Before the worldwide vaccination campaigns began in 2021, mRNA-based severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) vaccines, including BNT162b2 and mRNA-1273, were tested for efficacy and safety in large randomized trials. The trial studies established excellent safety profiles for the mRNA-based COVID-19 vaccines, following which they earned emergency use authorization (EUA). In the trials, however, rare side effects of vaccination were not reliably detected.
Consequently, there were reports of several new-onset and periodically repeated cases of glomerulonephritis among the SARS-CoV-2 vaccine recipients. The most common types of glomerulonephritis post-SARS-CoV-2 vaccination included minimal change disease (MCD), and Berger’s disease, wherein the kidney accumulates immunoglobulin A (IgA), also called IgA nephropathy (IgAN). Additionally, there were cases of membranous nephropathy (MN) and pauci-immune necrotizing glomerulonephritis (PINGN).
Due to insufficient evidence for a temporal link between SARS-CoV-2 vaccination and glomerulonephritis, the null hypothesis assumes that cases occurring in proximity to COVID-19 vaccination are simply coincidental.
About the study
In the present study, researchers directly compared the glomerulonephritis cases in Switzerland during 2021 to the number of expected cases based on the disease incidence rates between 2015 and 2019. As they matched cases of new-onset glomerulonephritis diagnosed during the COVID-19 vaccination campaign with the general population matched for age and time point, they were able to characterize patients suffering from the disease in temporal association with SARS-CoV-2 vaccination.
The team conducted two complementary studies. The first study cohort included patients aged 18 years or more with confirmed histological diagnoses of IgAN, PINGN, MCD, or MN between January 1, 2015, and August 31, 2021. Switzerland’s pathology institutes provided biopsy date, age, and gender information of all the patients participating in the study. Further, the researchers used Swiss census data for each year from 2015 to 2021 to calculate the incidence of all four types of glomerulonephritis.
They obtained information on the second study participants from the nephropathologists who had provided biopsy specimens of the eligible patients with age, sex, histological diagnosis, and the biopsy date. The study investigators reviewed each patient’s clinical and epidemiological data, a case report form (CRF) completed by the nephrologist treating the patient, and a questionnaire self-completed by the patient. The researchers chose 1,000 controls per patient from the general Swiss population. They used Kruskal-Wallis’ test and Pearson’s X2 test, as appropriate, for comparisons between the study groups.
For comparisons, the team used risk ratios computed by unconditional maximum likelihood estimation, based on the assumption that data on the total number of vaccinated and unvaccinated individuals in Switzerland were available. The researchers downloaded data on the types and number of vaccine doses by age and calendar week from the Swiss Federal Office of Public Health.
Further, the researchers used a Bayesian Poisson regression model to predict the expected incidence of glomerulonephritis cases for each month in 2021. The team presented case incidence as the number of biopsy-proven glomerulonephritis cases per million population. Further, they calculated incidence rate ratios for all four types of glomerulonephritis and each diagnosis separately by dividing the observed cases in 2021 by the expected cases.
Study findings
This study looked for incidences of glomerulonephritis among 7.1 million individuals, of which 69% had received at least one dose of an mRNA-based SARS-CoV-2 vaccine during the study period. The authors could not find evidence that vaccination increased the risk for new-onset glomerulonephritis. Therefore, all such cases were likely attributable to temporal coincidence. Moreover, the incidence of all four types of glomerulonephritis did not surpass the expected rate during the COVID-19 vaccination campaign.
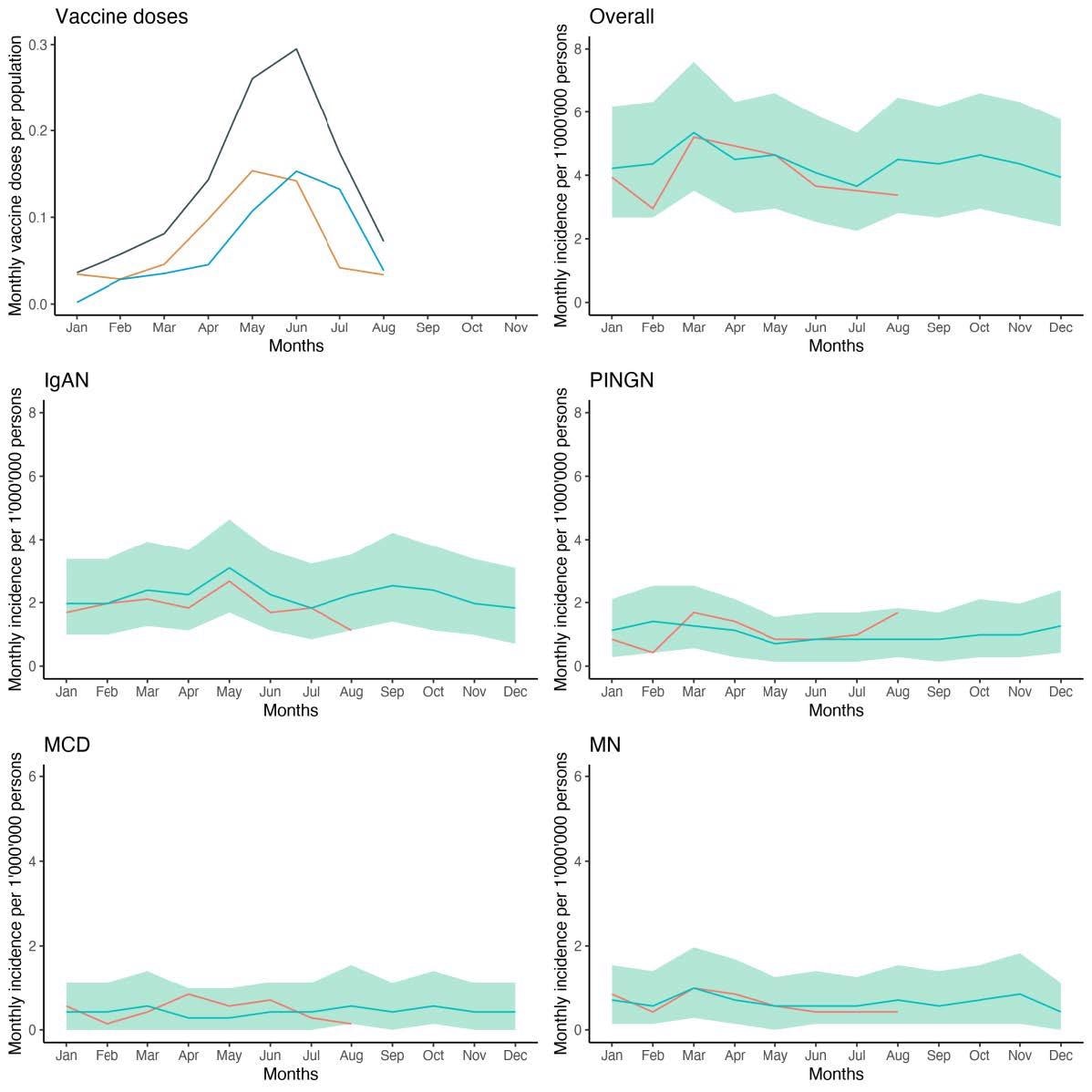
Expected and observed incidence of glomerulonephritis during the vaccination campaign. Shown is the number of first (orange), second (blue) and total (grey) doses of SARS-CoV-2 vaccines as a fraction of all patients aged ≥ 20 years (upper left panel) and the observed incidence of glomerulonephritis in patients aged ≥ 18 years from January to August 2021 (red line) compared to the expected incidence based on the years 2015 to 2019 (blue line) with 95% credible intervals (green shading) for the sum of all four glomerulonephritides, and by diagnosis.
The characteristics of patients with glomerulonephritis temporally related to vaccination did not differ from those with no temporal association to vaccination. In Switzerland, the only exception was old age, as older people were preferentially vaccinated during SARS-CoV-2 vaccination campaigns.
There was a slightly higher risk of the development of MCD due to SARS-CoV-2 mRNA vaccines; however, the absolute risk was relatively small. Likewise, the authors also did not observe any increase in the rates of patient-reported gross hematuria in patients with newly diagnosed IgAN in temporal association to vaccination.
Conclusions
Glomerulonephritis is a rare disease, so the researchers found its baseline incidence rates for other European countries. Interestingly, its incidence rate had fallen drastically during the lockdown imposed during the first COVID-19 pandemic wave, primarily attributed to IgAN, the most frequent of the four glomerulonephritides. This finding demonstrated the feasibility of the present study in identifying actual incidence rates of glomerulonephritis cases.
The study highlighted that the estimated risk for developing new-onset glomerulonephritis was equal in vaccinated vs. unvaccinated persons in Switzerland. Temporal analysis revealed that the number of patients who received a vaccine vs. those who did not were identical four weeks before the diagnosis of glomerulonephritis in both the study cohorts. Moreover, the findings were consistent for all four types of glomerulonephritis. The sensitivity analysis excluding all MN cases fetched similar results.
Overall, SARS-CoV-2 vaccination did not increase the incidence of any of the four types of common glomerulonephritis, including IgAN, PINGN, MCD, and MN.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Incidence of Glomerulonephritis after SARS-CoV-2 mRNA Vaccination, Matthias Diebold, Eleonore Locher, Philipp Boide, Anette Enzler-Tschudy, Anna Faivre, Ingeborg Fischer, Birgit Helmchen, Helmut Hopfer, Min Jeong Kim, Solange Moll, Giliane Nanchen, Samuel Rotman, Charalampos Saganas, Harald Seeger, Andreas David Kistler, medRxiv pre-print 2022, DOI: https://doi.org/10.1101/2022.05.18.22275112, https://www.medrxiv.org/content/10.1101/2022.05.18.22275112v1
- Peer reviewed and published scientific report.
Diebold, Matthias, Eleonore Locher, Philipp Boide, Annette Enzler-Tschudy, Anna Faivre, Ingeborg Fischer, Birgit Helmchen, et al. 2022. “Incidence of New Onset Glomerulonephritis after SARS-CoV-2 MRNA Vaccination Is Not Increased.” Kidney International 102 (6): 1409–19. https://doi.org/10.1016/j.kint.2022.08.021. https://www.kidney-international.org/article/S0085-2538(22)00697-4/fulltext.