used for a variety of different infections, including infected eyes, cuts and wounds, and malaria.
Although it takes a long time to make sure any drug is safe and effective to use, there are a few examples of natural antimicrobials being used today in modern medicine.
Honey, for example, is used by the UK National Health Service to treat burn wound infections. Another one is the antimalarial drug artemisinin, which comes from the plant wormwood (Artemisia annua).
Can you describe how medieval methods using natural antimicrobials could help fill the antibiotic discovery gap?
We do not have enough potential new antimicrobial drugs in the pipeline and looking into natural products could be a really good source.
Interestingly, many medieval remedies used mixtures of several ingredients, and we think this could be very informative for researchers: perhaps mixtures of different natural products, instead of single molecules, are the key to making more effective preparations.
You reconstructed a medieval remedy known as Bald’s eyesalve to investigate its antibacterial activity. What did you discover?
We have looked at bacteria in two forms, as individual cells (planktonic) and as sticky biofilm communities. Looking at planktonic bacteria is quicker and easier but it is not the most realistic, as when we have an infection the bacteria tend to form biofilms. These biofilms protect the bacteria and make them much harder to kill.
We have shown that Bald’s eyesalve can kill both planktonic cultures and biofilms of different bacteria including S. epidermidis (common in catheter infections), A. baumannii (common in war wounds), S. maltophilia (respiratory infections) and S. aureus (including the superbug MRSA).
The key thing we have shown is that while garlic alone can kill the planktonic bacteria easily, it does nothing against biofilms.
In fact, if you take away any one of Bald’s eyesalve’s ingredients you lose some of the activity against biofilms. This shows that every ingredient is doing something to contribute to the activity against these tricky biofilms.
Do you believe that by using natural remedies, we could help to tackle the problem of antibiotic resistance?
Most of our current drugs ultimately come from natural sources – mainly plants and fungi. And some of these natural sources have been used in medicine throughout history and in so many different cultures.
While a lot of historical and traditional remedies are likely to be placebos, or possibly even harmful, the fact that some have already led to drug discovery makes it hard to believe that none of the unexplored ones will have any scientific value.
We fully expect some of the remedies to just be folklore or placebo but hope that some of them may be an untapped source of novel antimicrobial mixtures.
Why is it important to look at combining these natural products, as opposed to looking at single compounds?
We are proposing that the mixture is more powerful than one single component. Often natural remedies are divided up into individual parts and tested on planktonic cultures (free-floating bacteria that are susceptible to the environment).
Hundreds of antimicrobial compounds have been identified this way but few of them show good activity against biofilms, and most of the time, compounds that look promising in the lab fail to make their way to the clinic.
Our work has shown that the mixture as a whole is more potent. If we had focused on separating up the mixture, we would have focused on garlic, which when we tested it later on biofilms would not have been active anymore.
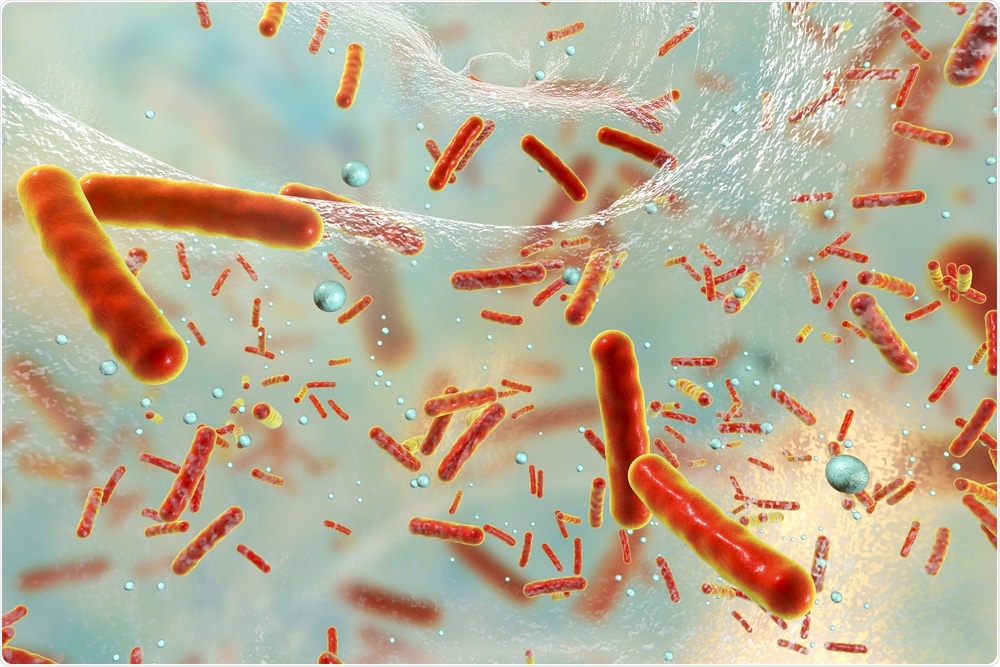
Image Credit: Kateryna Kon/Shutterstock.com
What are the next steps in your research into natural antimicrobials?
The two next steps for Bald’s eyesalve are first, to understand exactly what compounds make it antibacterial, and second, to continue our work on checking that this mixture is safe for human use.
We are also working on other natural remedies, and we hope to test these in a similar way to how we have investigated Bald’s eyesalve.
Where can readers find more information?
About Jess Furner-Pardoe_Bio.jpg)
I am in the 2nd year of my PhD focusing on understanding the chemistry of complex historical remedies.
About Dr. Freya Harrison
I am an Associate Professor of Microbiology at the University of Warwick. My team focusses on understanding the biology of bacterial biofilms in chronic infections and finding new ways to disrupt them._Bio.jpg)
We are especially interested in making more accurate lab models of biofilms in lung and wound infections, without using live animals, and in using these to explore possible new antibiofilm treatments. I also helped to found the Ancientbiotics consortium, which seeks to study, reconstruct, and test historical infection remedies.
About Dr. Blessing Anonye
I am a Lecturer in Medical Microbiology in the School of Medicine, University of Central Lancashire, Preston, and also a Visiting Research Fellow at the University of Warwick.
I am generally interested in the study of pathogens, antimicrobial resistance, and understanding the gut microbiota in health and disease._Bio.jpg)
I am particularly fascinated by research on how products from nature could potentially be used as alternatives to traditional antimicrobials.