Aid for effective treatment strategies for coronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is also provided in many ways by predictions and modeling using machine learning. COVID-19 positive individuals present distinct severity patterns that are associated with different immune activation profiles. The Chronic COVID-19 (CC) – also known as the ‘Long Haulers’ (LH) – is a group of previously infected individuals. They require longer times to experience a full recovery, representing a particular pathological type.
In a new study by researchers at Universidad de Costa Rica and other institutions, a bioinformatics approach is used to determine whether Chronic COVID-19 (CC) might have a distinct immunologic signature compared to the mild to moderate (MM) or the severe/critical COVID-19. In this context, the team sought to identify possible immunologic signatures of COVID-19 severity. The researchers found that severe cases are characterized by excessive inflammation and dysregulated T cell activation, recruitment, and counteracting activities.
The team used a multi-class deep neural network classifier to better fit the prediction model; they recapitulated a 100% precision, 100% recall and F1 score of 1 on the test set. A first score specific for the chronic COVID-19 patients is defined in this study as S1 = (IFN-γ + IL-2 )/ CCL4-MIP-1β. Further, a score specific for the severe COVID-19 patients is defined as S2 = (10*IL-10 + IL-6) 63 – (IL-2 + IL-8).
After recovering from their acute illness and presumably months after viral clearance, they continue to experience a multitude of symptoms. From several weeks to months, they may suffer joint pain, muscle aches, fatigue, “brain fog” or other such symptoms, most likely resembling rheumatoid arthritis, autoimmune disorders, and others such as fibromyalgia and chronic fatigue syndrome. It is also supposed that these symptoms may be caused by the persistence of the COVID-19 itself.
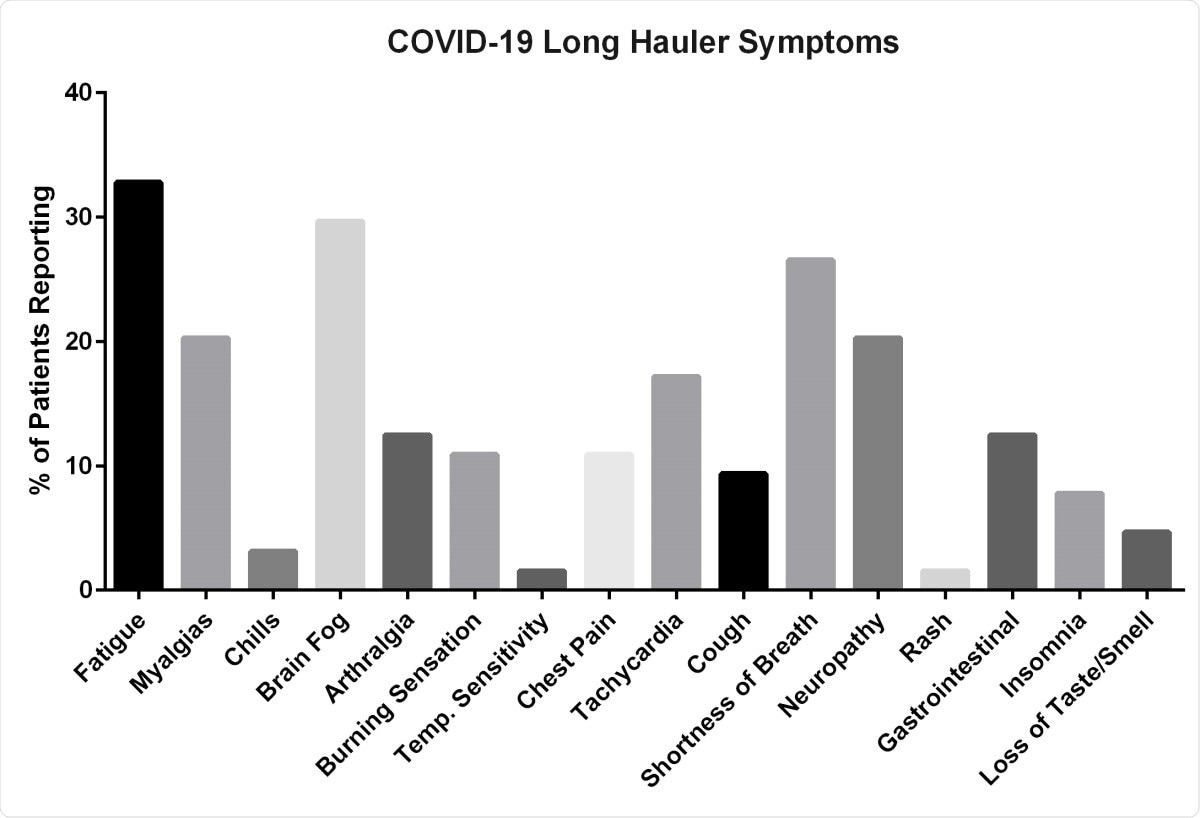
Symptoms reported by long hauler patients enrolled in the study.
In this study, the researchers investigated 144 individuals. There were 29 normal individuals. Patients spanning the COVID-19 disease continuum included 26 individuals with mild-moderate COVID-19, 25 individuals with severe COVID-19, and 64 individuals with Chronic COVID-19 symptoms. The researchers collected plasma and isolated PBMCs from all of them. They performed an immune subset profiling and a 14-plex cytokine panel on all patients. They analyzed the data using machine learning methods to predict and distinguish the groups from each other.
The severe cases are characterized by high IL-6 and IL-10 levels - these two cytokines are attributed to increasing the immunopathogenesis of COVID-19 and the predictive value in severe cases. To strengthen the classification, the score presented here differentiates the severe cases by the subtraction of IL-2 and IL-8, which are cytokines related to proper T cell activation (IL-2) and recruitment (IL-8).
The score generated for distinguishing the LH, these patients are characterized by increased IFN-γ and IL-2 and reduced CCL4 production. Interestingly, there was an increase in the percentage of circulating CD4+ and CD8+ T cells expressing CTLA-4 in the LH group compared to healthy donors. This is a molecule that affects antigen presentation in secondary lymphoid organs, but its presence in circulating T cells may also reflect compensatory mechanisms to the low CCL4 levels in the LH group.
The researchers propose that the long-lasting pulmonary damage observed in LH is caused by a combination of factors including 1) longer virus persistence influenced by LH immune profile characterized by high IFN-γ and IL-2 levels inducing Th1 polarization, which is ineffective with low CCL4-induced T cell recruitment, leading to an inflammatory myeloid cell activation; and 2) the immunopathological pulmonary effects consequence of this LH immune profile.
Interestingly, COVID-19 individuals (including LH, mild, severe) show high levels of CCL5, a chemoattractant that like CCL4 signals through CCR5.
Using machine learning, they identified algorithms that allowed for accurate determination of chronic COVID and severe COVID immunotypes. The researchers also addressed the question of whether the immunologic profile represents an immune response indicative of prolonged or chronic antigenic exposure. Importantly, they present a quantitative immunologic score that could be used to stratify patients to therapy and/or non-subjectively measure response to therapy.
Recent scientific evidence from the last few months strongly supports that the outcomes for COVID-19 patients are determined by the immune mechanisms activated in response to the viral infection, and they are different in each case. This study throws light on determining important predictive biomarkers that help in better stratification of patients - avoids saturation of health systems and reduces the burden on the caretakers.
Journal reference:
Bruce Patterson, Jose Guevara-Coto, Ram Yogendra, Edgar B. Francisco, Emily Long, Amruta Pise, Hallison Rodrigues, Purvi Parikh, Javier Mora, Rodrigo A. Mora-Rodriguez. Immune-Based Prediction of COVID-19 Severity and Chronicity Decoded Using Machine Learning. bioRxiv preprint server. 2020.12.16.423122; doi: https://doi.org/10.1101/2020.12.16.423122, https://www.biorxiv.org/content/10.1101/2020.12.16.423122v1