Several reports of breakthrough infections with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) have been published in different countries among fully vaccinated individuals. Most of these reports are from long-term care facilities (LTCF), which are considered a sentinel event for re-infection after full vaccination due to a sub-optimal antibody response because of the age of residents, underlying comorbidities, and ongoing corticosteroids therapy.
The recent spread of the SARS-CoV-2 B.1.617.2 Variant of Concern (VOC), which is more commonly known as the Delta variant, is of particular concern in this regard. Researchers have recently published a report on the preprint server medRxiv* wherein they analyzed an outbreak of breakthrough infections in a small nursing home in Northerneastern Italy. The aim of this study was to provide information on how the reduction in anti-spike immunoglobulin G (IgG) titers was proportional to the waning of messenger ribonucleic acid (mRNA) vaccine protects against the Delta variant.
About the study
Towards the end of August 2021, one healthcare worker (HCW) of the LTCF in the current study tested positive for the coronavirus disease 2019 (COVID-19) following routine checks performed via a microfluidic immunofluorescence assay for the qualitative detection of nucleocapsid antigens (LumiraDX SARS-CoV-2 Ag). Following this, all LTCF residents and staff were screened with the same assay, following which 12 additional residents and 5 HCWs tested positive for COVID-19.
Within the next two days, confirmatory molecular reverse-transcriptase polymerase chain reaction (RT-PCR) tests on nasopharyngeal swabs were carried out among all residents and HCW staff. Ten of these swabs were sent to the Istituto Zooprofilattico Sperimentale delle Venezie for the Sars-CoV-2 B.1.617.2 lineage characterization. At the same time, blood samples were drawn from residents and a sample of HCWs for determining serum levels of both anti-spike IgM and IgG antibodies.
The outbreak lasted 42 days, accounting for 10 days after the last SARS-CoV-2 infection. For the convenience of analysis, all affected residents were grouped as A) Asymptomatic patients a fever of greater than 38 °C or headache; B) Symptomatic patients with a fever of greater than 38 °C, cough, diarrhea, anorexia, lethargy, psychomotor retardation, and/or mental confusion; as well as C) Severely infected patients with dyspnoea and desaturation < p92 leading to fatal outcomes. Immunization records on the participants’ previous doses of the mRNA COVID-19 vaccine were also provided.
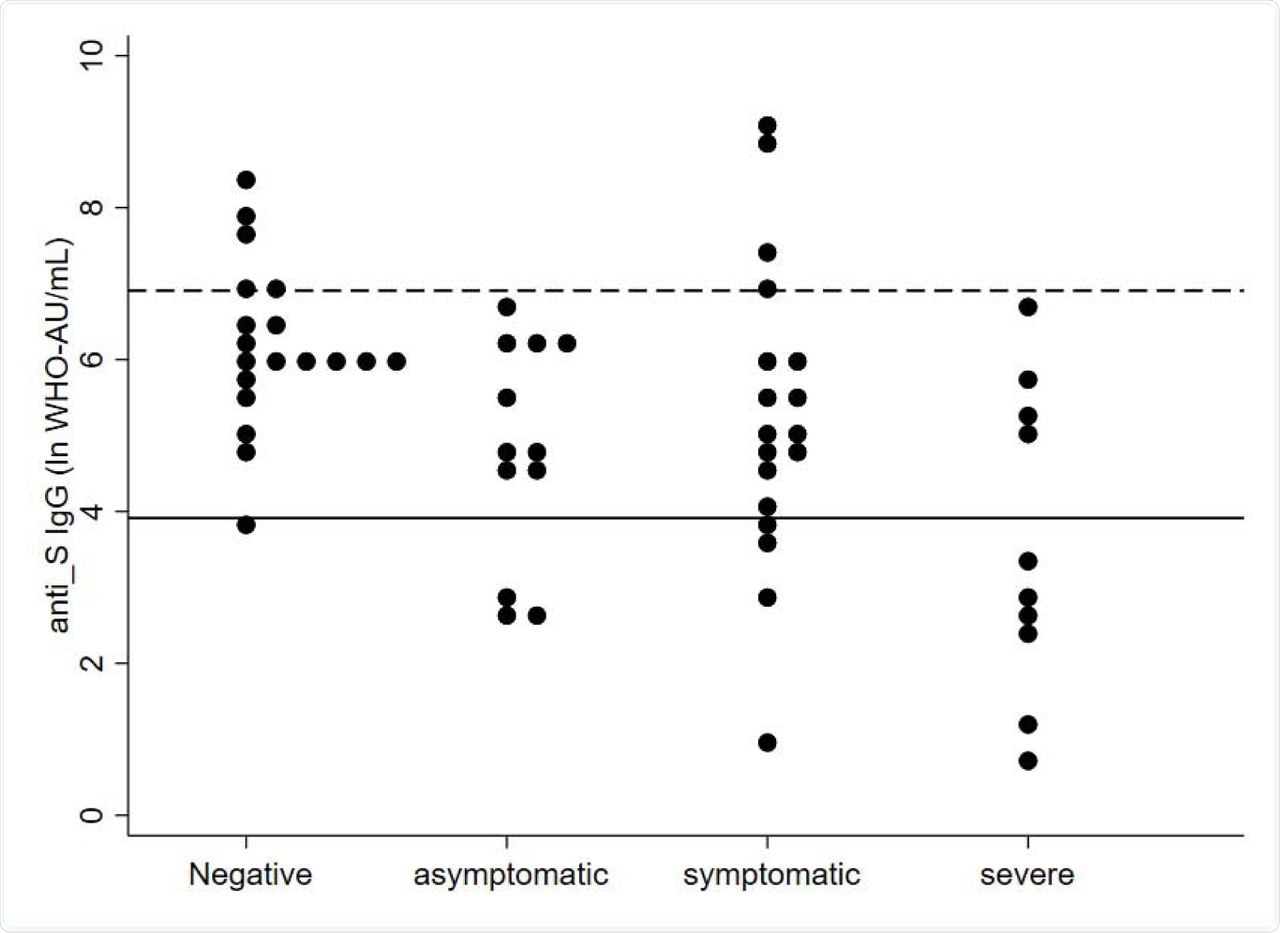 Cumulative Incidence of SARS-CoV-2 infection and Covid-19 disease among 59 residents fully vaccinated with mRNA vaccine 28 weeks before, and with no previous SARS-CoV-2 PCR-confirmed infection, by anti-S IgG level (BAU/mL) measured at the beginning of the outbreak. Full and dotted black lines represent two conventional threshold levels of 50 and 1000 BAU/mL.
Cumulative Incidence of SARS-CoV-2 infection and Covid-19 disease among 59 residents fully vaccinated with mRNA vaccine 28 weeks before, and with no previous SARS-CoV-2 PCR-confirmed infection, by anti-S IgG level (BAU/mL) measured at the beginning of the outbreak. Full and dotted black lines represent two conventional threshold levels of 50 and 1000 BAU/mL.
On the date of the first recorded infection, there were three individuals among the 69 residents and five individuals among the 69 HCWs present who had a previous SARS-CoV-2 RT-PCR-confirmed infection between March 2020 and April 2021. Taken together, 83% HCWs and 91% of residents were vaccinated against COVID-19, 98% of which had received the BNT162B2 mRNA vaccine, with the second dose received at an average of 196 days before the outbreak.
Among the residents, two individuals received only the priming dose, and four remained were unvaccinated. Comparatively, among HCWs, six were primed and six were unvaccinated.
Within 30 days, 46 and 14 new cases were found among residents and HCWs, respectively, with 75% of cases confirmed within the first week from the detection of the first case. Spike sequencing on seven residents and three HCW swab samples showed positive results for the Delta VOC.
Among the residents, 13 individuals were asymptomatic, 21 were symptomatic, and 12 had severe COVID-19 cases. Taken together, eight of the residents who were infected with SARS-CoV-2 during this outbreak had died. Two deaths occurred 11 days from the last negative PCR test and thus were not accounted as fatal COVID-19 cases.
Anti-spike IgG geometric mean was 161 and 625 BAU/mL among tested residents and HCWs, respectively. Residents who were younger than 80 years old showed a geometric mean of 585 BAU/mL, which is comparable to that of residents who were older than 80 who had a geometric mean of 103 BAU/mL,.
Among those tested, fully vaccinated, and without previous SARS-CoV-2 infection, none of the HCWs and 24% of residents had anti-Spike IgG of greater than 50 BAU/mL. For these residents, the elapsed time since the boost at the onset of the outbreak was about 199 days. For them, the anti-Spike IgG titers were less than 50 BAU/mL and resulted in a higher risk of SARS-CoV-2 and severe COVID-19 disease.
An estimated 25% of fully vaccinated LTCF residents with no previous SARS-COV-2 infection had anti-Spike IgG of less than 50 BAU/mL about 28 weeks after the boost. This translates into a vaccine efficacy (VE) of 35% against infection and 79% against severe COVID-19 disease, thus suggesting that the protection conferred from anti-spike IgG titers of less than 50 BAU/mL is very low.
Implications
This crucial study reported a Delta variant outbreak in an Italian LTCF. Measuring the IgM and IgG antibody titers among residents and HCWs alike proved valuable in analyzing the effects of the vaccine and determining the course of action for the elderly and immunocompromised.
Further research on a larger cohort would ensure a proper definition for the anti-spike IgG threshold levels to identify and better protect those who are at a higher risk of severe COVID-19, particularly following infection with the SARS-CoV-2 Delta variant.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Pierobon, A., Dal Zotto, A., Antico, A., et al. (2021). Outbreak of SARS-CoV-2 B.1.617.2 (Delta) variant in a Nursing Home 28 weeks after two doses of mRNA anti-Covid-19 vaccines: evidence of a waning immunity. medRxiv. doi:10.1101/2021.10.25.21265370 .
- Peer reviewed and published scientific report.
Pierobon, Alice, Alessandra Dal Zotto, Antonio Antico, Mario Ernesto De Antoni, Liviano Vianello, Monica Gennari, Antonio Di Caprio, Francesca Russo, Gianfranco Brambilla, and Mario Saugo. 2021. “Outbreak of SARS-CoV-2 B.1.617.2 (Delta) Variant in a Nursing Home 28 Weeks after Two Doses of MRNA Anti-COVID-19 Vaccines: Evidence of a Waning Immunity.” Clinical Microbiology and Infection, December. https://doi.org/10.1016/j.cmi.2021.12.013. https://www.clinicalmicrobiologyandinfection.com/article/S1198-743X(21)00721-7/fulltext.