The coronavirus disease 2019 (COVID-19) outbreak caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has resulted in a sharp rise in deaths and the number of infections worldwide. The pandemic has resulted in the deaths of more than 5.1 million people from more than 254 million infections as of November 18, 2021. Therefore, the development of safe and effective vaccines was considered an important measure to contain the pandemic and restore people’s lives to normal.
As per the global statistics reports from August 2, 2021, there are 326 total vaccine candidates. Out of them, 103 vaccines are in clinical trials, while 19 are now in everyday use. The 19 vaccines include 8 inactivated vaccines, 5 protein subunit vaccines, 2 mRNA vaccines, and 4 non-replicating viral vector vaccines. Furthermore, reports show that 53.7 percent of the world population has received at least one dose of the vaccine, while 41.5 percent are fully vaccinated.
However, the infection rate of COVID-19 is still high due to the emergence of new SARS-CoV-2 variants. Therefore, rapid herd immunity through vaccination is required to prevent the emergence of these new variants that can completely escape the immune surveillance.
The effectiveness and safety of the three mainstream vaccines in the market have been evaluated based on random clinical trials (RCT). The mRNA vaccines were found to be the most effective, followed by viral vector vaccines and inactivated virus vaccines. Although the current safety of the COVID-19 vaccines is high, long-term monitoring needs to be carried out, especially for people with underlying conditions. However, real-world studies vary significantly from the RCT. Mass vaccination in the real world requires considering several heterogeneous populations, vaccine supply, willingness, medical accessibility, etc. Several studies report the effectiveness of vaccines in the real world but the results remain controversial.
A new study published in Infectious Diseases of Poverty aimed to systematically evaluate the effectiveness and safety of the COVID-19 vaccines in the real world as well as establish a reliable evidence-based basis to determine the actual protective effect of the COVID-19 vaccines, especially considering the new waves of infection brought about by the variants.
The study
The study involved searching three databases, PubMed, Embase, and Web of Science, for eligible studies that have been published by July 22, 2021. It included 58 studies, out of which 32 were for vaccine effectiveness and 26 were for a safety study. The study was strictly performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA).
Observational studies were included that examined the effectiveness and safety of the COVID-19 vaccines among vaccinated people. Studies with irrelevant subjects, insufficient data, overlapping participants, reviews, editorials, case reports, conference papers, animal experiments, and those that did not clarify the identification of COVID-19 were excluded.
The studies were identified by two investigators who carried out data extraction and also assessed the study quality. A third investigator resolved any disagreements. Finally, meta-analysis was performed with the extracted data to assess the safety and effectiveness of the COVID-19 vaccines.
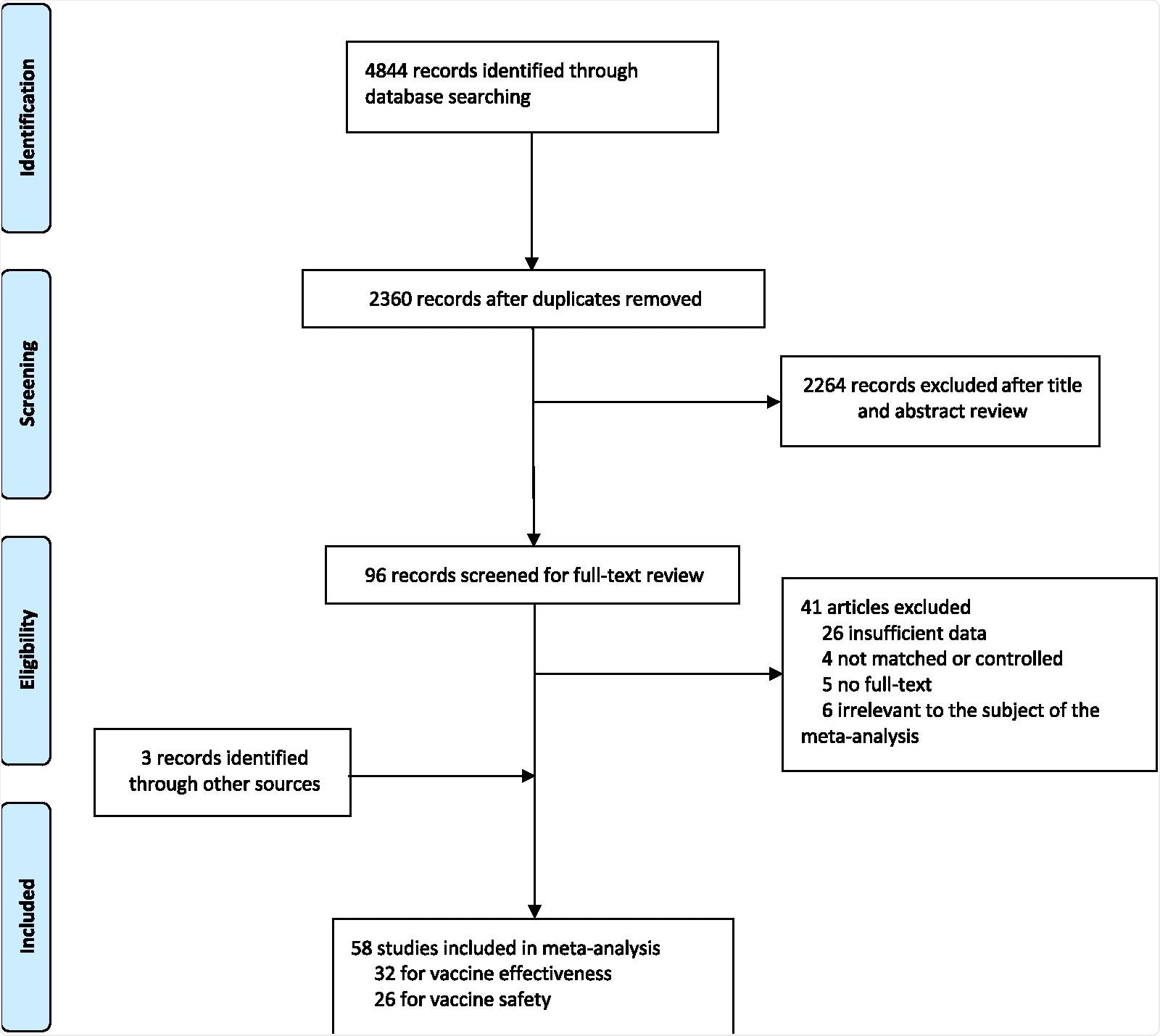
Flowchart of the study selection
Findings
The results of the study reported vaccine effectiveness (VE) separately for the first and second doses. For the first dose, the VE for prevention of infection was 41 percent, for prevention of symptomatic COVID-19 infection was 52 percent, for prevention of hospitalization was 66 percent, for prevention of ICU admission was 45 percent, and for the prevention of COVID-19 related deaths was 53 percent.
While for the second dose, the VE for the prevention of SARS-CoV-2 infection was 85 percent, for prevention of symptomatic COVID-19 was 97 percent, for prevention of hospitalization was 93 percent, for the prevention of ICU admissions was 96 percent, and for the prevention of COVID-19-related death was 95 percent.
Furthermore, the study reported the VE for the various SARS-CoV-2 variants. The VE was 85 percent for prevention against the Alpha variant, 54 percent for the Gamma variant, and 74 percent for the Delta variant. Only one study was available for the Beta variant, where the VE was reported to be 75 percent. The BNT162b2 vaccine was found to have the highest VE for each of the variants.
The study also reported overall pooled incidence rate was 1.5% for adverse events, 0.4 per 10,000 for severe adverse events, and 0.1 per 10 000 for death after vaccination.
Healthcare workers showed a higher incidence rate for adverse events, serious adverse events, as well death after vaccination. Also, the incidence rate of adverse events was found to be higher in the AZD1222 vaccine group, serious adverse events were found to be higher in the Gam-COVID-Vac vaccine group, and death after vaccination was found to be higher in the BNT162b2 vaccine group.
The current study thus indicated that two doses of the vaccine were effective against the different SARS-CoV-2 variants, although their effectiveness was less as compared to the original strain. The adverse events were found to be varied among different COVID-19 vaccine groups. However, serious adverse events were reported that suggest the need to implement a unified global surveillance system to monitor the adverse events of the COVID-19 vaccines around the world. Also, while determining the priority of the vaccines, the socioeconomic characteristics of each country must be considered.
Therefore, it can be concluded that the improvement of vaccine coverage is still the most essential tool that can help to end the pandemic.
Limitations
The current study had certain limitations. First, the study included limited basic data on specific populations. Second, no subgroup analysis on more population characteristics, such as age was conducted. Third, most of the original studies collected adverse events only up to 7 days post-vaccination. This could have an impact on the safety analysis.