Coronavirus disease 2019 (COVID-19) is caused by severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2), a novel RNA virus part of the coronavirus family. SARS‐CoV‐2 has a relatively long incubation period compared to other coronaviruses. COVID-19 emerged in Wuhan, China, in late 2019 and spread across the globe, progressing into a full-fledged pandemic causing significant morbidity and mortality in over 200 nations so far.
In the initial stages of SARS‐CoV‐2 infection, symptoms such as dry cough, fever, myalgias, and gastrointestinal symptoms are seen in most patients, while some experience a temporary loss of smell and taste. As the infection progresses, patients experience breathing trouble, neutrophilia, coagulation abnormalities, and rarely, neurological symptoms. Patients with fatal SARS-CoV-2 infection can experience acute respiratory distress, myocardial discomfort, stroke, and multiorgan damage during the final stages.
SARS-CoV-2 infection causes downregulation of tissue ACE2
More and more studies are suggesting that COVID-19 causes severe endothelial inflammation along with lung and heart complications. SARS-CoV-2 binds to the catalytic site of membrane-bound angiotensin-converting enzyme 2 (ACE2) for entry to the cell, which causes downregulation of ACE2 in tissues. Recently, researchers from the University of Melbourne and Burnet Institute, Australia, reported that the downregulation of cardiac ACE2 is linked to increased plasma ACE2 activity. This study is summarized in a preprint paper published in medRxiv.*
In this observational study involving patients who have recovered from COVID-19, the team hypothesized that SARS-CoV-2 infection is associated with ACE2 shedding from cell membranes and increased activity of plasma ACE2 receptors.
The researchers measured the catalytic activity of plasma ACE2 with the help of a validated and sensitive quenched fluorescent substrate-based assay in a study cohort comprising 18-year-old Australians (n=66). The latter had recovered from mild, moderate, or severe SARS-CoV-2 infection. The positive result was confirmed using the RT-PCR test. Age and gender-matched uninfected individuals (n=70) acted as controls. Serial samples were available in 23 recovered patients.
Elevated plasma ACE2 activity persisted in SARS-CoV-2 patients 114 days post-infection
The findings of the study show that plasma ACE2 activity at 35 days post-infection was 97-fold higher in recovered COVID-19 patients when compared to uninfected controls (p<0.0001). Also, plasma ACE2 activity significantly varied with disease severity (p=0.033). Severe COVID-19 was associated with higher ACE2 activity as compared to mild disease (p=0.027).
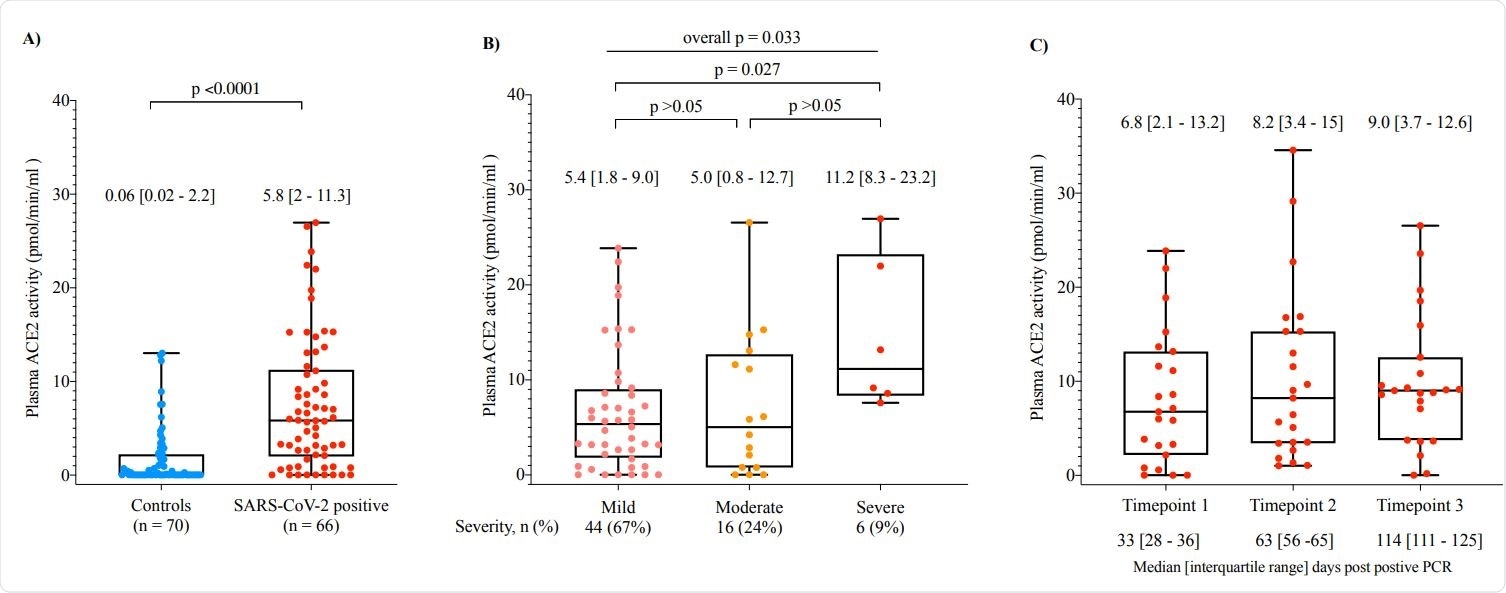
Plasma ACE2 activity is elevated in patients who recovered from SARS-CoV-2 infection (A), is increased with disease severity (B), and remains elevated 2-3 months after SARS-CoV-2 infection.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Interestingly, SARS-CoV-2-positive men (n=39) had higher median plasma ACE2 levels when compared to SARS-CoV-2-positive women (n=27) (p<0.0001). The team also analyzed if elevated plasma ACE2 activity persisted in SARS-CoV-2 positive subjects at 63 and 114 days post-infection. They found that plasma ACE2 activity stayed persistently elevated in most participants, with no significant differences between time points in post hoc comparisons (p>0.05).
Increased plasma ACE2 can be an independent risk factor for patients with cardiac disease
According to the researchers, this is the first study to find elevated plasma ACE2 activity after COVID-19 infection, and also the first with longitudinal data that indicates that plasma ACE2 activity stays elevated even at 114 days post-infection.
The team concluded that SARS-CoV-2 binding to ACE2 could have 2 effects. First, downregulation of membrane ACE2 which causes a dysregulated local renin-angiotensin system, which in turn triggers inflammation and tissue damage. Second, the dysregulated renin-angiotensin system is associated with prolonged release of the active site of ACE2 into the blood circulation.
Previous studies have shown that increased ACE2 was linked to increased risk of major cardiovascular events. Although the pathophysiological cause or consequence of elevated plasma ACE2 activity in severe COVID-19 is unknown, the study showed that increased plasma ACE2 activity could be an independent risk factor for patients with cardiac disease.
At a time when there is growing concern over severe COVID-19 in some patients and how to manage it, the authors emphasize the need for more extensive studies in the future to examine if elevated plasma ACE2 activity can identify at-risk individuals who are more prone to prolonged illness following SARS-CoV-2 infection.
“Larger studies are now needed to determine if persistent elevated plasma ACE2 activity identifies people at risk of prolonged illness following COVID-19 and to address whether therapeutic strategies directed at a dysregulated renin-angiotensin system can reduce COVID-19 complications.”

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Plasma ACE2 activity is persistently elevated following SARS-CoV-2 infection: implications for COVID-19 pathogenesis and consequences Sheila K Patel, Jennifer A Juno, P Mark Hogarth, Wen Shi Lee, Stephen J Kent, Louise M Burrell medRxiv 2020.10.06.20207514; doi: https://doi.org/10.1101/2020.10.06.20207514, https://www.medrxiv.org/content/10.1101/2020.10.06.20207514v2
- Peer reviewed and published scientific report.
Patel, Sheila K., Jennifer A. Juno, Wen Shi Lee, Kathleen M. Wragg, P. Mark Hogarth, Stephen J. Kent, and Louise M. Burrell. 2021. “Plasma ACE2 Activity Is Persistently Elevated Following SARS-CoV-2 Infection: Implications for COVID-19 Pathogenesis and Consequences.” European Respiratory Journal 57 (5): 2003730. https://doi.org/10.1183/13993003.03730-2020. https://erj.ersjournals.com/content/57/5/2003730.