
 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Background
Nosocomial SARS-CoV-2 infections from long-term care facilities (LTCFs) and other geriatric institutions constitute a substantial fraction of COVID-19 cases and SARS-CoV-2-associated mortality and morbidity all over the world. Healthcare-associated SARS-CoV-2 infection might have a significant role in augmenting the COVID-19 pandemic.
The identification of the source and transmission chains of SARS-CoV-2 infection enhances infection prevention and control (IPC) strategies. However, sufficient data regarding the SARS-CoV-2 transmission chain among HCWs and elderly patients, as well as their respective roles in the nosocomial outbreaks, are not available yet.
About the study
In the present retrospective cohort study, the researchers analyzed the transmission dynamics of several nosocomial outbreaks of COVID-19 comprising HCWs and elderly patients in the Hospital of Geriatrics, which is part of the Geneva University Hospitals (HUG). This hospital was largely responsible for treating non-COVID-19 and COVID-19 patients during the first wave of the COVID-19 pandemic.
The data were prospectively collected from the Swiss Federal Office of Public Health-mandated surveillance of hospitalized COVID-19 patients, HUG’s Department of Occupational Health for symptom-onset data, and Department of Human Resources (HR) for HCW shifts.
The study included all SARS-CoV-2 reverse transcription-polymerase chain reaction (RT-PCR)-positive HCWs and nosocomial COVID-19 patients of four outbreak-affected wards from March 1, 2020, to May 7, 2020.
Patients with hospital-acquired and community-acquired COVID-19 were denoted as “patientnoso” and “patientcommunity,” respectively. HCWs working in COVID-19 wards admitting community-acquired infections and non-COVID wards where nosocomial outbreaks occurred are referred to as “HCWcovid” and “HCWoutbreak,” respectively.
SARS-CoV-2 whole-genome sequencing (WGS) was performed using an amplicon-based sequencing method. Further, SARS-CoV-2 genome sequences were aligned and phylogenetically analyzed using the MUSCLE (v3.8.31) software and the Maximum Likelihood method and Tamura 3-parameter model, respectively. The transmission trees among HCWs and patients were reconstructed using the Bayesian framework.
Study findings
A total of 180 SARS-CoV-2 positive cases, of which included 91 HCWcovid, 36 HCWoutbreak, and 53 patients, from the four outbreak wards, were included in the study. According to the post hoc analysis, four of the 53 positive patients were likely to be community-acquired COVID-19 cases.
The ward level SARS-CoV-2 transmission rate was 10-19% and 21% for patients and HCWs, respectively. A total of 16 importation events from three patients and 13 HCWs were estimated, which led to 16 secondary cases of COVID-19.
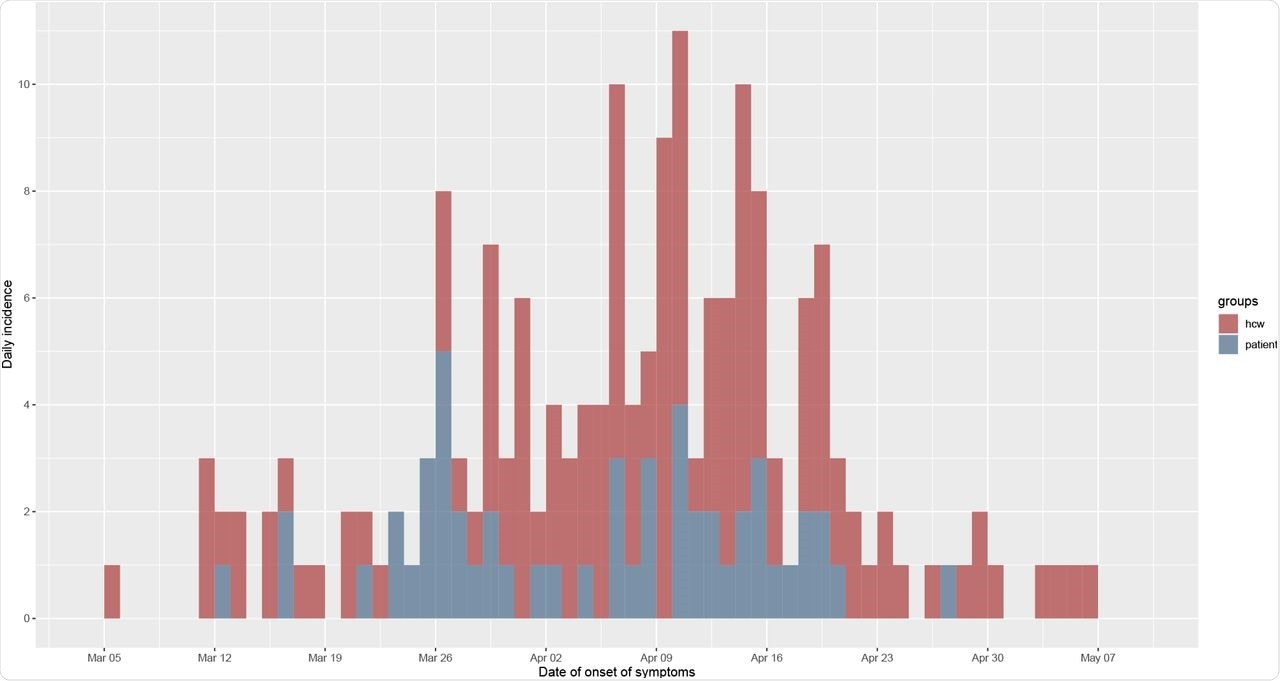
Epidemic curve of the nosocomial COVID-19 outbreak in a geriatric hospital involving HCWs and patients.
Patient-to-patient transmission among patients who shared a ward was 97.6%, whereas patient-to-patient transmission among those sharing a room was 44.4%.
Patientnoso were two times more likely to infect other patientnoso than expected, with an observed to expected ratio and 95% CrI of 1.91 and 1.08-4.00, respectively. Further, HCWoutbreak was two times more likely to infect other HCWoutbreak than expected, with an observed to expected ratio and 95% CrI of 2.25 and 1.00-8.00, respectively.
The HCWcovid proportion of infectors was as expected during the early and late phases of the outbreak. The HCWoutbreak and patientnoso groups had 26.2% and 13.4% of transmitters, respectively, during the late phases of the outbreak.
Conclusions
The present study provides valuable insights into the transmission dynamics of nosocomial SARS-CoV-2 infections among HCWs and elderly populations in a geriatric acute care hospital setting. According to the authors, this is the first study to extensively investigate the COVID-19 outbreak using WGS and sophisticated modeling at a geriatric hospital.
The sophisticated modeling of combined epidemiological and genetic data employed in the study demonstrated the overall SARS-CoV-2 transmission patterns. The transmission dynamics among the HCWcovid and HCWoutbreak indicated a two times higher risk of HCW-to-HCW transmission in the HCWoutbreak group as compared to the HCWcovid group.
Patients within the same ward had a higher incidence of patient-to-patient transmission than those in the same room. Several importation events that led to a substantial increase in secondary cases or clusters were identified primarily in HCWs. The WGS coverage of the study was very high, as 80% of the cases involved provided sequencing data.
Overall, the current study underscores the possible gaps and areas for improvement in IPC strategies, which can potentially limit the extent of hospital-acquired SARS-CoV-2 infection transmission.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Abbas, M., Cori, A., Cordey, S., et al. (2022). Reconstructing transmission chains of SARS-CoV-2 amid multiple outbreaks in a geriatric acute-care hospital. medRxiv. doi:10.1101/2022.01.07.22268729. https://www.medrxiv.org/content/10.1101/2022.01.07.22268729v1.
- Peer reviewed and published scientific report.
Abbas, Mohamed, Anne Cori, Samuel Cordey, Florian Laubscher, Tomás Robalo Nunes, Ashleigh Myall, Julien Salamun, et al. 2022. “Reconstruction of Transmission Chains of SARS-CoV-2 amidst Multiple Outbreaks in a Geriatric Acute-Care Hospital: A Combined Retrospective Epidemiological and Genomic Study.” Edited by Joshua T Schiffer, Wendy S Garrett, Lulla Opatowski, and Thi Pham. ELife 11 (July): e76854. https://doi.org/10.7554/eLife.76854. https://elifesciences.org/articles/76854.