Researchers from Massachusetts General Hospital have used a microfluidic device to incorporate neuroinflammation into a model of Alzheimer’s disease. It is hoped that the development will improve our ability to screen for potential therapies.
Previously, the team developed an “Alzheimer’s in a dish” culture system that mimics the pathology underlying Alzheimer’s disease. However, the system did not include neuroinflammation, the main driver of brain cell death.
As reported in the journal Nature Neuroscience, technology developed by co-senior author Hansang Cho has now incorporated glial cells called astrocytes that support nerve cells and provide some immune function.
Our original Alzheimer’s-in-a-dish system recapitulated the plaques and tangles typically seen in the brains of patients with Alzheimer's disease, but did not induce neuroinflammation."
Rudolph Tanzi, Co-Author
In 2014, the team published a paper in Nature describing a 3-D, gel-based culture system that formed amyloid-beta plaques and neurofibrillary tangles in human neurons with gene variants associated with early-onset familial Alzheimer’s disease (FAD).
That study confirmed that it is the deposition of the plaques that initiates the formation of tangles with misfolded tau protein.
Now, Cho’s technology has updated the system with a microfluidic device made up of two chambers that measures the migration of microglia as they move from an outer chamber into an inner chamber loaded with amyloid.
Cho and colleagues used the system to grow neural stem cells with FAD variants in the central chamber.
The team found that several weeks later, the neurons and astrocytes that had differentiated had increased levels of amyloid-beta, tau and the inflammatory factors known to play a role in the neuroinflammation that occurs in Alzheimer’s.
As shown in the image below, six days after activated microglia (red) were added to the outer chamber of the new microfluidic device, the inflammatory cells migrate through channels into the inner chamber, containing cultured neurons and astrocytes (green) with gene variants associated with familial Alzheimer's disease.
Inflammatory factors such as TNF-alpha and Il-6 were also significantly increased and after six days, the number of neurons and astrocytes had decreased by 20%.
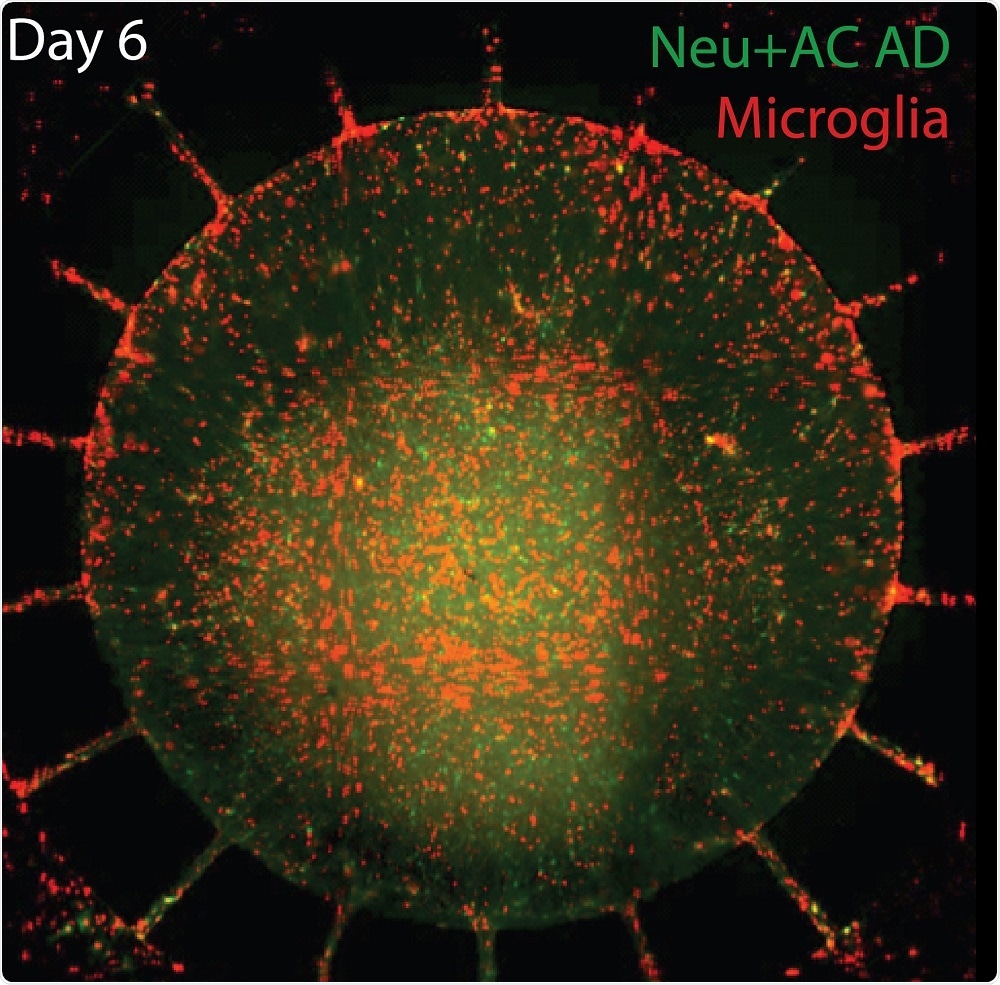 (Image Credit: Joseph Park, Doo Yeon Kim, Rudolph E. Tanzi, and Hansang Cho; Genetics and Aging Research Unit, MassGeneral Institute for Neurodegenerative Disease)
(Image Credit: Joseph Park, Doo Yeon Kim, Rudolph E. Tanzi, and Hansang Cho; Genetics and Aging Research Unit, MassGeneral Institute for Neurodegenerative Disease)
"This system should help us better understand the timeline by which these pathological events lead to dementia and enable us to screen for drugs that stop plaque deposition, tangle formation and the resultant neuroinflammation," says Tanzi.