The development and emergence of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) variants of concern that could potentially evade a vaccine-induced immune response is an ongoing concern, with the alpha (B.1.1.7), beta (B.1.351), gamma (B.1.248), and delta (B.1.614.2) lineages having largely independently evolved mutations to the spike protein and receptor binding domain that enhance transmissibility and in some cases provide mild resistance to neutralizing antibodies.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
How was the study performed?
The Pfizer-BioNTech, Moderna, and Johnson & Johnson vaccines have each been approved for emergency use by the U.S. Food and Drug Administration (FDA), with the former two being mRNA-based while the latter utilizes an adenovirus vector.
Sera were collected from individuals having received any one of these vaccines at several time points, extending from one week to three months post-vaccination. In addition, the neutralizing activity of the generated antibodies towards several SARS-CoV-2 variants was assessed.
The key mutations that characterize each of the examined lineages were identified for better representation by the pseudoviral particles utilized, expressing the unique spike protein on their surface whose structure will determine the affinity of neutralizing antibodies towards them.
Sera from individuals that had been infected with SARS-CoV-2 prior to the emergence of these variants of concern was firstly administered, with the spike protein bearing the D614G mutation common to these variants being neutralized by the sera with antibody titers of 346 at IC50.
Comparatively, titers of only 305, 71, 78, 105, and 105 were seen upon exposure to alpha, beta, delta, delta plus, and lambda variants, respectively, indicating modest resistance to neutralization in these latter strains.
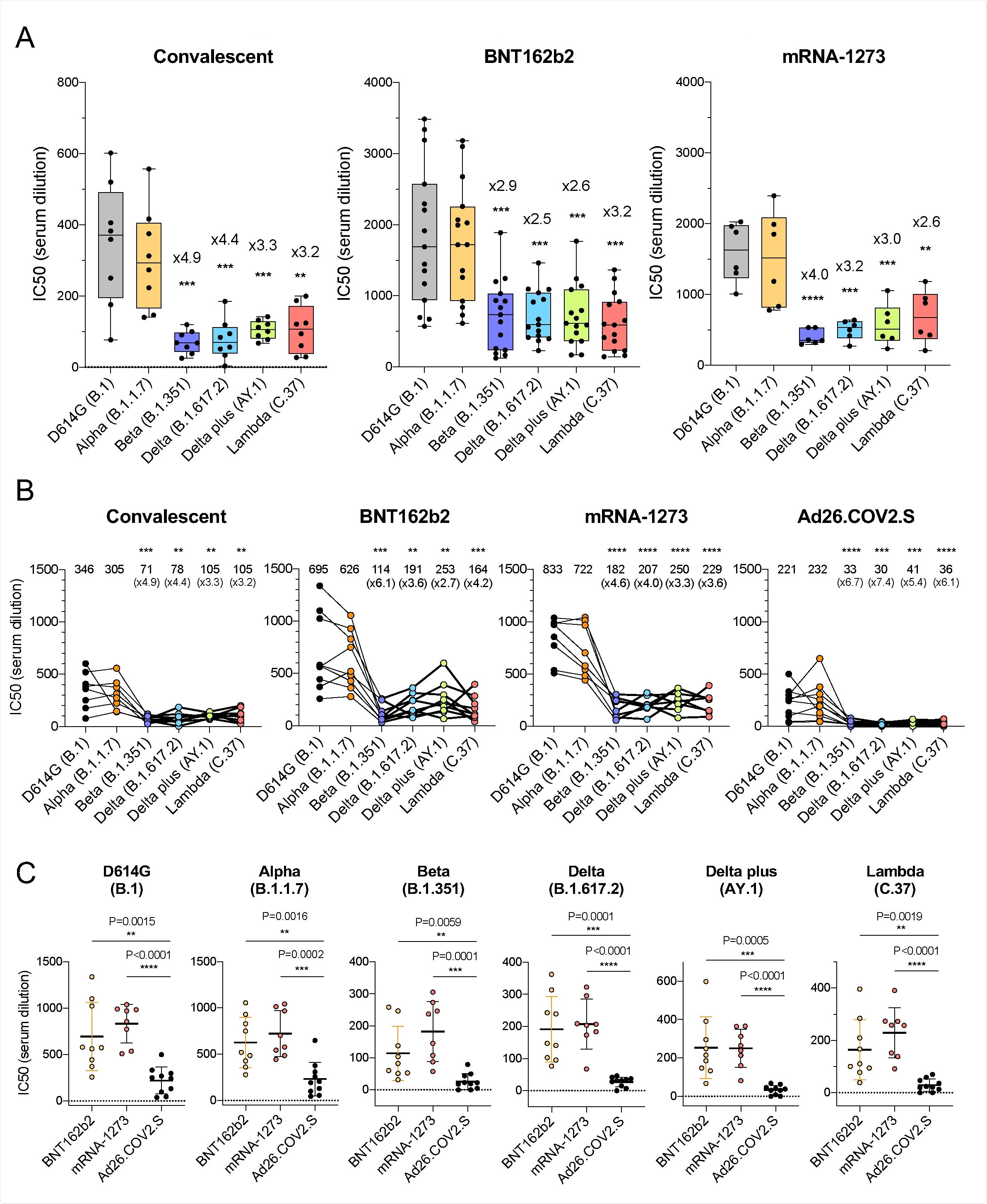
Comparison of neutralization titers of variant spike protein pseudotyped viruses by convalescent sera, antibodies elicited by BNT162b2, mRNA-1273, Ad26.COV2.S. (A) Neutralization of variant spike protein pseudotyped viruses by convalescent serum (n=8) (left). Neutralizing titers of serum samples from BNT162b2 vaccinated individuals (n=15) (middle). Neutralizing titers of serum samples from mRNA-1273 vaccinated donors (n=6) (right). The serum was collected at early time point (7 days after second immunization). The neutralization IC50 from individual donors is shown. Significance is based on two-sided t-test. (B) Comparison of neutralization of variants by convalescent serum (n=8, the same donors in A), BNT162b2 vaccinated individuals (n=9), mRNA-1273 vaccinated donors (n=8), Ad26.COV2.S vaccinated donors (n=10), sera from vaccinated individuals were collected at later time points. Each line shows individual donors. (C) Comparison of neutralization potency of each vaccine by different SARS-CoV-2 variants. The neutralization IC50 from individual donors vaccinated by BNT162b2 (yellow), mRNA-1273 (pink), Ad26.COV2.S (black) is shown. Significance is based on two-sided t-test.
Comparison of vaccines
Sera collected from individuals having received either of the mRNA vaccines was notably more effective two weeks post-administration against the D614G strain than convalescent sera, with a subsequent and modest 2.5-4.0-fold drop in antibody titer observed towards the SARS-CoV variants of concern in comparison with D614G.
Resistance towards antibodies observed in beta, delta, and lambda variants were attributed to E484K, L452R, and L452Q and F490S mutations, respective to the strain.
Upon further investigation, the group identified the L452R/Q mutation of the lambda variant as a key factor in reduced neutralizing antibody potency, seeing a two-fold increase in viral infectivity in immunized hosts and a three-fold increase in relative affinity towards the ACE2 receptor.
Alternatively, sera collected from individuals having received the adenovirus vector-based vaccine was seen to experience an even greater drop in efficacy against the variants of concern compared to the mRNA vaccines, around 5-7 fold against the delta plus or beta variants compared to D614G. REGN10933 and REGN10987 monoclonal antibodies were also exposed to the multiple SARS-CoV-2 lineages, showing reduced activity towards the beta and delta plus variants compared with D614G, attributed to K417N and E484K mutations.
This work has demonstrated that the SARS-CoV-2 variants of concern show a degree of resistance towards convalescent or vaccine-induced antibodies. However, that the mRNA vaccines, in particular, are still likely to generate a sufficient response against any lineage three months post-administration.
The adenovirus vector-based vaccine demonstrated a more notable loss in efficacy towards the newly emerging SARS-CoV-2 variants, being able to generate a less robust antibody response. However, the authors note that while other studies have observed a slight drop in the generated antibody response by the J&J vaccine against the latter variants, the results have not been as stark as reported here, which could be a factor of demographics or some other unaccounted influence.
In any case, constant genomic surveillance and testing of SARS-CoV-2 variants of concern will be required for the foreseeable future, potentially facilitating the development of vaccine boosters that maintain the efficacy of newly emerging variants that would otherwise escape established immunity.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Comparison of Neutralizing Antibody Titers Elicited by mRNA and Adenoviral Vector Vaccine against SARS-CoV-2 Variants Takuya Tada, Hao Zhou, Marie I. Samanovic, Belinda M. Dcosta, Amber Cornelius, Mark J. Mulligan, Nathaniel R. Landau, bioRxiv, 2021.07.19.452771; doi: https://doi.org/10.1101/2021.07.19.452771, https://www.biorxiv.org/content/10.1101/2021.07.19.452771v2
- Peer reviewed and published scientific report.
Tada, Takuya, Hao Zhou, Marie I. Samanovic, Belinda M. Dcosta, Amber Cornelius, Ramin S. Herati, Mark J. Mulligan, and Nathaniel R. Landau. 2022. “Neutralization of SARS-CoV-2 Variants by MRNA and Adenoviral Vector Vaccine-Elicited Antibodies.” Frontiers in Immunology 13 (March). https://doi.org/10.3389/fimmu.2022.797589. https://www.frontiersin.org/articles/10.3389/fimmu.2022.797589/full.