All these are different cells present in the immune system which are involved in fighting foreign bodies (such as microbes) or clearing dead cells.
Phagocytes and Phagocytosis
When the body is breached by infectious agents, such as certain microbes, they encounter various parts of the immune system. In general, phagocyte is a broad term which refers to any cell which carries out phagocytosis.
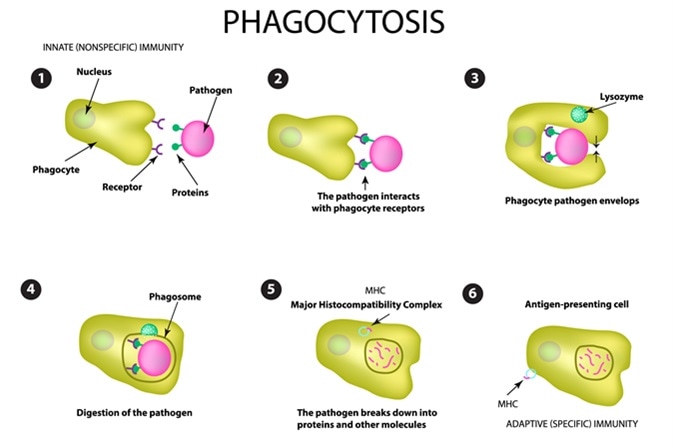
Phagocytosis. Image Credit: Timonina / Shutterstock
In phagocytosis, phagocytes engulf large prokaryotic cells, such as bacteria, or eukaryotic cells, such as yeast cells or dead cells (>0.5 µm) to kill them, or small particles to remove them from the circulation.
This process was first described by Metchnikoff, who introduced the word “phagocyte” while conducting his work on the water flea, Daphnia.
Although in lower eukaryotes phagocytosis is mainly used to acquire nutrients, in higher eukaryotes phagocytes are mainly involved in killing invading pathogens, thus forming a part of the immune system.
Macrophages
Macrophage is a type of white blood cell which is a phagocyte. They are scavengers which constantly move around to remove dead cells and foreign bodies such as pathogenic microbes; this occurs by the production of compounds such as nitric oxide.
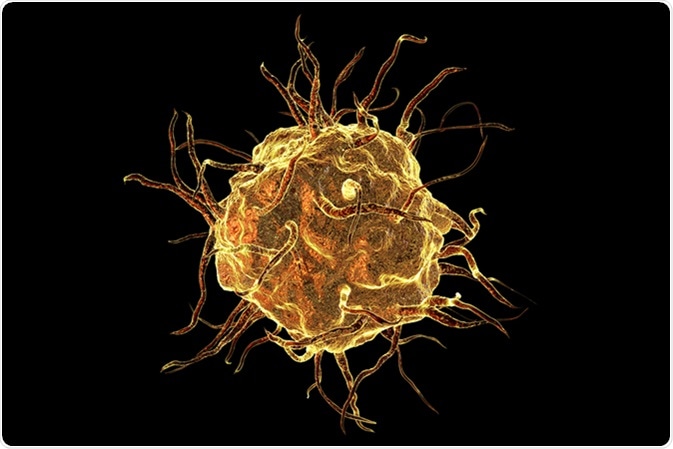
Macrophage cell isolated on black background, monocyte, close-up view of immune cell, 3D illustration. Image Credit: Kateryna Kon / Shutterstock
They do not specifically act against a particular antigen and are thus considered to be a part of the innate immune system.
Innate immunity refers to the parts of the immune system which are activated first, thus forming the first line of defense against pathogens.
They are derived from monocytes, which in turn arise from hematopoietic stem cells in the bone marrow.
They can either be fixed macrophages or wandering macrophages; fixed macrophages reside in areas more susceptible to pathogen invasions, such as the lungs or the intestine.
Wandering macrophages move around in the bloodstream and lymph nodes to detect invaders. Thus, they can be found in several regions of the body.
Macrophages produce inflammatory molecules, like cytokines, and this can activate other immune responses.
Also, macrophages can form a bridge between the innate and adaptive immune systems; macrophages are able to “process and present” specific antigens to T-cells, which are key cells of the adaptive immune system.
Neutrophils
Neutrophils are the most abundant white blood cell in humans and arise from granulocytes. They are also phagocytic in nature, and Metchnikoff called neutrophils the “archetypal phagocyte”.
Neutrophils are the first immune cells to be recruited, which can be through the cytokines produced by macrophages. Therefore, neutrophils are also part of the innate immune system.
Antimicrobial action of neutrophils is more potent than that of macrophages, and they have several microbicidal methods.
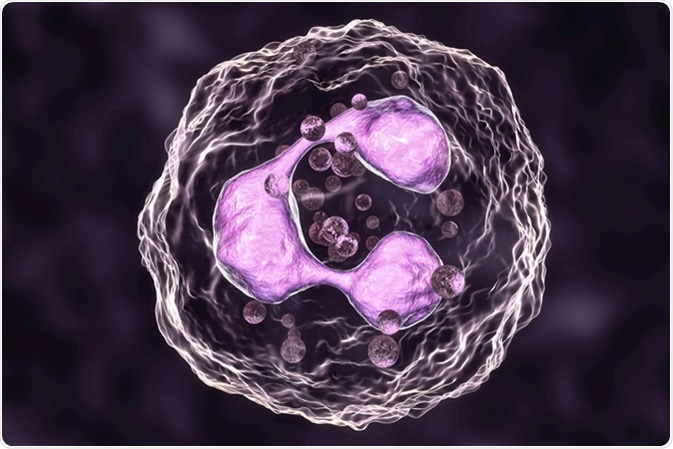
Neutrophil, a white blood cell, 3D illustration. Image Credit: Kateryna Kon / Shutterstock
One of the ways they kill a foreign object is by generating reactive oxygen species or by using several antimicrobial proteins.
Myeloperoxidase is a critical enzyme present in neutrophils which is involved in oxidative antimicrobial activity of neutrophils.
Neutrophils can also release antimicrobial factors, as well as form extracellular traps (NETs) to “catch” pathogens.
Eosinophils
Eosinophils are also a type of white blood cell which also arise from granulocytes. They have granules that can be stained by eosin. They, like other blood cells, are generated in bone marrow during hematopoiesis.
Eosinophils are part of the innate immune system and act against foreign invasions by releasing inflammatory molecules and cytotoxic cationic proteins.
The main function of eosinophils is against larger parasites which cannot easily be phagocytosed. However, they are also involved in the development of asthma and allergy and their numbers are higher in those who have asthma or allergies; the release of inflammatory molecules and the cytotoxic cationic proteins not only destroy parasites, but also cause damage to host tissue.
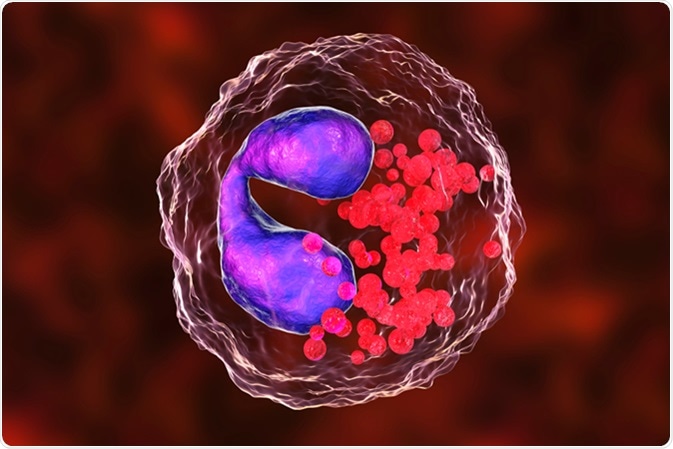
Eosinophil, a white blood cell, 3D illustration. Image Credit: Kateryna Kon / Shutterstock
Differences Between Nutrophils and Eosinophils
Both neutrophils and eosinophils have a multi-lobed nucleus, which differentiates them from other white blood cells like macrophages, monocytes and lymphocytes.
Eosinophils can be stained by eosin which leads to a brick-red stain, while neutrophils are stained a pink color.
Neutrophils are more abundant in the body; 40-75% of white blood cells are neutrophils, while only 1-6%of white blood cells are eosinophils. Eosinophils are larger; the diameter of neutrophils is 9 µm, while the diameter of eosinophil is 12–17 µm.
Neutrophils do not last for a long time, surviving for 5-90 hours, while eosinophils last 8–12 hours in circulation, or 8–12 days in tissues.
Although both neutrophils and eosinophils are myeloid cells (along with monocytes/macrophages and others), they differ in terms of their structure and mode of action against invasions; neutrophils are phagocytic and thus their part in the innate immune response is through the phagocytosis of small microbes, while eosinophils release inflammatory molecules and cytotoxic cationic proteins to target large parasites.
Also, eosinophils can be activated by non-pathogens, leading to a damaging inflammatory response such as in asthma and allergies.
Further Reading
Last Updated: Dec 8, 2022