The coronavirus disease 2019 (COVID-19) pandemic demands better and more rapid testing to ensure more accurate diagnosis, monitoring, and surveillance of disease and its spread. Serologic testing is used to identify severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection after the acute phase.
Antibody response in COVID-19
Seroprevalence studies, which measure a pathogen's presence in a population through blood tests, can be used to frame appropriate policies in managing the outbreak of COVID-19. However, this is dependent on the sensitivity and accuracy of the test itself. Currently, available tests are associated with a high percentage of false positives and false negatives.
Most serological studies carried out so far have described the onset of the antibody response to SARS-CoV-2, targeting the spike (S) and nucleocapsid (N) protein antigens, from the fourth day following the earliest symptom. At this time, specific IgM and IgG antibodies are detected, either at the same time or one after the other.
The antibody titers are generally observed to become steady around the sixth day from the first detection of antibodies. At present, most immunological tests center around recombinant S and N antigens. The S antigen is exposed on the viral surface, while the N protein is the most abundant viral protein during infection.
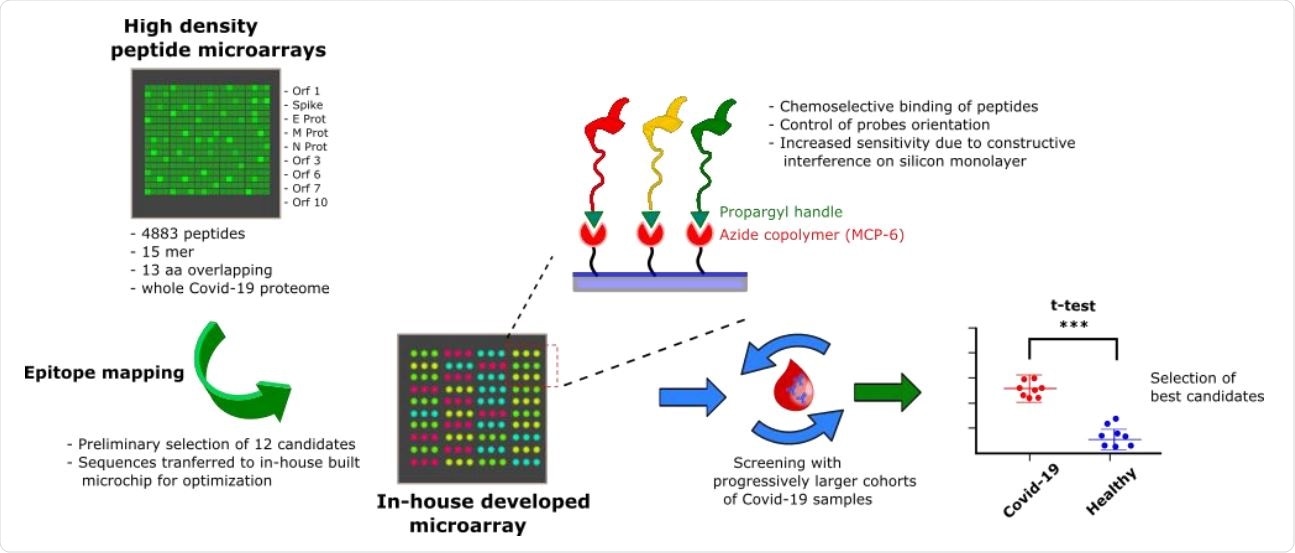
Overview of the probe selection workflow. A high-density peptide microarray displaying the whole SARS-CoV-2 proteome was probed for immunoreactivity with COVID-19 serum samples leading to the selection of 12 peptide hits. The most promising candidates were then transferred to a low-density microarray platform for site-selective and oriented peptide immobilization and validated with progressively larger and independent cohorts of patients to select the most sensitive and specific immunoreactive peptide probes.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Issues with full-length antigens
Recombinant full-length antigens have several disadvantages, however. They are expensive, difficult to store, and subject to deterioration over time and environmental fluctuations. The quality can thus vary significantly between batches. Moreover, the potential for cross-reaction is another issue that can confuse the final result of the test.
This is especially true of SARS-CoV-2 since some of the viral proteins are closely related to those expressed by phylogenetically close human coronaviruses, which are also commonly found in the human population at the same time, such as those causing the common cold.
The same regions of these viral proteins targeted by the virus-specific antibodies are also not fully described as of now, though fully understanding this could help explain different disease outcomes. It could also aid in the development of different immunology-based tests and therapies.
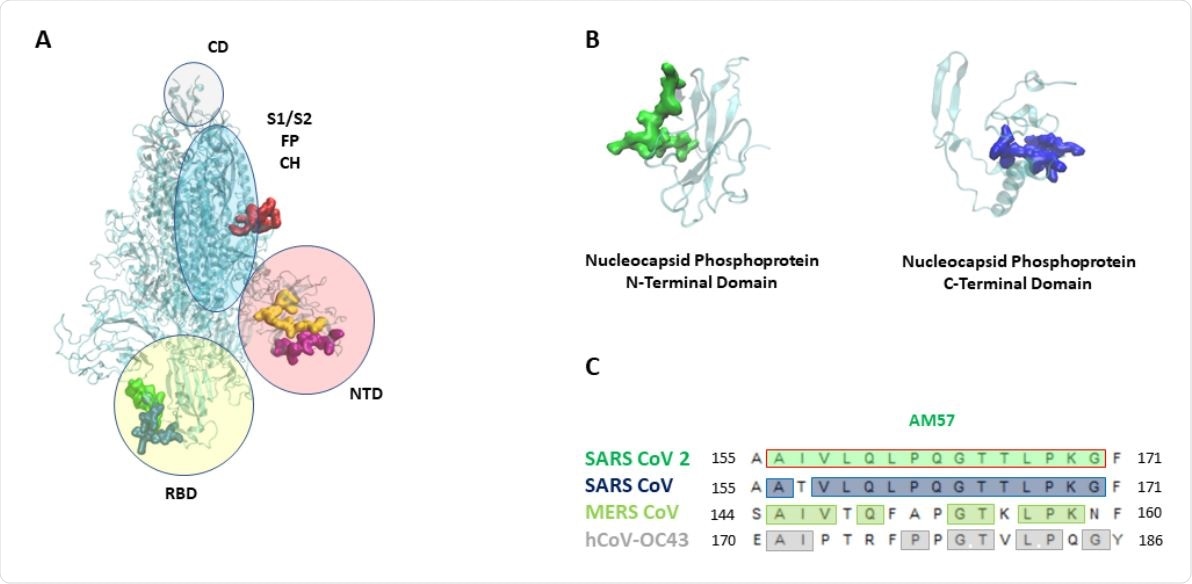
(A): SARS-CoV 2 Spike (S) protein with its domains 12 (NTD: n terminal domain, S1 e S2: furin cleavage site, CD: connecting domain, HR2: heptad repeat 2, FP: fusion peptide, CH: central helix). Epitopes are highlighted as follows: AM55 in red; AM50 in yellow; AM64 in purple; AM 63 in blue, AM 49 in green. (B) : SARS-CoV 2 nucleocapsid (N) protein, the N-terminal and C-terminal domains. Epitopes are highlighted as follows: AM57 in green, AM66 in blue. (C) : AM57 sequence alignment on SARS CoV 2, SARS CoV, MERS CoV, hCoV-OC43.
Advantages of synthetic peptides
The use of synthetic peptide probes is a promising solution to these problems since they are stable for storage, cheaply produced, and have high consistency from batch to batch. Moreover, problems with protein secondary and tertiary structure no longer arise. The ability to synthesize peptides to the exact sequence needed makes them highly versatile so that they can be used across a range of diagnostic settings, whether for point-of-care testing, lateral-flow testing, or for centralized laboratory workflows using ELISA and bead-mounted assays.
Selection and validation of epitopes
To help understand antigen-antibody interactions at the primary antigenic regions, the current researchers used peptide microarrays. This platform allows multiplex screening of up to thousands of peptides at the same time. The peptides are immobilized as spots on solid media, arranged in orderly patterns.
The researchers used over 4,800 peptides covering the entire viral proteome, sourced from serum samples from seven elderly PCR-confirmed and antibody-positive COVID-19 patients. All had a history of mild or moderate disease about a month before serum collection. Each peptide was 15 amino acids long, with 13 overlapping amino acids.
They found 12 possible linear epitopes on the N and S protein and the ORF1ab polyprotein. Using the microarray technology they had already developed, which uses peptides arranged in a site-selective and oriented manner, they validated the 12 epitopes with serum from another 12 patients, with the same time-frame, as well as serum collected before the first diagnosed COVID-19 case, in December 2018. Of the 12, six epitopes could discriminate between the cases and the controls.
Increasing the number of test samples to 28, collected from patients 1-5 months after symptom onset, reduced the hit epitopes to 3, one each from the N and the S protein and one from the ORF1ab polyprotein. Of these, the epitope in the N protein was highly immunoreactive and was specific in its binding to antibodies from infected individuals versus negligible binding in the control sera.
High discriminant power for N-Epitope AM57
The researchers concluded that the N protein presented the linear epitope (AM57) with the best specificity and sensitivity, in the region 155-171. In addition, this epitope shows only 53% homology with the N protein of seasonal coronaviruses.
They validated their conclusion using 50 samples from other COVID-19 patients, collected 1-5 months after the earliest symptom. This showed that anti-AM57 IgG antibodies showed high discriminant power, with 92% sensitivity and 100% specificity. This is very close to the performance offered by the full N antigen.
IgM antibodies against this epitope also had high discriminant power, but not against the full-length N antigen. The lack of any false-negatives with the IgG antibodies could be attributed to the lack of conservation of this epitope among other coronaviruses, thus preventing pre-existing cross-reactivity.
In addition, the AM57 epitope was assayed using 5 longitudinal sets of sera collected over months from the onset of disease. The researchers found that at two weeks from infection as defined by a positive PCR test, both IgM and IgG were detectable. The IgG but not the IgM antibody response persisted over the 7 weeks of testing.
Implications
The study concludes, "The ability of the AM57 peptide to early detect IgM response worth further investigation." Moreover, the authors say, "Synthetic peptides offer clear advantages in terms of costs and synthetic versatility allowing straightforward implementation in diverse diagnostic settings: from lateral-flow-tests for point of need diagnostics to ELISA and bead-based assays for centralized settings."
The ability of peptide microarrays to deal with a large number of peptides or specimens at the same time could potentially allow more specific synthetic probes to be formed for the diagnosis of COVID-19. Another promising offshoot could be the identification of new targets for immunotherapy of the infection.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Musico, A. et al. (2020). SARS-CoV-2 Epitope Mapping on Microarrays Highlights Strong Immune-Response to N Protein Region. bioRxiv preprint. doi: https://doi.org/10.1101/2020.11.09.374082, https://www.biorxiv.org/content/10.1101/2020.11.09.374082v1
- Peer reviewed and published scientific report.
Musicò, Angelo, Roberto Frigerio, Alessandro Mussida, Luisa Barzon, Alessandro Sinigaglia, Silvia Riccetti, Federico Gobbi, et al. 2021. “SARS-CoV-2 Epitope Mapping on Microarrays Highlights Strong Immune-Response to N Protein Region.” Vaccines 9 (1): 35. https://doi.org/10.3390/vaccines9010035. https://www.mdpi.com/2076-393X/9/1/35.