People who need daily injections such as those with Type 1 diabetes would be happy to know that researchers at the MIT have come up with a specially devised pill that could deliver injections when swallowed. They have named it self-orienting millimeter scale applicator, or SOMA. The results of their experiment were published in the latest issue of the journal Science.
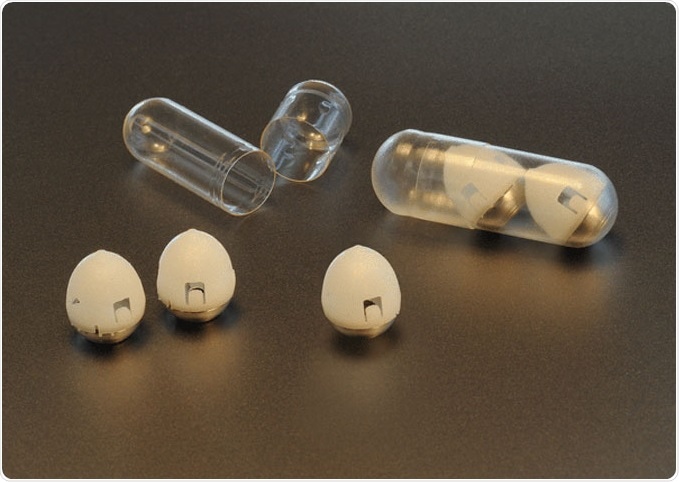
MIT-led research team has developed a drug capsule that could be used to deliver oral doses of insulin. Image: Felice Frankel
The researchers have developed SOMA - these pea-sized capsules that contain a small needle that is made up of solid, compressed insulin. When ingested this insulin gets injected into the stomach wall. The team has already begun testing these pill injections on pigs and found it to be consistently effective in delivering the doses of insulin needed by a diabetic patient.
According to Giovanni Traverso, co-author and assistant professor at Harvard Medical School-affiliated Brigham and Women’s hospital, “Our motivation is to make it easier for patients to take medication, particularly medications that require an injection. The classic one is insulin, but there are many others.” He explained that taking insulin injections daily can be a painful ordeal for diabetics.
The team explains that the idea for this pill injection came from a species of leopard tortoise seen in Africa. This tortoise has a dome like shell which is high and allows it to set itself right when it rolls on its back. The idea also came from the Weeble-Wobble toy that can right itself on its own. The capsule too is dome shaped so that it can right itself to allow the injection to face the stomach wall. First author Alex Abramsom, an MIT graduate student said, “If they are pushed over but are able to orient themselves. The leopard tortoise also had a flat base, which makes it difficult to push over, and it can roll over easily if it ends up on its back. So let's say a person was leaning over when the device was about to insert. The device will configurate and orient itself every single time so it contacts the lining of the stomach.”
A self-orienting millimeter-scale applicator (SOMA) for oral delivery of insulin and other biologics
The needle contains a compressed spring which is held back with a disc of sugar. As the capsule dissolves with the water and stomach acids, the spring is released and the injection is paced onto the stomach wall from where it works. Abramsom explains, “When the spring releases, it releases its kinetic energy all at once.”
Because of the lack of pain sensors in the stomach wall, this injection is painless. Within the next hour the needle dissolves in blood and is eliminated. The spring and the other parts of the capsule are eliminated though the digestive system without causing problems. In their experiments, the researchers could inject up to 5 milligrams of insulin successfully into the pigs’ stomach walls. The insulin delivered is solid in form. “Instead of liquid, we wanted to make it solid because you can fit a lot more in the pill in solid form than in liquid,” explained Dr Traverso.
The researchers are now perfecting their system by trying them on pigs and dogs and within the next three years, they hope human clinical trials could begin. They are presently working with working with pharmaceutical company Novo Nordisk to develop SOMA.
The Centers for Disease Control and Prevention (CDC) says that 30.3 million Americans at present suffer from diabetes mellitus and many of these need regular insulin shots. Senior author Dr Robert Langer, a member of MIT's Koch Institute for Integrative Cancer Research in a statement said, “We are really hopeful that this new type of capsule could someday help diabetic patients and perhaps anyone who requires therapies that can now only be given by injection or infusion.”