
 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Significance of post-COVID mental health morbidities
Several international studies have been conducted on COVID-19 patients to identify the prevalence of adverse mental health symptoms. To this end, previous meta-analyses have revealed high anxiety and depression symptoms in COVID-19 patients within six months post-hospitalization. However, more recent studies on non-hospitalized COVID-19 patients have provided limited information on long-lasting mental morbidities with varying illness severities.
About the study
The present multinational study was conducted in Sweden, Norway, Scotland, Estonia, Denmark, and Iceland from April 2020 to August 2021 to determine the development of adverse mental health outcomes among the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)-infected general population based on acute infection severity up to 16 months post-diagnosis.
Among a total of 299,334 participants from the seven cohorts, 247,249 individuals were included in the study after the exclusion of subjects with incomplete data on COVID-19 diagnosis, disease severity, analytical cohort, and mental health symptoms outcome measures.
The time-related contrast in the prevalence of anxiety, COVID-19-related distress, poor sleep quality, and depression symptoms among COVID-19 patients and those not infected with SARS-CoV-2 from the time of entry and illness severity were measured using a cross-sectional analysis and multivariable Poisson regression model. Among individuals who were diagnosed with COVID-19, the differences in repeated measures of mental health symptoms before and after the COVID-19 diagnosis were tested using the generalized estimating equations (GEE) analysis.
The diagnosis of COVID-19 was based on self-reports of confirmed positive antibody test or polymerase chain reaction (PCR) test. The time from diagnosis to data collection was coded into 0-2; 2-6; 6-16-month categories.
The acute infection severity of COVID-19 was determined using self-reports of the number of COVID-19-associated bedridden days, the number of days with fever, and data on COVID-19 associated hospitalization.
Study findings
The results show that during the study period, 4%, which amounts to a total of 9,979 participants of the population were diagnosed with COVID-19. Of these individuals, the proportion of females was higher and the mean age of the participants was between 40-50 years, with the exception of Norway cohorts that had a mean age of mid-30s.
Participants with a history of COVID-19 had an overall high level of poor sleep quality and depression symptoms in the first 16 months post-COVID as compared to the distress and anxiety symptoms in those without a history of COVID-19. However, the prevalence of COVID-19-related distress and depression attenuated with time. According to the severity of COVID-19, the trajectories of adverse mental morbidities post-COVID varied significantly throughout the 16 months duration.
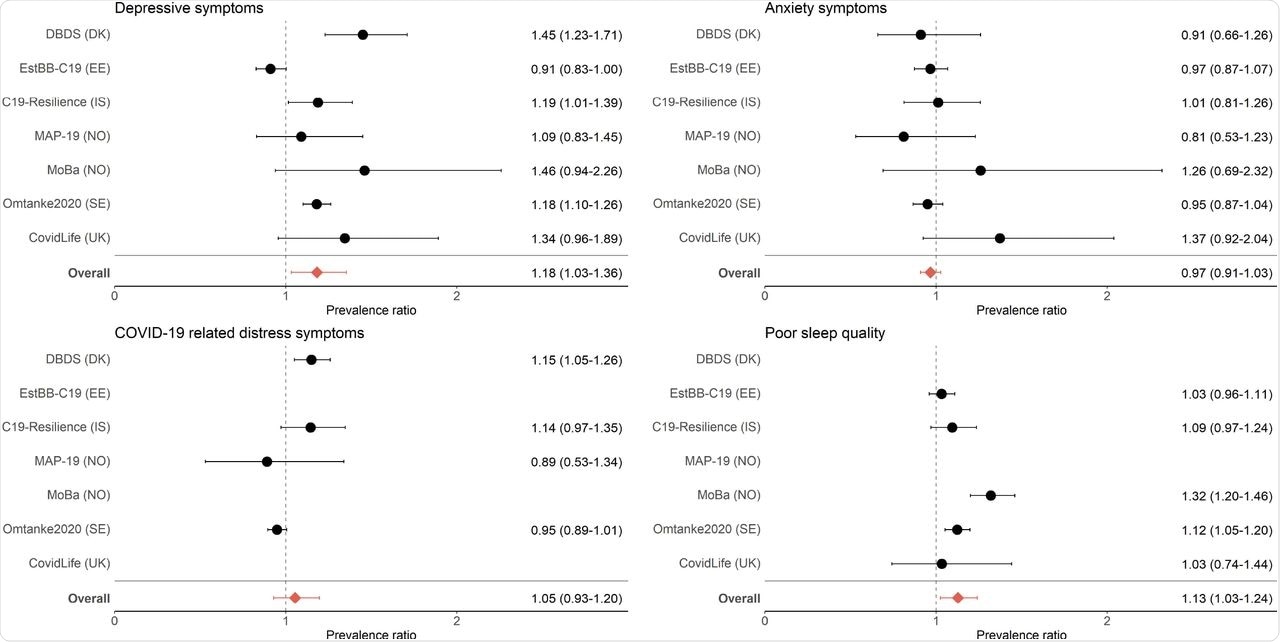 Prevalence ratios (with 95% confidence intervals) of mental health indicators among individuals with a diagnosis of COVID-19 compared with individuals without a COVID-19 diagnosis.
Prevalence ratios (with 95% confidence intervals) of mental health indicators among individuals with a diagnosis of COVID-19 compared with individuals without a COVID-19 diagnosis.
Throughout the 16-month study period, COVID-19 patients who were bedridden for more than seven days had a 50-60% increased risk of post-COVID anxiety and depression as compared to those who were not bedridden due to COVID-19. In patients diagnosed with COVID-19, 21% had depressive symptoms above the cut-off value at least six months post-diagnosis, whereas 44% of patients who were hospitalized with COVID-19 reported depressive symptoms between 6-16 months post-diagnosis.
The cohorts with an increased number of COVID-positive patients also had an increased history of psychiatric disorders. The prevalence of post-COVID mental health symptoms among the confirmed COVID-19 cases was similar in four of the six countries studied.
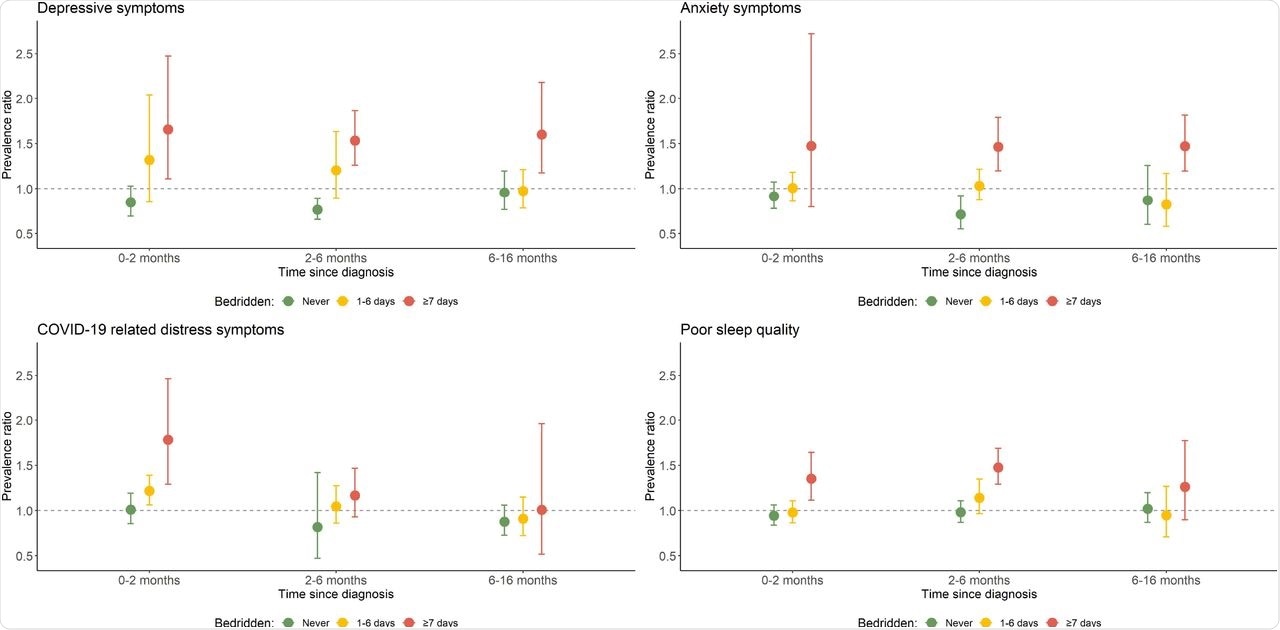 Mental health indicators during the first 16 months after diagnosis of COVID-19 by time bedridden.
Mental health indicators during the first 16 months after diagnosis of COVID-19 by time bedridden.
Conclusions
The current multinational study found that the mental morbidities up to 16 months after recovering from COVID-19 can be primarily determined based on the acute infection severity.
Those who had severe COVID-19 infection were bedridden for more than seven days as compared to those with mild disease. The extended bedridden time in COVID-19 patients was associated with an elevated risk of mental health symptoms, whereas COVID-19 patients who were never bedridden had a reduced risk of post-COVID mental health symptoms throughout the 16 months post-diagnosis. According to the authors, this association of extended bedridden time and adverse mental health symptoms was first identified in this study.
The study findings correlate with the limited information from previous studies on the adverse mental health status of individuals after recovering from COVID-19. The prevalence of post-COVID-19 mental health symptoms was almost similar among all the cohorts studied, thereby indicating the absence of any systematic bias in the present study. The observations in this study highlight the need for continued clinical monitoring beyond the initial year in those experiencing severe post-COVID-19 symptoms.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Magnusdottir, I., Lovik, A., Unnarsdottir, A. B., et al. (2021). Acute COVID-19 severity and 16-month mental morbidity trajectories in patient populations of six nations. medRxiv. doi:10.1101/2021.12.13.21267368. https://www.medrxiv.org/content/10.1101/2021.12.13.21267368v1
- Peer reviewed and published scientific report.
Magnúsdóttir, Ingibjörg, Anikó Lovik, Anna Bára Unnarsdóttir, Daniel McCartney, Helga Ask, Kadri Kõiv, Lea Arregui Nordahl Christoffersen, et al. 2022. “Acute COVID-19 Severity and Mental Health Morbidity Trajectories in Patient Populations of Six Nations: An Observational Study.” The Lancet Public Health 0 (0). https://doi.org/10.1016/S2468-2667(22)00042-1. https://www.thelancet.com/journals/lanpub/article/PIIS2468-2667(22)00042-1/fulltext.