Preeclampsia affects about 5% of pregnancies and is responsible for over 60,000 maternal deaths annually. This health condition is characterized by hypertension with mild to life-threatening end-organ complications such as eclampsia, stroke, and pulmonary edema.
Preeclampsia is linked to a systemic inflammatory response in the body. Therefore, chronic inflammation in the peripheral tissues and placenta leads to increased concentrations of inflammatory biomarkers, such as CRP, IL-6, and VCAM-1 in the blood.
In previous studies, these biomarkers, particularly IL-6 and VCAM-1, have been found to be elevated in severe cases of preeclampsia. However, the role of CRP remains unclear, as some studies report increased levels in severe cases, while others do not show significant differences.
About the study
The present study included women from the Preeclampsia Obstetric Adverse Events (PROVE) Biobank, Preeclampsia Intervention 2 (PI 2) trial at Tygerberg Hospital in South Africa, and Preeclampsia Intervention with Esomeprazole (PIE) trial cohorts. The PROVE biobank aimed to facilitate preeclampsia research, while the PIE and PI 2 trials were randomized controlled trials testing new treatments for pre-term preeclampsia.
The study enrolled women diagnosed with preeclampsia, based on the International Society for the Study of Hypertension in Pregnancy (ISSHP) criteria, and significant proteinuria. Blood samples were collected from women before delivery; however, those participating in intervention trials involving esomeprazole or metformin extended-release (ER) were excluded from the study.
The participants were grouped based on their preeclampsia complications including without end-organ complications, with one end-organ complication, and with multiple end-organ complications from various systems. Severe hypertension could be present in any group and specific complications were defined for each group.
Blood samples were collected and analyzed through enzyme-linked immunosorbent assay (ELISA) for VCAM-1, IL-6, and CRP. Statistical analyses included unadjusted and adjusted comparisons using analysis of variance (ANOVA) and analysis of covariance (ANCOVA), respectively, on log-transformed biomarker values. Missing values were replaced and a sensitivity analysis was performed.
All tests were two-sided and statistical analyses were conducted using a statistical package for social science (SPSS) and statistical analysis system (SAS) software. The results were illustrated using scatter plots.
Study results
The study included a total of 183 women, each of whom were categorized based on the severity of their preeclampsia and presence of end-organ complications. Among these individuals, 119 women experienced preeclampsia without any end-organ complications.
In contrast, 49 women presented with one end-organ complication, thus indicating a more severe form of the disease. Furthermore, 15 women experienced multiple end-organ complications.
Women who suffered from end-organ complications were more likely to be younger, have a higher body mass index (BMI), and nulliparous. Among women with one end-organ complication, the time from sampling to delivery was comparatively shorter. Furthermore, women experiencing multiple end-organ complications were significantly more likely to deliver a stillborn child.
In women with one end-organ complication, IL-6 plasma concentrations showed a 1.5-fold increase; however, this was not statistically significant in adjusted analyses. Comparatively, patients with preeclampsia and multiple end-organ complications had a significant 4.9-fold increase in IL-6 as compared to those without end-organ complications.
When compared to one end-organ complication, multiple complications had a 3.2-fold increase in IL-6. The sensitivity analysis confirmed these findings, with a borderline significant 2.2-fold increase in IL-6 for one end-organ complication as compared to no complications.
Upon comparing VCAM-1 plasma concentrations, women with one end-organ complication showed a 1.4-fold increase as compared to those without end-organ complications. Similarly, women with multiple end-organ complications also exhibited a 1.7-fold increase as compared to women without end-organ complications. However, there was no difference in VCAM-1 concentrations between one and multiple end-organ complications.
No difference in the plasma concentrations of CRP was observed between the groups after adjusting for confounding factors.
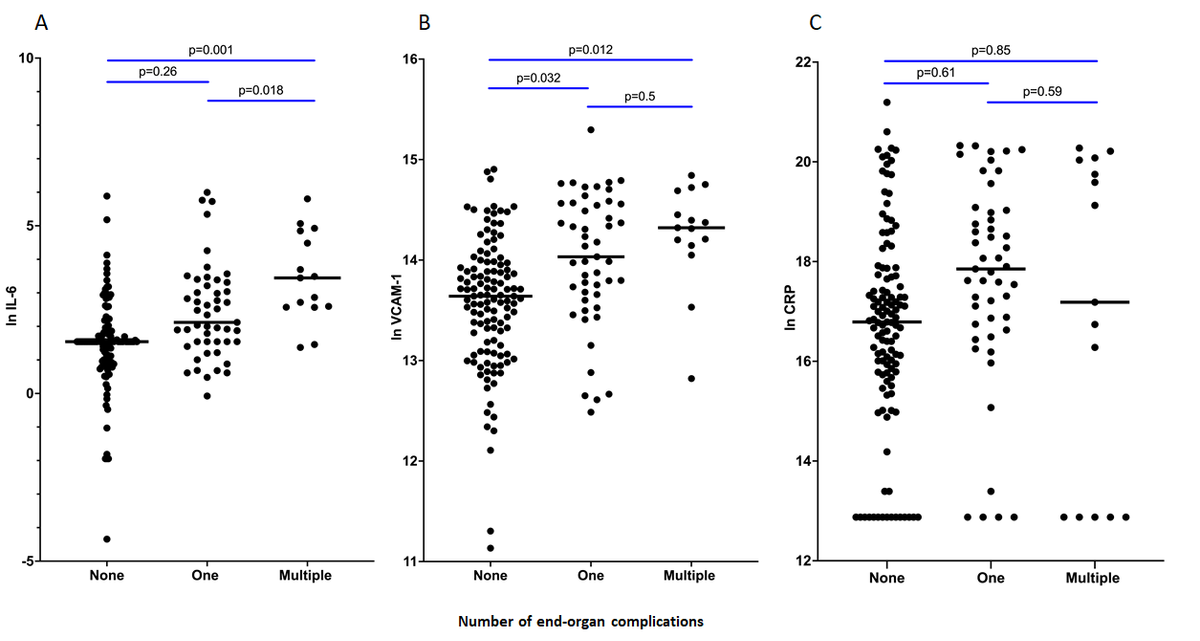 Scatter plots of log-transformed plasma concentrations of IL-6 (A), VCAM-1 (B) and CRP (C).
Scatter plots of log-transformed plasma concentrations of IL-6 (A), VCAM-1 (B) and CRP (C).
Discussion
Increased IL-6 levels were associated with the severity of end-organ involvement in preeclampsia, thus providing evidence of worsening disease severity. Other studies, often smaller and less specific in their definitions of severity, have shown varying results.
The present study, which focused on end-organ complications, was the first to demonstrate the clear association between IL-6 levels and number of end-organ complications, independent of severe hypertension.
Higher VCAM-1 concentrations were also linked to end-organ dysfunction in preeclampsia, which supports previous findings. The present study's strict criteria for defining end-organ involvement adds strength to this association as compared to studies with less specific indicators of severity.
In contrast to IL-6 and VCAM-1, the researchers did not observe any differences in plasma CRP concentrations with end-organ complications. Other studies have shown conflicting results, possibly due to their focus on severe hypertension and other multiple symptoms as indicators of severity, rather than specific end-organ complications.
Overall, this study provides a valuable understanding of the role of circulating inflammatory biomarkers in preeclampsia and their association with disease severity. The larger sample size and strict definitions of end-organ complications contribute to the robustness of these findings.
Conclusions
Among women with preeclampsia with end-organ complications, IL-6 and VCAM-1 levels were elevated, while CRP levels showed no significant difference. These findings suggest that IL-6 and VCAM-1 might play crucial roles as disease drivers in preeclampsia and could potentially serve as candidate biomarkers for diagnosing and predicting end-organ complications related to this condition.

 *Important notice: Research Square publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: Research Square publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.