
 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Introduction
In Italy, several vaccines received authorization in the struggle to contain the deadly coronavirus disease 2019 (COVID-19) pandemic, including the two messenger ribonucleic acid (mRNA) vaccines BNT162b2 (Pfizer-BioNTech) and CX-024414 (Moderna), as well as two adenovirus vector vaccines including ChAdOx1 nCoV-19 (Oxford-AstraZeneca) and Ad26.COV2-S (Johnson & Johnson). Since their approval, over 56% of the Italian population has been covered by vaccination.
The current study studies vaccination coverage among people who had nasopharyngeal swabs showed symptoms of COVID-19 or were hospitalized. The researchers then compared the incidence of each between vaccinated and non-vaccinated individuals and analyzed the trends of each over time.
All swabs were tested using reverse transcriptase-polymerase chain reaction (RT PCR) testing for four genes including RNA-dependent RNA polymerase (RdRp), spike (S) gene, nucleocapsid (N) gene, and the envelope (E) gene. The cycle threshold for a positive test was set as over 30. All four genes had to be positive for a fully positive test.
Symptoms like shortness of breath, sore throat, a runny nose, headache, severe fatigue, diarrhea, nausea or vomiting, or itchy red lesions on the fingers and/or toes, were considered suggestive of COVID-19 if present two weeks before or after a positive PCR test.
The researchers used artificial intelligence (AI) to analyze the data after identifying those with and without effective vaccination, as well as for those who were unvaccinated.
Study findings
The study took place from March 8, 2021, to October 31, 2021, in the Campania region of Italy. Over 2.5 million swabs were obtained from adults during this period.
Of the total number of COVID-19-positive adults, 82% were non-vaccinated and 15% vaccinated. Overall, the prevalence of COVID-19 among the fully vaccinated people in Campania with 15 or more days between the second dose and the positive test was 0.33%.
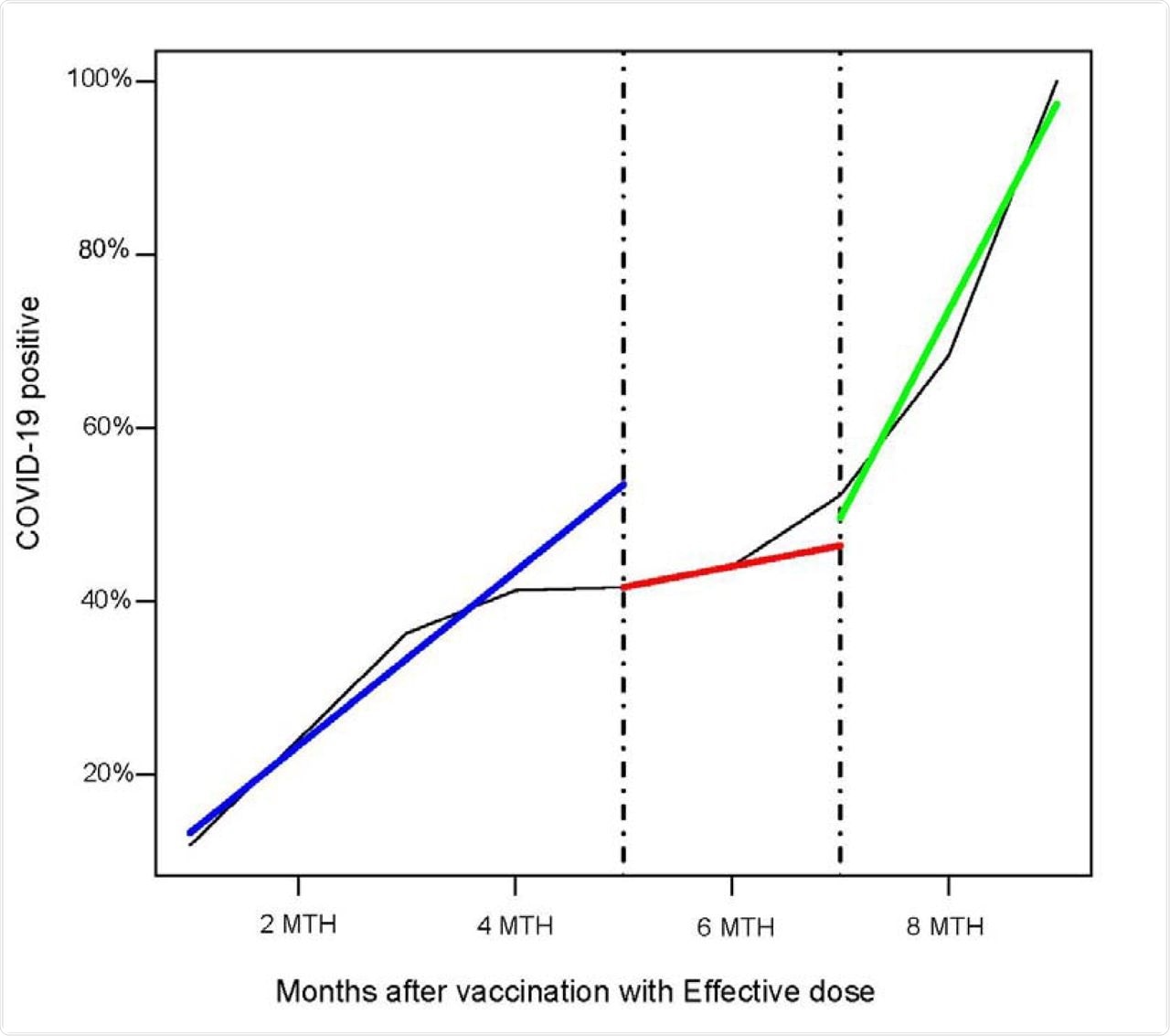
Segmented linear regression models
Among the vaccinated in this study, 7.5% tested positive within 15 days of the second dose or had received only a single vaccine dose. Almost the same number had received the second dose of the vaccine 15 or more days before testing positive.
About half the positive tests were in those aged up to 40 years, with about 30% and 16% being in the 40-60-year age group and 6-80 year age group, respectively. About 3% were in those older than 80 years.
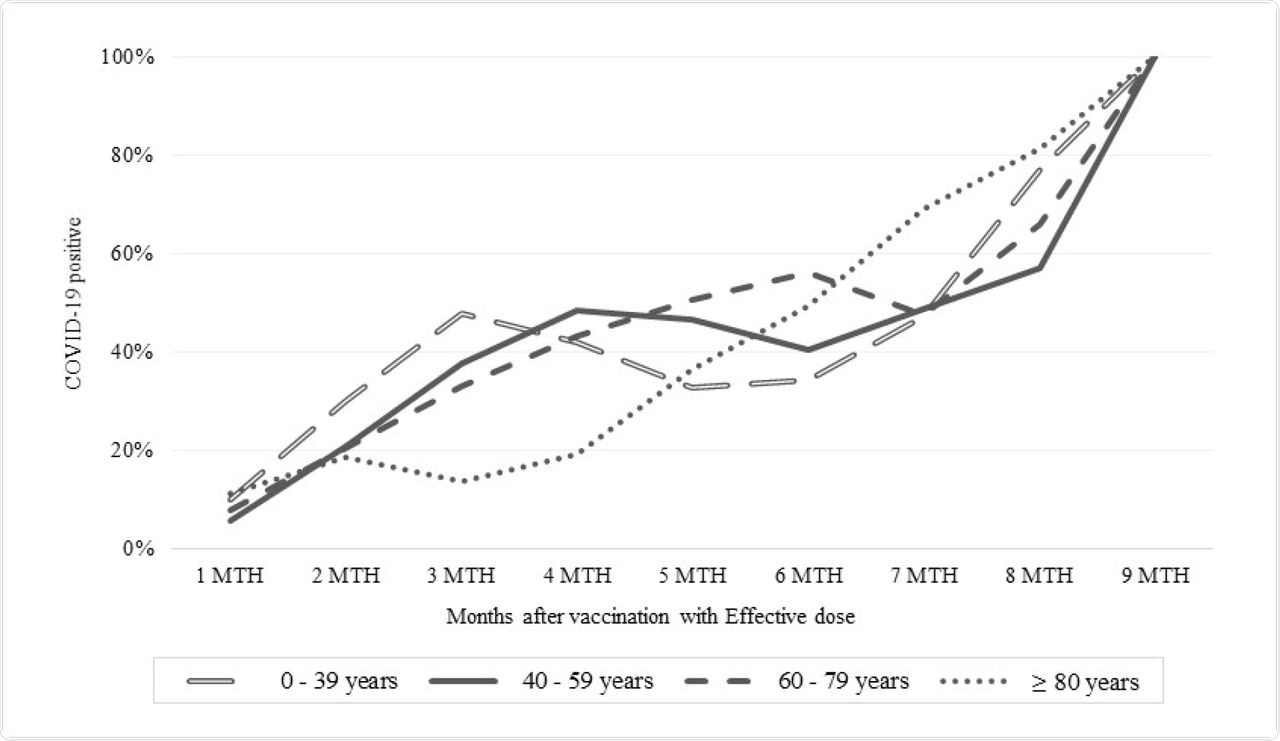
Percentage of COVID-19 positive patients stratified by number of months after vaccination with effective dose and stratified by age groups
Less than 3% were hospitalized and 0.1% were admitted to the intensive care unit (ICU), with almost 84% of the hospitalized individuals being non-vaccinated as compared to 6% who had received the second dose 15 or more days before they became sick. Over 90% of ICU patients were unvaccinated, with less than 2% effectively vaccinated.
Severe COVID-19 occurred in 482 individuals, of which almost 90% were unvaccinated. Of the remaining individuals who experienced severe COVID-19, 7.5% had received only one vaccine dose or were within 15 days of the second dose. Only 3% of these individuals had been effectively vaccinated.
Critical disease was recorded in 57 subjects, of whom 83% were unvaccinated, 11% ineffectively vaccinated, and 7% effectively vaccinated.
Males were at a 70% greater risk for hospitalization or ICU admission, while elderly people over 60 years had 29-34 times higher odds of having to be hospitalized or admitted to the ICU.
Ineffective vaccination, that is, having received only a single dose or two doses less than 15 days prior, was associated with a four-fold higher risk as compared to a seven-fold higher risk for the unvaccinated.
The waning of immunity was obvious at five and nine months from the second dose. Similarly, about half of the breakthrough infections occurred in individuals younger than 80 years, with over 40% occurring in individuals over the age of 80 years at six months after vaccination.
When classified by type of vaccine, breakthrough infections with the J&J vaccine occurred within a month of the second dose. Conversely, about half of the reported breakthrough infections occurred 4-6 months after receiving a second dose of the AstraZeneca (AZ) adenovirus vector vaccine.
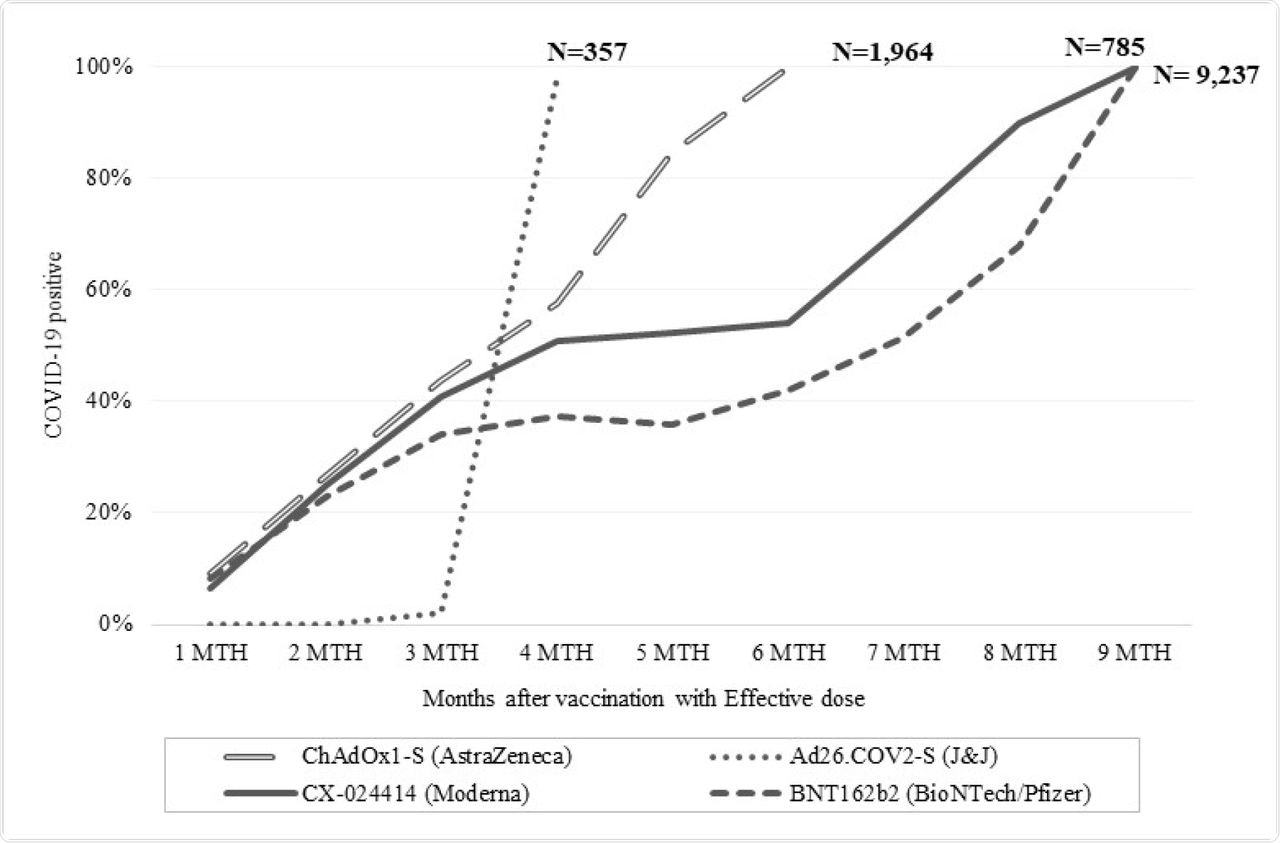
Percentage of COVID-19 positive patients stratified by number of months after vaccination with effective dose and stratified by age groups and stratified by vaccine type
With the Moderna vaccine, half of the patients tested positive for COVID-19 from four months onward, and 90% tested positive by nine months from the second dose. Finally, over a third of breakthrough infections with the Pfizer vaccine occurred at 4-5 months, with over two-thirds occurring by eight months.
Implications
A surveillance approach based on the use of integrated BIG Data system offer a precise and real analysis with low incidence of errors in the categorization of subjects.”
The results of this Campania study show a strong protective effect of two doses of an mRNA or adenovirus vaccine vector against SARS-CoV-2 infection, hospitalization, and ICU admission. Overall, 0.33% of the vaccinated population tested positive for COVID-19 as compared to 7% of people in this study, most of whom were asymptomatic.
The study findings suggest that test positivity increases with the time from the second dose, peaking at five months, with most tests being asymptomatic. While mRNA and the AZ viral vector vaccines show comparable initial effectiveness, the AZ vaccine appears to decline in its efficacy at a more rapid rate after four months. In contrast, the J&J vaccine effectiveness declines at one month.
Notwithstanding the waning of immunity, the results show that vaccination still reduces the severity of disease and the risk of severe hospitalization after infection. However, effective vaccination may not prevent viral transmission, as a percentage of vaccinated people may continue to be infected, with or without symptoms.
In Italy, almost 95% of infections by the end of July 2021 were caused by the Delta variant, which is resistant to vaccine-induced antibodies at low titers. In the absence of universal vaccination, vaccine antibody escape could lead to the emergence of newer SARS-CoV-2 variants that may altogether escape host immunity.
Breakthrough infections occur with a breakpoint between 5th and 7th month after vaccination. Such infections are often asymptomatic and may pose a risk to vulnerable populations.”
Antivirals may be urgently needed to counter this trend. Meanwhile, additional boosters may help fill the gap.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Perrella, A., Bisogno, M., D’Argenzio, et al. (2022). SARS-CoV-2 Infection Breakthrough Among the Non-Vaccinated and Vaccinated: A Real World Evidence study based on Big Data. medRxiv. doi:10.1101/2022.02.22.21266830. https://www.medrxiv.org/content/10.1101/2022.02.22.21266830v1.
- Peer reviewed and published scientific report.
Perrella, Alessandro, Massimo Bisogno, Angelo D’Argenzio, Ugo Trama, Enrico Coscioni, and Valentina Orlando. 2022. “Risk of SARS-CoV-2 Infection Breakthrough among the Non-Vaccinated and Vaccinated Population in Italy: A Real-World Evidence Study Based on Big Data.” Healthcare 10 (6): 1085. https://doi.org/10.3390/healthcare10061085. https://www.mdpi.com/2227-9032/10/6/1085.