A team of researchers have found that persons with schizophrenia may have lower levels of certain specific proteins that show up on their brain scans. This could help as diagnostic tools, say experts. The new study titled, “Synaptic density marker SV2A is reduced in schizophrenia patients and unaffected by antipsychotics in rats”, is published in the latest issue of the journal Nature Communications.
The study from the Medical Research Council (MRC) London Institute of Medical Sciences shows that certain proteins are needed in the brains of normal persons to form connections between neurons. These proteins are found to be depleted in brains of persons with schizophrenia.
The experts suggest that lack of effective neuronal connection within the brain due to lack of this protein could be one of the reasons why certain cognitive difficulties are seen in persons with schizophrenia. Assessment of this protein could not only open doors to new diagnostic methods, explain researchers, but also provide therapeutic targets for development of drugs for treatment of this dreaded mental illness.
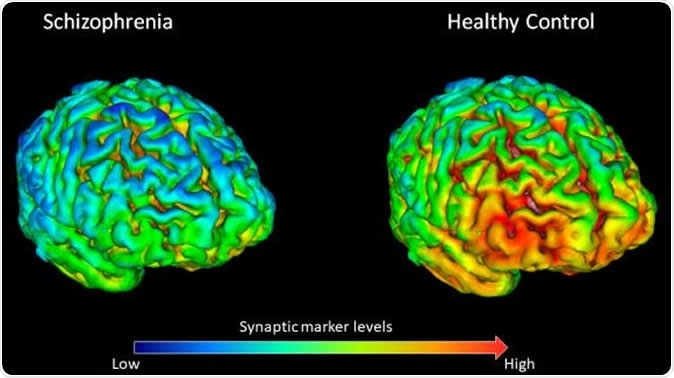
PET brain scans showing that 18 healthy volunteers (right) have on average higher levels (shown by yellow-red) of synapse marker protein SV2A than 18 participants with schizophrenia (left). Image Credit: E. Onwordi at MRC London Institute of Medical Sciences
Experts have explained that in patients with schizophrenia there are damaged or dysfunctional connections between nerves or synapses. These synapses are vital when it comes to transmission of electric signals within the brains. These problematic synapses could be half understood only from brains obtained after death of a person with schizophrenia, they wrote. There was no way a living person with schizophrenia could be studied using scans that could show the damaged synapses. Animal models that showed the damaged synapses were not close to human brains.
In this study the team looked at PET brain scans of humans with schizophrenia after having injected them with a tracer drug. This tracer would emit signals to the scanning device and the real time image of the brain could be captured. This tracer was prepared in a manner so that it could bind to a specific brain protein called the SV2A (synaptic vesicle glycoprotein 2A). the protein has been shown to be present in abundance at the synaptic nerve endings wrote the researchers.
The team included 18 adult patients with schizophrenia and 18 adults who did not have the condition. Using the tracer and the PET scans of the brain the team looked at the density of SV2A within the brains of the persons with schizophrenia compared to normal persons. Results revealed that persons with schizophrenia contained lower amount of SV2A in their frontal cortex (FC) and anterior cingulated cortex (ACC) regions of the brain. These areas are commonly involved in thought and cognitive abilities as well as planning wrote the researchers. They also added that other regions of the brain including “dorsolateral prefrontal and temporal cortices and occipital lobe” also showed lower SV2A levels.
Study leader Professor Oliver Howes of MRC London Institute of Medical Sciences, Imperial College London and King's College London, said, “Our current treatments for schizophrenia only target one aspect of the disease - the psychotic symptoms - but the debilitating cognitive symptoms, such as loss of abilities to plan and remember, often cause much more long-term disability and there's no treatment for them at the moment. Synaptic loss is thought to underlie these symptoms.” He added, “Our lab at the MRC London Institute of Medical Sciences is one of the few places in the world with this new tracer, which means we've been able for the first time to show there are lower levels of a synaptic protein in people with schizophrenia. This suggests that loss of synapses could underlie the development of schizophrenia. We need to develop new treatments for schizophrenia. This protein SV2A could be a target for new treatments to restore synaptic function.”
Study researcher Dr Ellis Onwordi, from the MRC London Institute of Medical Sciences, also added, “Schizophrenia is a highly debilitating disorder, and the therapeutic options are too limited for many patients. To develop better treatments in the future we need studies like this to shine a light on how the extraordinarily complex wiring of the human brain is altered by this disease. Having scans that can characterise the distribution of the approximately 100 trillion synapses in the living brain, and find differences in their distribution between people with and without schizophrenia, represents a significant advance in our ability to study schizophrenia.”
As an addition to their study the team wanted to look at the effects of antipsychotic medications on the brain levels of SV2A. The drugs haloperidol and olanzapine are commonly used in patients with schizophrenia. The team now administered these drugs to lab rats for 28 days and then assessed the levels of SV2A in the rat brains. The results of this short experiment showed that the drugs did not affect the levels of SV2A. This experiment also provided that the levels of SV2A in the study was lowered due to the disease and not due to the drugs that the patients were taking.
Professor Howes said, “This is reassuring as it's suggesting that our antipsychotic treatments aren't leading to loss of brain connections. Next we hope to scan younger people in the very early stages to see how synaptic levels change during the development of the illness and whether these changes are established early on or develop over time.” The team also wrote in conclusion, “These findings indicate that synaptic alterations occurs in vivo in schizophrenia, and lower SV2A levels are unlikely to be directly accounted for by antipsychotic drug treatment.”
Journal reference:
Onwordi, E.C., Halff, E.F., Whitehurst, T. et al. Synaptic density marker SV2A is reduced in schizophrenia patients and unaffected by antipsychotics in rats. Nat Commun 11, 246 (2020) doi:10.1038/s41467-019-14122-0, https://www.nature.com/articles/s41467-019-14122-0