Bone marrow-derived cells play a role in changes to the mouse uterus before and during pregnancy, enabling implantation of the embryo and reducing pregnancy loss, according to research published September 12 in the open-access journal PLOS Biology. Although the study was done in mice, it raises the possibility that dysfunction of bone marrow-derived progenitor cells may contribute to implantation failure and pregnancy loss in women.
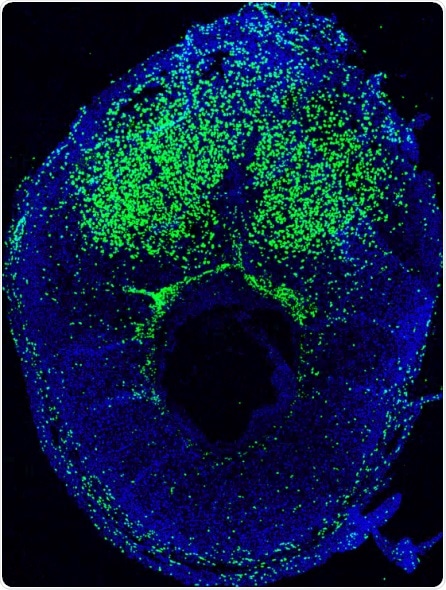
An immunofluorescent section of a pregnant mouse uterus on embryonic day E9.5 showing the distribution of bone marrow-derived cells, labeled with green fluorescent protein (GFP). Cell nuclei are labeled with DAPI (blue). Numerous bone marrow-derived cells are recruited to the pregnant uterus where they contribute to embryo implantation and pregnancy. Credit: Reshef Tal
Bone marrow progenitors can become either blood or tissue cells. Within the uterus they differentiate into endometrial tissue cells in the lining of the womb, but until now it was not known if they have a function in pregnancy. Reshef Tal and colleagues from Yale School of Medicine developed a bone marrow transplantation protocol that preserved ovary and reproductive function, allowing them for the first time to track these cells in pregnancy, showing that during pregnancy cells from the bone marrow were preferentially recruited to the uterus and were concentrated near the site of implantation, on the maternal side of the placenta. The authors demonstrate that after reaching the uterus, these cells proliferate and become so-called decidual cells, specialized uterine cells which are critical for nurturing the embryo and supporting its implantation.
The authors then made use of mice that lack Hoxa11, a protein which is found in uterine cells but also in bone marrow-derived progenitor cells; these mice are known to have defects in the womb lining and are unable to become pregnant. Mice with partial Hoxa11 deficiency can become pregnant but have recurrent pregnancy losses. Strikingly, the authors found that after receiving bone marrow transplants from healthy mice, the Hoxa11-deficient mice switched on genes involved in preparing the womb lining for pregnancy and became pregnant. In mice with partial Hoxa11 deficiency, bone marrow transplant from healthy mice prevented pregnancy loss resulting in normal litter numbers.
Recurrent pregnancy loss in humans affects 1-2% of couples and is usually unexplained. Hoxa11 production has been implicated in human implantation and several studies have shown that levels of Hoxa11 protein are decreased in conditions associated with pregnancy failure such as endometriosis, submucosal leiomyomas and pregnancy loss. The findings reveal the role of Hoxa11-positive bone marrow-derived progenitor cells in the mouse uterus and the authors suggest further work be done to investigate the role of these cells in human implantation and pregnancy.
The authors of the study say:
The common thinking about bone marrow in relation to pregnancy is that it is the origin of many immune cells which play important roles at the maternal-fetal interface to promote successful pregnancy. This study shows for the first time that adult bone marrow is also a source of non-immune cells in the pregnant uterus. We demonstrate that bone marrow progenitors are mobilized to the circulation in pregnancy and home to the uterus where they become decidual cells and have profound effects on gene expression in the uterine environment and ultimately help prevent pregnancy loss."
The authors go on to say, “We are currently translating these findings into humans to better understand the role that these cells play in recurrent implantation failure and recurrent pregnancy loss, two conditions that are unexplained in the majority of cases and have no effective treatment. The findings of this study open exciting new avenues for research into the cause of these conditions as well as developing new treatments for women suffering from them.”
Source:
Journal reference:
Tal, R. et al. (2019) Adult bone marrow progenitors become decidual cells and contribute to embryo implantation and pregnancy. PLOS Biology. doi.org/10.1371/journal.pbio.3000421.