In 2020, the impact of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which is the causal agent of the coronavirus disease 2019 (COVID-19), on pregnant women was revealed by the World Health Organization (WHO). To this end, the WHO reported that COVID-19 infection during pregnancy posed a high risk of hospitalization. Furthermore, there is an increased possibility of preterm birth and admission for neonatal care for the newborn baby in these cases.
This conclusion by the WHO was the result of data obtained from prior studies conducted in the United States and China during the first six months of the pandemic. However, the impact of the SARS-CoV-2 variants on pregnant mothers and their unborn children has yet to be fully understood.
 Study: Impact of SARS-CoV-2 variant on the severity of maternal infection and perinatal outcomes: Data from the UK Obstetric Surveillance System national cohort. Image Credit: GolF2532 / Shutterstock.com
Study: Impact of SARS-CoV-2 variant on the severity of maternal infection and perinatal outcomes: Data from the UK Obstetric Surveillance System national cohort. Image Credit: GolF2532 / Shutterstock.com

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Pregnancy and COVID-19
In the United Kingdom, the SARS-CoV-2 Alpha variant, which was been deemed a variant of concern (VoC), was initially reported as the dominant variant in September 2020. By May 2021, the Delta SARS-CoV-2 variant dominated COVID-19 cases in the U.K.
Previous reports indicated that the Alpha strain possessed a high transmission rate and could cause severe infection to non-pregnant women, which increased hospital admissions. However, after the emergence of the Delta variant, researchers found that the risks of hospital admissions doubled within the general population when compared to the infection rate when the Alpha strain was the dominant circulating strain. However, there is limited data currently available on the impact of the SARS-CoV-2 variants on pregnant women and perinatal outcomes.
A recent study conducted in the U.K. revealed that the rate of hospital admissions of pregnant women was much higher during the second wave, during which the Alpha variant was the dominant strain, as compared to the first wave with the original SARS-CoV-2 strain. However, this study could not confirm if the risk of hospitalization increased with the emergence of new variants.
Another study conducted in India reported that during the second COVID-19 wave that was dominated by the Delta strain, there was a higher rate of intensive care unit (ICU) or high dependency unit admissions and deaths as compared to that which was recorded during the first wave. This report aligned with the results of another study conducted in Brazil.
Despite these findings, there remains a gap in data that accurately reveals the impact of SARS-CoV-2 variants on maternal and perinatal outcomes. This information is crucial to develop a robust strategy to protect this group from the severe effects of COVID-19.
SARS-CoV-2 VoCs and pregnant women
A new study published on the preprint server medRxiv* focuses on the impact of SARS-CoV-2 on maternal and perinatal outcomes. The present study included hospitalized pregnant women with confirmed SARS-CoV-2 infection and compared the severity of infection based on three dominant strains using multivariable logistic regressions. Notably, the study was conducted at three different time periods during which the wildtype, Alpha, and Delta variants were the dominant strain, respectively.
This study revealed that among 3,371 pregnant women, the majority of participants had experienced moderate to severe COVID-19. The severity of their symptoms significantly increased between the Wildtype and Alpha periods (first wave) and between the Alpha and Delta periods (second wave).
During the period when the Alpha strain was dominant, women were more likely to require respiratory support and show symptoms of pneumonia. The likelihood of women requiring respiratory support and experiencing severe pneumonia increased, even more, when the Delta strain was dominant. Although a reduced use of invasive ventilation was reported over time, there was increased use of high flow oxygen and continuous positive airway pressure (CPAP) over time.
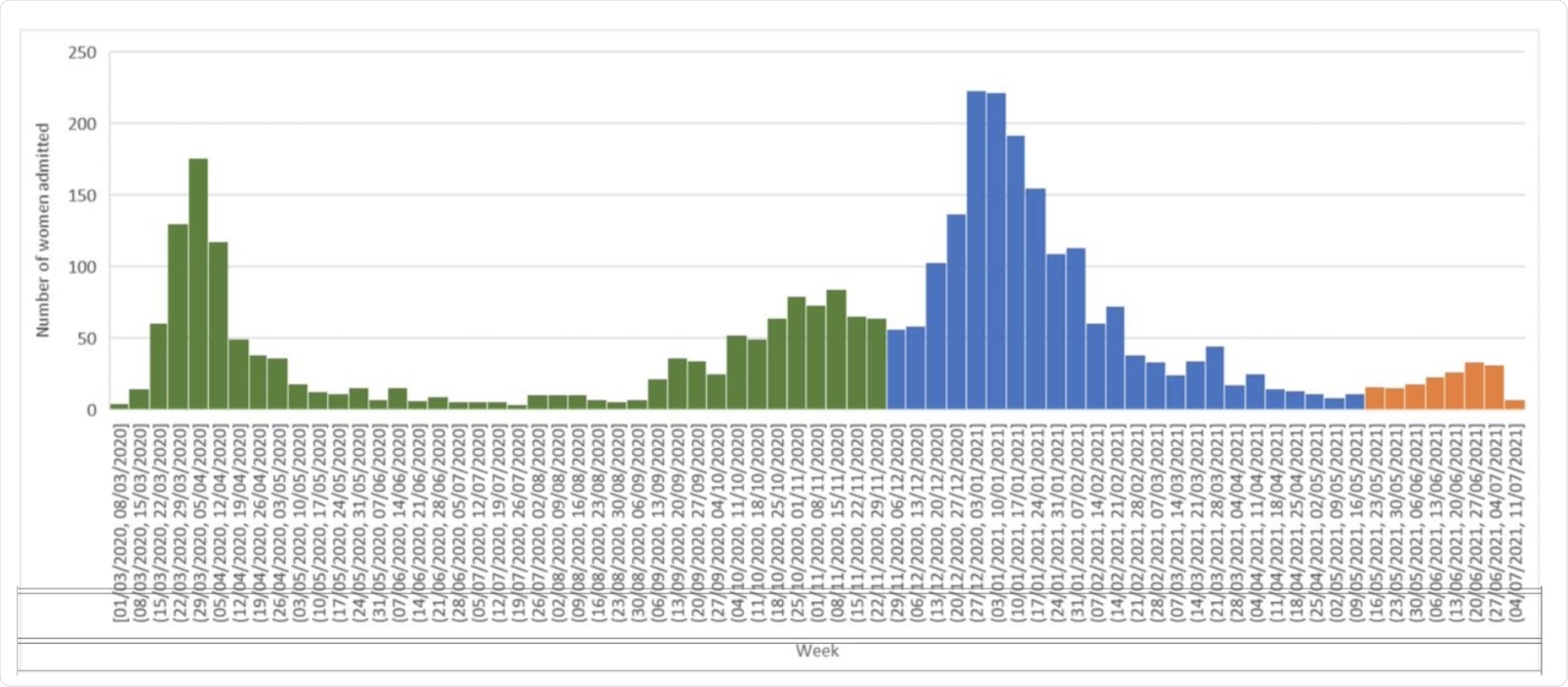 Admissions of pregnant women with symptomatic confirmed SARS-CoV-2 to UK hospitals during Wildtype (01/03/20-30/11/2 2020, Green), Alpha (01/12/20 – 15/05/21, Blue) and Delta periods (16/05/21-11/07/21, Orange)
Admissions of pregnant women with symptomatic confirmed SARS-CoV-2 to UK hospitals during Wildtype (01/03/20-30/11/2 2020, Green), Alpha (01/12/20 – 15/05/21, Blue) and Delta periods (16/05/21-11/07/21, Orange)
Impact of vaccines on pregnant women
The authors of the present study revealed that no fully vaccinated pregnant woman required hospitalization, even after the emergence of SARS-CoV-2 variants. Notably, vaccinated pregnant women who experienced breakthrough infections did not require extensive pharmacological intervention.
Strengths and limitations of the study
This is the first prospective cohort study that analyzed the impact of SARS-CoV-2 variants on pregnancy and perinatal outcomes. The strength of this study is the national case identification of all women admitted to the hospital due to severe COVID-19 infection.
One of the limitations of this study is the exclusion of pregnant women with mild symptoms who did not require hospital admission. Despite this limitation, it is highly likely that all women who were severely infected were hospitalized, which reduces any potential bias. Another limitation of this study is that variant sequencing data was not included, and the time period was instead used as a proxy.
Conclusion
The current study showed that pregnant women who were completely vaccinated were not severely affected by both SARS-CoV-2 wildtype and VoCs. Despite the high effectiveness associated with the COVID-19 vaccines, the researchers observed a reluctance in this patient population to take vaccines. As a result, there remains an urgent need to tackle misinformation and encourage pregnant women to get vaccinated, particularly when considering the risks associated with the Delta variant.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Vousden, N., Ramakrishnan, R., Bunch, K., et al. (2021). Impact of SARS-CoV-2 variant on the severity of maternal infection and perinatal outcomes: Data from the UK Obstetric Surveillance System national cohort. medRxiv. doi:10.1101/2021.07.22.21261000. https://www.medrxiv.org/content/10.1101/2021.07.22.21261000v1.
- Peer reviewed and published scientific report.
Vousden, Nicola, Rema Ramakrishnan, Kathryn Bunch, Eddie Morris, Nigel A B Simpson, Christopher Gale, Patrick O’Brien, et al. 2022. “Severity of Maternal Infection and Perinatal Outcomes during Periods of SARS-CoV-2 Wildtype, Alpha, and Delta Variant Dominance in the UK: Prospective Cohort Study.” BMJ Medicine 1 (1): e000053. https://doi.org/10.1136/bmjmed-2021-000053. https://bmjmedicine.bmj.com/content/1/1/e000053.