Introduction
What is the endometrium?
Endometrial cellular and molecular biology
Endometrial inflammation and immune function
Endometrial microbiota and local immune interactions
Endometrial metabolism and aging
The endometrium, metabolic instability, and cancer risk
Research gaps and future directions
References
Further reading
The endometrium is a highly dynamic tissue, regulated by mitochondrial metabolism, immune signaling, hormonal balance, and microbial interactions, which collectively influence aging, inflammation, fertility, and disease risk. Emerging evidence suggests that mitochondrial dysfunction, chronic endometritis, microbiota dysbiosis, and metabolic instability may contribute to impaired endometrial health and endometrial cancer development beyond traditional reproductive contexts.
 Image Credit: crystal light / Shutterstock.com
Image Credit: crystal light / Shutterstock.com
Introduction
The endometrium is a dynamic tissue shaped by mitochondrial function, hormonal regulation, immune surveillance, and microbial balance.1,3 Age-related mitochondrial dysfunction, chronic inflammation, and cellular senescence alter the structure and metabolic resilience of the endometrium. Chronic inflammatory conditions like chronic endometritis (CE) and microbiota dysbiosis similarly create disruptions in immune homeostasis and tissue integrity that contribute to larger gynecologic pathologies, including implantation failure, recurrent pregnancy loss, abnormal uterine bleeding, and some endometrial diseases.2,3
This article explores the role of the endometrium in metabolism, immune regulation, inflammation, microbiota balance, aging, and chronic gynecological conditions, reinforcing its crucial broader importance in women’s health.
What is the endometrium?
The endometrium has two distinct layers, of which include its functional layer, which undergoes cyclic growth and shedding with each menstrual period, as well as the basal layer, which is responsible for regenerating the endometrium after menstruation. Within the endometrium are both luminal and glandular epithelial layers, as well as stroma, immune cells, and different types of vascular tissue that are dynamically remodeled during the 28-day menstrual cycle. Under the coordinated influence of estradiol and progesterone, the endometrium undergoes cyclic proliferation, secretory transformation, angiogenesis, and immune modulation to support tissue renewal and maintain uterine physiological homeostasis.1,3
Endometrial cellular and molecular biology
As age progresses, mitochondrial deoxyribonucleic acid (DNA) is more likely to mutate, thereby increasing the risk of electron transport chain dysfunction and reduced adenosine triphosphate (ATP) production, which leads to oxidative stress and disruption of cell homeostasis. However, age-associated mitochondrial DNA alterations may also arise from replication errors, and direct human endometrial evidence remains limited. High levels of reactive oxygen species (ROS) perpetuate genomic instability, epigenetic modifications, and cellular senescence, especially in stromal and epithelial cells. At lower levels, ROS may also activate adaptive stress-response pathways, a phenomenon known as mitohormesis, which can transiently enhance cellular resilience.1
Mitochondrial quality control mechanisms, including fission-fusion dynamics, autophagy, and mitophagy, are dysregulated, further accelerating tissue aging. Despite these vulnerabilities, the endometrium retains remarkable regenerative capacity through cyclic remodeling by stem or progenitor cells, mitochondrial biogenesis, and tightly regulated growth factor and hormonal signaling pathways.1
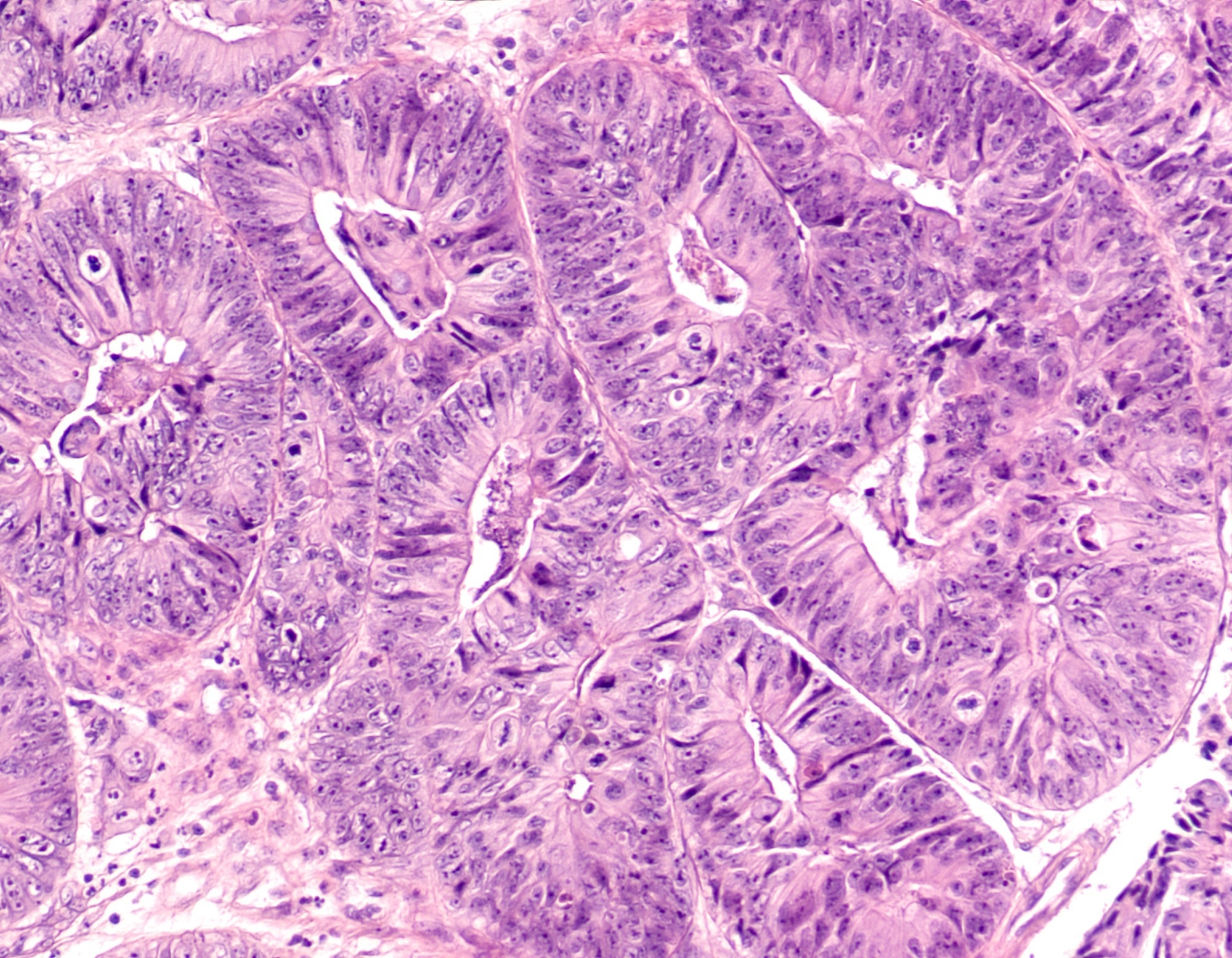 Image Credit: David A Litman / Shutterstock.com
Image Credit: David A Litman / Shutterstock.com
Endometrial inflammation and immune function
Endometrial inflammation is tightly regulated by a complex immune network that maintains uterine homeostasis while permitting implantation. The endometrium contains abundant innate and adaptive immune cells, including macrophages, dendritic cells, uterine natural killer cells, neutrophils, and T lymphocytes, that fluctuate throughout the menstrual cycle and support tissue remodeling, angiogenesis, and immune tolerance.2,3
CE is a persistent inflammatory disorder characterized by plasma cell infiltration, microbial imbalance, and elevated pro-inflammatory cytokines that disrupt endometrial function and tissue remodeling.2,3 CD138 immunohistochemistry is commonly regarded as the diagnostic gold standard, while hysteroscopy and molecular microbiological testing can provide complementary information.2 However, diagnostic thresholds remain variable, and hysteroscopic findings alone can increase the risk of overdiagnosis.2 Microecological imbalance resulting from microbial-immune interactions may include endometriosis, endometrial polyps or adenomyosis, endometrial hyperplasia, as well as endometrial and cervical cancer.
Chronic inflammation, hormonal dysregulation, and cellular senescence due to disrupted age-related mitochondrial physiology can also lead to increased susceptibility to endometrial thinning, abnormal uterine bleeding, and loss of reproductive capability. Collectively, these disorders highlight that endometrial dysfunction, driven by inflammation, microbial dysbiosis, and aging-related molecular changes, has significant clinical implications independent of implantation or pregnancy.1,2,3
Endometrial microbiota and local immune interactions
A balanced uterine microbiome is characterized by the presence of symbiotic bacteria, such as Lactobacillus, that support mucosal defense, enhance barrier integrity, and modulate immune cell maturation and cytokine production. The endometrial microbiota is generally lower in abundance and more diverse than the vaginal microbiota and may not simply represent contamination from the lower reproductive tract.3 Microbial ligands activate pattern-recognition receptors like Toll-like receptors to initiate signaling pathways that regulate inflammatory responses and antimicrobial peptide secretion.2,3
Uterine dysbiosis is characterized by reduced Lactobacillus dominance and the overgrowth of pathogenic bacteria, contributing to persistent immune activation, elevated pro-inflammatory cytokines, and impaired endometrial receptivity. This microbial imbalance has been implicated in chronic endometrial inflammation, implantation failure, and broader pelvic pathology beyond fertility contexts.2,3 CE is also associated with reduced expression of implantation-related markers such as HOXA10, HOXA11, leukemia inhibitory factor, IGFBP-1, and integrin αvβ3, which may impair embryo adhesion and the window of implantation.2
The endometrium is an active metabolic tissue with significant energy requirements to regenerate and differentiate each month and respond to hormones. The combination of aging, mitochondrial DNA mutations, altered electron transport chain function, and decreased ATP production leads to ROS generation, which disrupts cellular homeostasis.1
Age-related reductions in estrogen and progesterone signaling can impair mitochondrial function, autophagy, mitophagy, and hormone-responsive gene expression, thereby leading to oxidative stress and hormonal imbalances.1 These cellular responses diminish endometrial thickness, thereby limiting its ability to successfully accept an embryo during implantation while increasing the risk of local inflammation. Thus, reductions in mitochondrial function may contribute to abnormal uterine bleeding, menopausal transition changes, and other symptoms related to endometrial dysfunction associated with age.1
Endometrial Cancer: What You Need to Know but No One Talks About!
Several factors increase the risk of endometrial cancer, which is one of the most common malignancies to affect women in developed countries, some of which include age, genetics, excessive estrogen exposure, and hormonal patient characteristics like late menopause, nulliparity, and early onset age for menstruation4. The presence of metabolic syndrome (MS), which is characterized by insulin resistance, hyperglycemia, obesity, and arterial hypertension, is increasingly studied for its role in promoting carcinogenesis, particularly within the female reproductive tract.
Obesity is a key factor that increases the risk of endometrial cancer, with this association largely attributed to fluctuations in metabolic processes involving glucose, insulin, and other factors. Metabolic instability has been proposed as a potential emerging framework for understanding endometrial cancer risk beyond obesity alone.4 Recent evidence suggests that repeated variability in weight, glucose, insulin, adipokines, and sex hormones may create a pro-inflammatory, estrogen-sensitive, and proliferative endometrial microenvironment even in some women without obesity.4 This metabolic instability creates a state of chronic cellular stress and inflammation that increases the proliferative activity of endometrial cells by altering repair, apoptotic, and hormonal signaling pathways.4
Rather than being explained by body weight alone, endometrial cancer risk may also reflect broader metabolic and hormonal imbalance.4
Research gaps and future directions
CE remains underdiagnosed due to the lack of standardized diagnostic criteria and a subtle clinical presentation, underscoring the need for improved biomarkers and standardized protocols.2 New molecular methods, including immunohistochemical markers, cytokine profiling, gene expression arrays, and microbiome sequencing, are increasingly being used to distinguish the pathological features of normal and dysfunctional endometrium.
Mitochondrial dysfunction, hormonal dysregulation, and cellular senescence associated with aging are understudied factors that contribute to endometrial decline beyond their effects on fertility. In the future, the interdisciplinary integration of gynecology, immunology, microbiology, and metabolic biology will be essential to advance the development of targeted diagnostics and therapeutic strategies that support lifelong endometrial health.1,2,3
References
- Kobayashi, H., Nishio, M., Umetani, M., et al. (2025). Endometrial Aging and Reproductive Decline: The Central Role of Mitochondrial Dysfunction. International Journal of Molecular Sciences 26(11). DOI: 10.3390/ijms26115060. https://www.mdpi.com/1422-0067/26/11/5060
- Lucan, M., Sandor, M., Bodog, A., et al. (2025). Chronic Endometritis: A Silent Contributor to Infertility and Reproductive Failure - A Comprehensive Review. Reproductive Medicine 6(2). DOI: 10.3390/reprodmed6020014. https://www.mdpi.com/2673-3897/6/2/14
- Zhu, N., Yang, X., Liu, Q., et al. (2022). “Iron triangle” of regulating the uterine microecology: Endometrial microbiota, immunity and endometrium. Frontiers in Immunology 13. DOI: 10.3389/fimmu.2022.928475. https://www.frontiersin.org/journals/immunology/articles/10.3389/fimmu.2022.928475/full
- Sukhanova, M. A., Muraviev, S. Y., Tarabrin, E. A., et al. (2025). The Role of “Metabolic Instability” as a New Risk Criterion in the Pathogenesis of Endometrial Cancer. Cancers 17(23); 3840. DOI: 10.3390/cancers17233840. https://www.mdpi.com/2072-6694/17/23/3840
Further Reading
Last Updated: May 11, 2026