As a result of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), there has been significant morbidity and mortality among nursing home residents during the coronavirus disease 19 (COVID-19) pandemic.
Initially, the prioritized vaccination drive in the NH residents was able to provide a satisfactory level of protection from COVID-19 associated morbidity and mortality. Still, later over time, as the vaccine-induced antibody levels waned, the nursing home residents once again became prone to breakthrough SARS-CoV-2 incidences.
Researchers from the United States, in their recent study published on the preprint server medRxiv*, have evaluated the humoral responses to third vaccine dose in nursing home residents and healthcare workers (HCW) and found that that second booster (or third vaccine dose) significantly increased anti-spike, anti-receptor binding domain (RBD), and neutralization titers in almost all nursing home residents and HCW to considerably higher levels than what was attained after the completion of the initial two-dose vaccine series.
 Study: Significantly elevated antibody levels and neutralization titers in nursing home residents after SARS-CoV-2 BNT162b2 mRNA booster vaccination. Image Credit: Skylines / Shutterstock
Study: Significantly elevated antibody levels and neutralization titers in nursing home residents after SARS-CoV-2 BNT162b2 mRNA booster vaccination. Image Credit: Skylines / Shutterstock

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Antibody levels, developed from standard two-dose immunization series, dropped by >80% in nursing home residents and HCW
According to a previous study conducted by the same team, antibody levels and neutralization titers in nursing home residents, with completed two-dose series of BNT162b2 (Pfizer-BioNTech) mRNA vaccination, dropped by more than 80% in six months following vaccination. Fifty-seven percent did not even have detectable neutralizing antibodies. HCWs also demonstrated over 80% decline, even if they had a history of prior SARS-CoV-2 infection.
This marked decay of humoral protection left the residents at risk of breakthrough SARS-CoV-2 infection and prompted the authorization of booster doses in nursing home residents.
Reports on the post-booster vaccination titers in the more frail and disabled nursing home population are not available. Therefore, the team co-lead by Dr. David H Canaday and Dr. Stefan Gravenstein undertook this study to examine the effect of boosting humoral immunity among nursing home residents and HCWs, who live in their close vicinity.
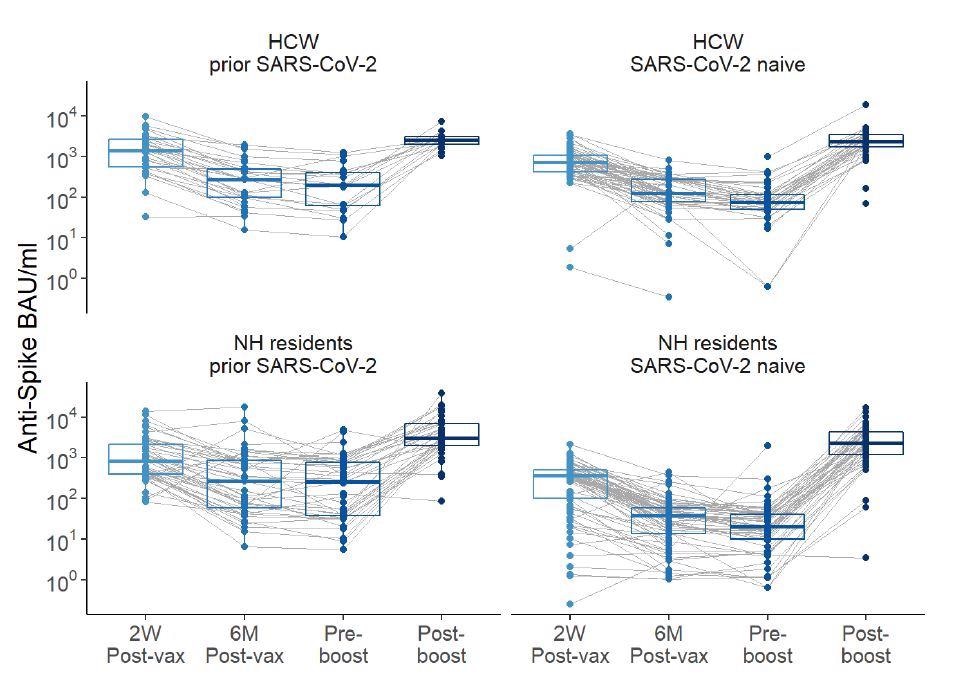 Anti-spike levels over time pre- and post-boost with BNT162b2 mRNA vaccination in healthcare workers (HCWs) and nursing home (NH) residents, with and without history of SARS-CoV-2. Anti-spike values depicted in the binding arbitrary units /milliliter (BAU/ml) based on the WHO standard. 2 weeks (2W Post-vax) and 6 months (6M Post-vax) post primary vaccination series and Pre-boost (generally 6-8 months after the first two-dose vaccination series) and Post-boost which is 14±3 days after vaccine boost.
Anti-spike levels over time pre- and post-boost with BNT162b2 mRNA vaccination in healthcare workers (HCWs) and nursing home (NH) residents, with and without history of SARS-CoV-2. Anti-spike values depicted in the binding arbitrary units /milliliter (BAU/ml) based on the WHO standard. 2 weeks (2W Post-vax) and 6 months (6M Post-vax) post primary vaccination series and Pre-boost (generally 6-8 months after the first two-dose vaccination series) and Post-boost which is 14±3 days after vaccine boost.
What did the researchers do?
Serum samples were obtained within 14 days before and 14 ± 3 days after BNT162b2 mRNA second booster dose from 85 nursing home residents (median age 77) and 44 HCWs (median age 50) from three nursing homes for whom the serum samples after initial SARS-CoV-2 BNT162b2 mRNA vaccination series were available.
IgG antibodies to spike protein and its RBD were quantified. Neutralizing antibody titers were determined using lentiviral particles pseudotyped with spike protein based on the Wuhan strain.
Geometric mean fold rise (GMFR) was assessed from pre- to post-booster, and from two weeks post-initial vaccination to post-booster on the log-transformed titer fold change values.
Study findings
Prior SARS-CoV-2 infected nursing home residents and infection-naive nursing home residents and HCWs all achieved higher anti-spike antibody, anti-RBD antibody, and neutralization titers after the second booster than observed two weeks after their initial vaccine series, demonstrating that second booster produced their highest antibody titers to date.
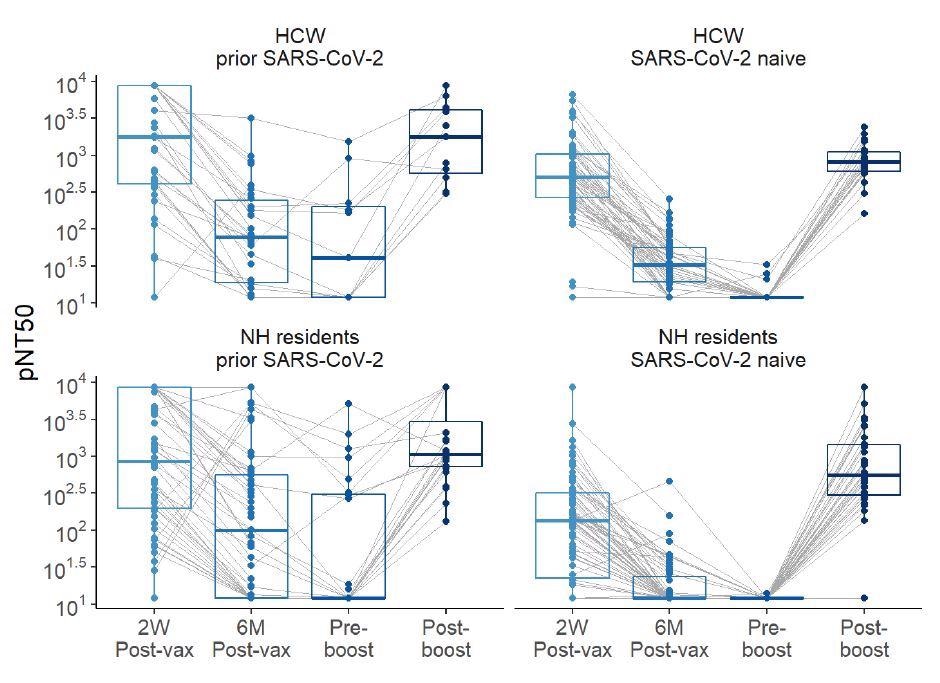 Neutralization titers over time pre- and post-boost with BNT162b2 mRNA vaccination in HCW and NH residents, with and without history of SARS-CoV-2. Pseudovirus neutralization (pNT50) values are shown. The upper limit of detection of the assay is 1:8748 and the low limit of detection of the neutralization assay is 1:12.
Neutralization titers over time pre- and post-boost with BNT162b2 mRNA vaccination in HCW and NH residents, with and without history of SARS-CoV-2. Pseudovirus neutralization (pNT50) values are shown. The upper limit of detection of the assay is 1:8748 and the low limit of detection of the neutralization assay is 1:12.
“We take encouragement from the finding that most of even this debilitated and multi-morbid NH group can immunologically eventually mount a substantial antibody response to these vaccines”, the team highlights.
Infection-naive nursing home residents who previously demonstrated the lowest initial vaccine response and lowest antibody titers six months later, after boosting, had a robust GMFR of 9.3 in anti-spike antibody levels and a GMFR of 6 in neutralization titer from their prior peak titers two weeks after the initial vaccine series.
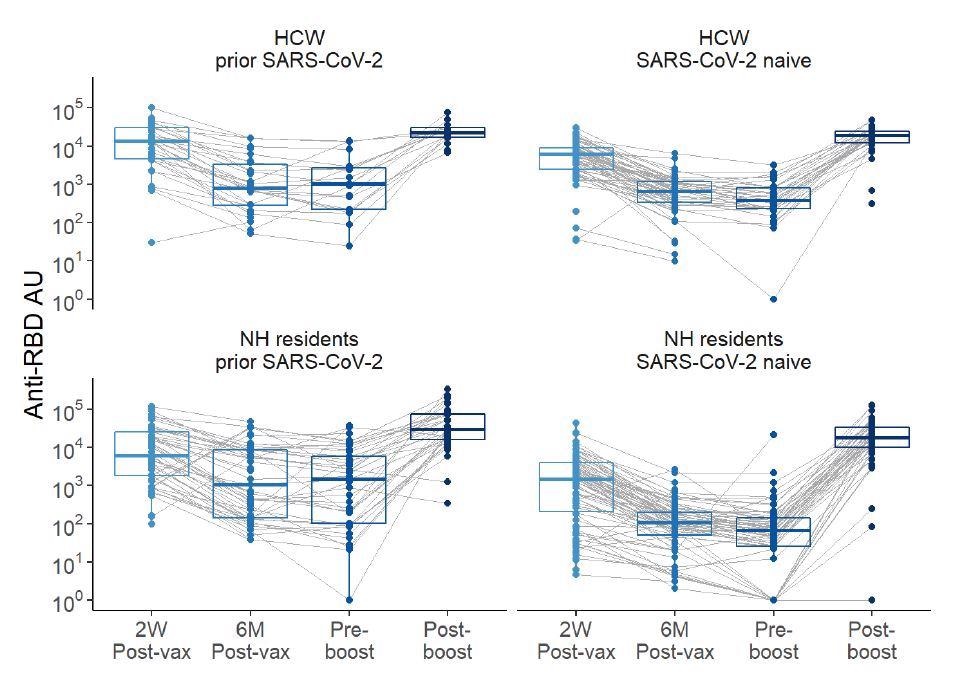 Anti-Receptor binding domain (RBD) levels over time pre- and post-boost with BNT162b2 mRNA vaccination in HCW and NH residents, with and without history of SARS-CoV-2.
Anti-Receptor binding domain (RBD) levels over time pre- and post-boost with BNT162b2 mRNA vaccination in HCW and NH residents, with and without history of SARS-CoV-2.
A previous report that supports the prospect of anti-spike antibody titer being an important correlate of protection suggested that anti-spike antibody titers of 264 BAU/ml can confer 80% protection from symptomatic infection.
Notably, the current study found that 95% of the nursing home residents attained these antibody levels after the second booster, compared to only 81% two weeks after the initial two-dose series.
Moreover, the geometric mean titers (GMT) of anti-spike antibodies increased to 1977 BAU/ml after the second booster compared to only 212 BAU/ml post-primary vaccine series in the infection naïve nursing home residents. Similarly, neutralization titers had a GMT increase, achieving much higher levels after boosting (578 vs. 96 NT50).
The second booster dose also improved the antibody levels in the hyporesponsive group, with low antibody levels attained after the initial two-dose vaccine series, much closer to the median level of the responding population.
Based on the findings, the team thus supports the use of a second booster, if possible, at a much earlier time in nursing home residents to prevent this immunologically weaker group from the occurrence of breakthrough infections.
“Given the decline in antibody levels in the 6 months following initial vaccination, and the substantial increase in anti-spike, RBD and neutralization levels after the booster, our data strongly support current CDC recommendations for boosting nursing home residents and HCWs for the likelihood that it translates to increased clinical protection”, concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Canaday DH, et al. (2021) Significantly elevated antibody levels and neutralization titers in nursing home residents after SARS-CoV-2 BNT162b2 mRNA booster vaccination. medRxiv. doi: https://doi.org/10.1101/2021.12.07.21267179, https://www.medrxiv.org/content/10.1101/2021.12.07.21267179v1
- Peer reviewed and published scientific report.
Canaday, David H., Oladayo A. Oyebanji, Elizabeth White, Debbie Keresztesy, Michael Payne, Dennis Wilk, Lenore Carias, et al. 2022. “COVID-19 Vaccine Booster Dose Needed to Achieve Omicron-Specific Neutralisation in Nursing Home Residents.” EBioMedicine 80 (June). https://doi.org/10.1016/j.ebiom.2022.104066. https://www.thelancet.com/journals/ebiom/article/PIIS2352-3964(22)00247-X/fulltext.