The coronavirus disease 2019 (COVID-19) pandemic, which is caused by infection with the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), brought caused over 5.73 million deaths as of February 7, 2022. Some of the common symptoms associated with COVID-19 include headache, cough, myalgia, dyspnea, diarrhea, and arthralgia. More recently, a new symptom has been associated with COVID-19 that leads to taste or smell disorders (TSD) in infected patients.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
The relationships between immune response intensity, TSD, and their association with other COVID-19 symptoms remain unclear. Although long-term data remains scarce, TSD has been reported to be persistent in some patients over time.
In a new study published on the preprint server medRxiv,* researchers conduct an analysis based on the data from the “Santé, Perception, pratiques Relations et Inégalités Sociales en population générale pendant la crise COVID-19” (SAPRIS) multi cohort study. The goal of the study was to identify subject characteristics with TSD, investigate the relationship between TSD and immune response intensity, and characterize symptom associations for patients with or without TSD.
About the study
Three general population-based cohorts were included in the current study. The first was a general adult population-based cohort that represented 215,000 adults between the ages of 18 to 69 years and was recruited from 2012.
The second study cohort was referred to as E3N / E4N, which was a multigenerational adult cohort with 113,000 participants, of which 90,000 were called for an internet follow-up. The third group included NutriNet-Santé, which was a nutritional general population-based cohort that began in 2009 and included 170,000 participants.
All study participants had to respond to two electronic self-administered questionnaires that were sent on April 1, 2020, and had to be returned before May 27, 2020. The participants also provided self-sampling dried-blood spot (DBS) for serology testing to identify patients who were infected with SARS-CoV-2.
The symptoms included in this study were present at least once within 14 days before each questionnaire was reported. Additionally, data on alcohol consumption, smoking status, and body mass index (BMI) were also extracted and considered as binary variables.
The enzyme-linked immunosorbent assay (ELISA) was used to detect anti-SARS-CoV-2 antibodies (IgG) against the S1 domain of the spike (S) protein, along with the nucleocapsid protein (NP) in some cases. The optical density ratios of ELISA-S, ELISA-NP, and neutralizing anti-SARS-CoV-2 antibody titers were considered as quantitative variables.
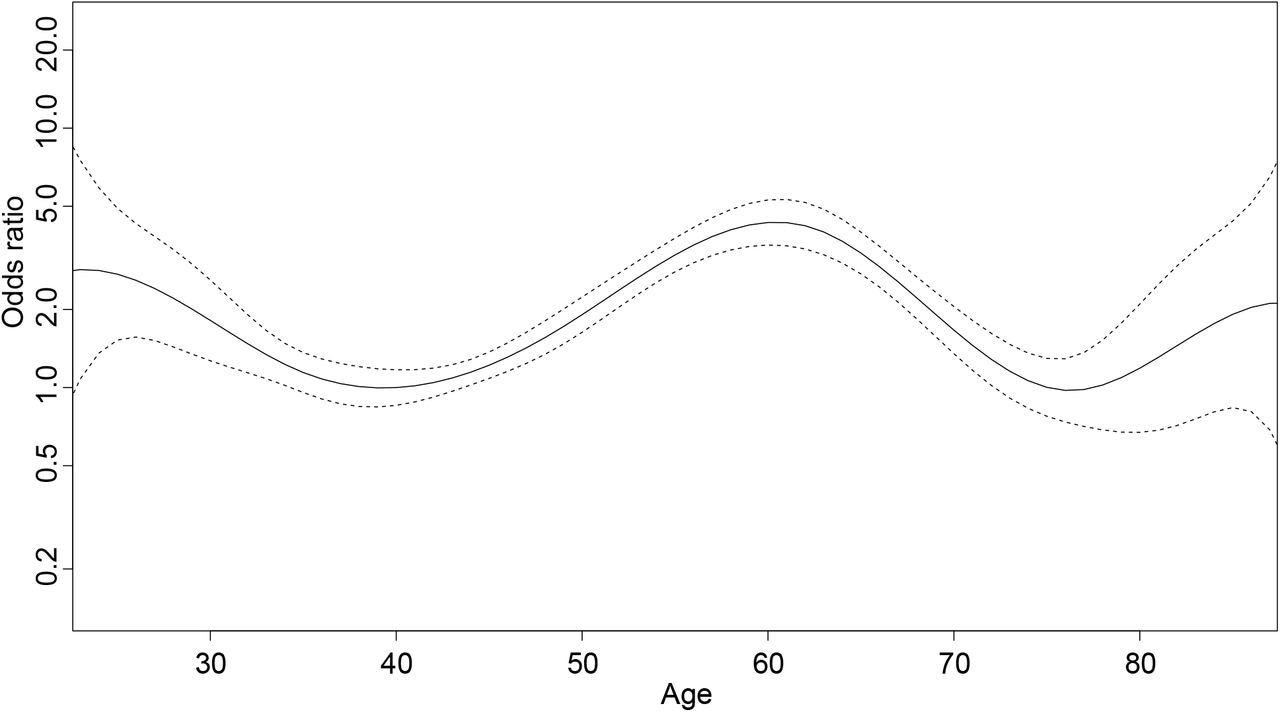
Age-dependent estimated OR (and 95% CI) of taste or smell disorder, people aged 40 as reference Graphic representation of age-dependent estimated OR (and 95% CI) of taste and smell disorders in multivariable analyses. People aged 40 are considered as reference.
Study findings
Out of the 93,610 participants who completed both questionnaires and were invited to perform a DBS, 3,439 were included in the study. Out of the recruited participants, 750 were reported TSD. Whereas 71.2% of women with a median age of 51 reported TSD, 68.7% with a median age of 46 did not report this symptom.
Smoking status, alcohol consumption of at least two drinks a day, and the female sex were associated with a higher probability of TSD. Participants aged 30, 50, 60, or 70 showed a higher probability of TSD as compared to those aged 40.
All serological titers were associated with a higher probability of TSD. Furthermore, in 90% of study participants, TSD was associated with a wide variety of symptoms, while for 10% of the participants, TSD was an isolated symptom or associated with rhinorrhea.
The current study indicates that the chances of developing TSD were higher in women, smokers, and people who drink more than two drinks a day. TSD was also found to induce a strong humoral response, with most cases of TSD associated with a wide variety of symptoms.
Limitations
Only a positive ELISA test was considered to indicate SARS-CoV-2 infection. An additional limitation was that humoral immunity that developed in the weeks following infection can decrease with time and may not be detectable in 10% to 20% of individuals. Finally, self-reporting of symptoms can introduce bias.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Ramillon, J., de Lamballerie, X., Robineau, O., et al. (2022). Humoral response, associated symptoms and profile of patients infected by SARS-CoV-2 with taste or smell disorders in the SAPRIS multicohort study. medRxiv. doi:10.1101/2022.02.01.22270250. https://www.medrxiv.org/content/10.1101/2022.02.01.22270250v1.
- Peer reviewed and published scientific report.
Ramillon, Julien, Xavier de Lamballerie, Olivier Robineau, Hélène Blanché, Gianluca Severi, Mathilde Touvier, Marie Zins, et al. 2023. “Antibody Response, Associated Symptoms and Profile of Patients Presumably Infected by SARS-CoV-2 with Taste or Smell Disorders in the SAPRIS Multicohort Study.” BMC Infectious Diseases 23 (1). https://doi.org/10.1186/s12879-023-08162-7. https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-023-08162-7.