Limb movement is achieved through the massive loads imposed by the muscles on bones. Such mechanical loading is essential, not only for locomotion and exercise but also to enable the maintenance of posture against gravity.
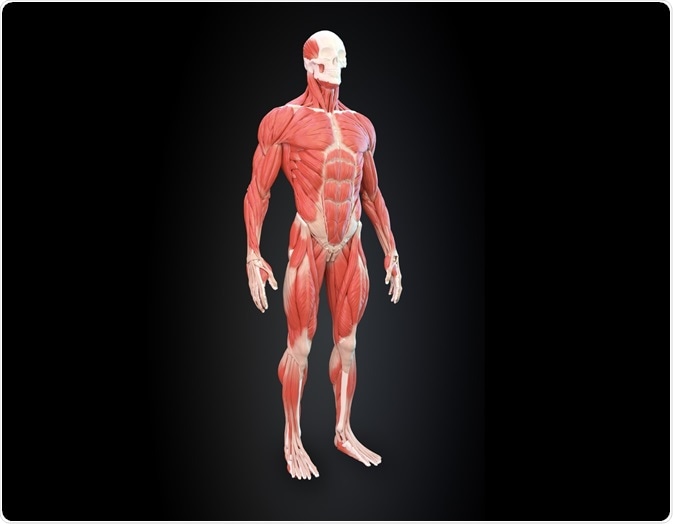 Image Credit: Mopic / Shutterstock.com
Image Credit: Mopic / Shutterstock.com
The forces exerted by muscle on bone have been identified as a key factor in the control and adaptation of the bone mass as well as its underlying microarchitecture1. The bone trabeculae in the hip bone, for example, follow the stress lines that are determined by the forces exerted on the bone by gravity and muscle loading.
Since bone and muscle mass has shown such close association, it follows that a reduction in the forces exerted by muscle on bone, as occurs naturally with advancing age, could also impact bone structure and health.
Of particular concern is the possibility that muscle wastage may give rise to a reduction in bone mass. Although bone loss can be readily evaluated using techniques such as histomorphometry, X-ray microcomputed tomography (micro-CT), texture analysis, and dual-energy absorptiometry, it is more difficult to quantify muscle changes.
To investigate whether there is a correlation between muscle wastage and bone mass, novel techniques for measuring muscle mass are being developed.
Effects of aging on muscle and bone mass
Muscle mass and muscle function naturally decline as part of the aging process. This general, progressive loss of muscle strength and physical performance with advancing age is known as sarcopaenia2.
Age-related reduction in muscle mass can be further augmented through adaptation to reduced usage. Research into sarcopenia indicates that there is an associated effect on bone mass as muscle mass declines. For example, men with sarcopenia were found to have significantly lower bone mineral density and were more likely to have osteoporosis than men who had not yet developed sarcopaenia3.
The possibility that immobilization and reduced muscle usage provoke bone loss, as exemplified in patients experiencing para- or tetraplegia4, has been explored for many years but methodological limitations have thwarted full investigation of the association.
Advances in space research studying the physiological effects of microgravity have accelerated the development of animal models of disuse-induced bone loss5. However, accurate assessment of muscle mass in vivo has proved to be a challenge.
Evaluating muscle mass in vivo
Precise measurement of muscle mass is desirable, to assess risk among the elderly and facilitate disease diagnosis and treatment. Although there are many different methods available for determining the amount of body muscle mass, they are all estimations based on different assumptions and have varying degrees of accuracy.
Techniques include bioelectrical impedance analysis, body scannings, such as dual-energy X-ray absorptiometry (DEXA), magnetic resonance imaging (MRI), computed tomography, and calculation, such as 24-hour urinary excretion of creatinine. However, muscle mass can only be accurately quantified by direct measurement post-mortem, which is obviously of little practical value.
The available array of very different tools for assessing muscle mass means that no single technique is routinely used by all clinicians. The heterogeneity of tools and the ranges of cut-off values used to evaluate sarcopenia mean that the data collected cannot all be consolidated to investigate associated effects6.
Research continues to identify an accurate, non-invasive methodology for reliable quantification of muscle mass. The development of novel computed tomography techniques that enable enhanced contrast of soft tissues have focussed attention on this tool for accurate, non-invasive evaluation of muscle mass.
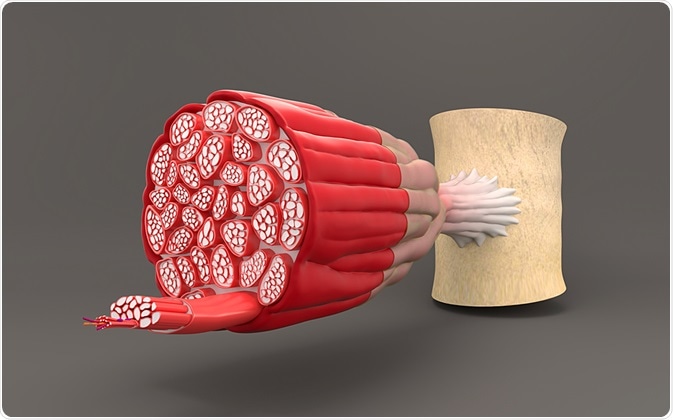 Image Credit: Anton Nalivayko / Shutterstock.com
Image Credit: Anton Nalivayko / Shutterstock.com
Assessment of muscle mass using micro computed tomography
Computed tomography has been widely studied for the determination of muscle mass, but before contrast enhancement, it was only possible to measure all soft tissues. This was because the muscle could not be adequately distinguished from other soft tissues7,8.
Advances in computed tomography imaging of muscle fibers that enable differentiation of the various types of soft tissue have re-ignited interest in this tool for the determination of muscle mass. The technique has recently been used in a study evaluating the effects of paralysis on bone density in a Clostridium botulinum toxin A (BTX) mouse model (n=21)9.
BTX blocks the release of acetylcholine at the neuromuscular synapse to induce transient paralysis of the injected muscles. It has been shown not to have a systemic effect in the mouse10.
BTX was used to paralyze a single hind limb in the mouse; the other hind limb served as a direct control. The musculature and trabecular bone volume of both limbs were then imaged before injection and 7-, 14-, 21-, 28-, 56- and 90-days post-injection by micro-CT with HgCl2 contrast enhancement using a Skyscan 1172 micro-CT equipped with an X-ray tube. At every assessment, 3 mice were sacrificed to enable direct measurement of muscle mass.
The microCT determinations of muscle mass were compared with values obtained directly via post-mortem dissection. Changes in muscle mass were related to the changes observed in bone volume.
The cross-sectional areas of gastrocnemius and quadriceps muscle were significantly lower in the paralyzed limb from 7 days after BTX injection. The greatest decrease was recorded at 21 days for the gastrocnemius muscle and 28 days for the quadriceps muscle.
Recovery of muscle mass began at 56 days in the quadriceps and at 90 days in the gastrocnemius. Bone volume was also shown to decrease in the paralyzed limb and reached maximal loss at 56 days after BTX injection.
Bone volume was seen to start increasing again at 90 days. Similar results were obtained with the anatomical method and significant correlations were obtained between the two methods.
The latest research demonstrated that accurate, non-invasive quantitative analysis of muscle loss and recovery is possible by micro-CT using a metallic contrast agent. It also confirmed that bone loss occurs secondary to muscle wastage and showed parallel recovery of muscle and bone once the effects of the BTX had worn off.
References
- Chappard D, t al. Morphologie 2008;92:162–170.
- Cruz-Jentoft AJ, et al. Age Ageing 2010;39:412–423.
- Verschueren S, et al. Osteoporos Int 2013;24:87–98.
- Minaire P, et al. Calcif Tissue Res 1974;17:57–73.
- Jee WS, Ma Y. Morphologie 1999;83:25–34.
- Bruyère O, et al. European Geriatric Medicine 2016;7(3):243-246.
- Bouvard B, et al. Bone 2012;50:858–864.
- Manske SL, Boyd SK, Zernicke RF. Calcif Tissue Int 2010;87:541–549.
- Libouban H, et al. Calcif Tissue Int 2018;102:695–704.
- Lodberg A, et al. Bone Rep 2015;2:59–67.
About Bruker BioSpin - NMR, EPR and Imaging

Bruker BioSpin offers the world's most comprehensive range of NMR and EPR spectroscopy and preclinical research tools. Bruker BioSpin develops, manufactures and supplies technology to research establishments, commercial enterprises and multi-national corporations across countless industries and fields of expertise.