To this end, they analyzed a nationwide, longitudinal cohort of 142758 blood donors who donated blood two to three times in 2020. The Centers for Disease Prevention and Control (CDC) established this cohort in association with Red Cross, Vitalent, Creative Testing Solutions, and Westat.
 Study: Estimates of SARS-CoV-2 Seroprevalence and Incidence of Primary SARS-CoV-2 Infections Among Blood Donors, by COVID-19 Vaccination Status — United States, April 2021–September 2022. Image Credit: next143 / Shutterstock
Study: Estimates of SARS-CoV-2 Seroprevalence and Incidence of Primary SARS-CoV-2 Infections Among Blood Donors, by COVID-19 Vaccination Status — United States, April 2021–September 2022. Image Credit: next143 / Shutterstock
Background
From the beginning of the COVID-19 pandemic to the end of 2022, changes in COVID-19 testing behaviors and test result reporting requirements have hindered authorities from estimating the U.S. SARS-CoV-2 primary infection burden. However, this data has public health implications; for instance, it could help identify population subsets at higher risk of infection and devise targeted strategies to mitigate the risk.
About the study
In the present study, researchers randomly selected one sample per blood donor from the CDC cohort to test for antibodies against the SARS-CoV-2 spike (S) and nucleocapsid (N) antigens in the first three quarters of 2022 and one quarter of 2021, i.e., April to June 2021. They also ascertained whether the donor had received a COVID-19 vaccine at each blood donation visit.
Further, the team weighted the sample data for selection into cohort accounting for two factors, as follows:
i) response during the four quarters;
ii) demographic variations between the blood donor and the general U.S. population.
Based on each study participant's antibody testing results and COVID-19 vaccination history, researchers estimated their vaccine-, infection-induced, or hybrid immunity. In addition, they estimated the number of individuals whose immune status changed between two quarters. This criterion limited this analysis to 72,748 blood donors, i.e., 51% of cohort strength. An iterative weighting adjustment method, thus, helped obtain weights via stratification and raking combined.
Furthermore, the team estimated the seroconversion of anti-N–negative individuals to anti-N–positive individuals across all four quarters included in this study. They stratified estimates by race/ethnicity and four age bands, 16 to 29, 30 to 49, 50 to 64, and ≥65 years. The cohort comprised people primarily from four ethnicities, viz., Asian, Black, Hispanic, and others.
Finally, the team presented seroprevalence and infection rates as weighted means and compared these results using two-sided t-tests. They stratified comparison results by demographics and vaccination status, where a significance level for α was equal to 0.05.
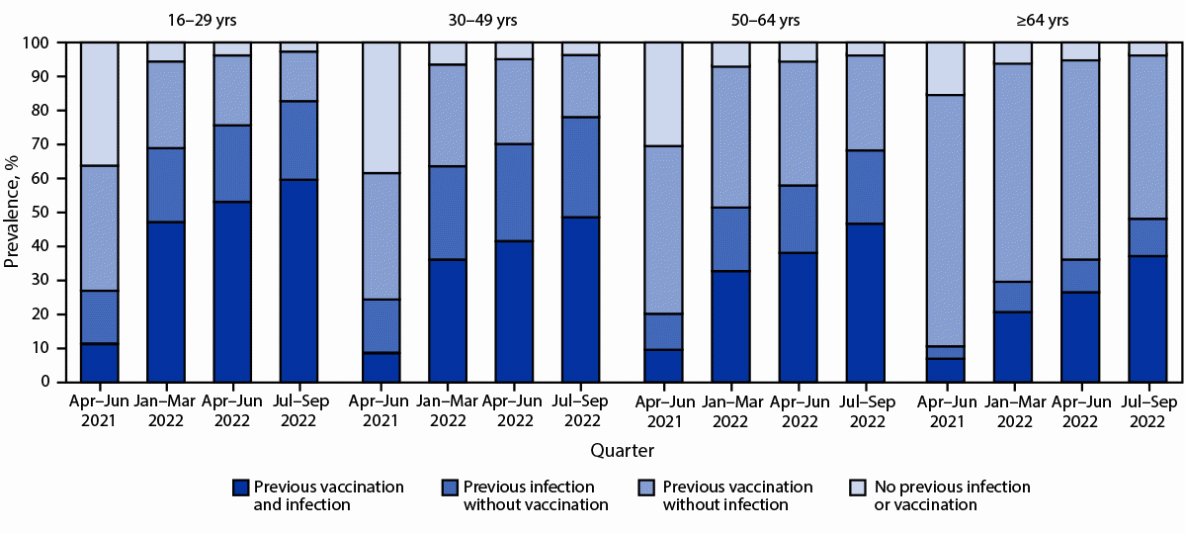
Prevalences of vaccine-induced, infection-induced, and hybrid* immunity† against SARS-CoV-2 among blood donors aged ≥16 years, by age group — United States, April 2021–September 2022
Results
In this study cohort, an estimated 96.4% of individuals aged 16 years or more had previous infection- or vaccination-induced SARS-CoV-2 antibodies, of which 47.7% had hybrid immunity by the end of September 2022 third quarter; 22.6% of individuals had developed immunity by natural infection and 26.1% from vaccination.
N antibody seroconversion indicates natural SAR-CoV-2 infection; in this study, it was higher in unvaccinated persons relative to vaccinated people, showing that vaccination provided some protection against SARS-CoV-2 infection. It could also be because vaccinated and unvaccinated individuals have different prevention behaviors, including face masking and social distancing.
During the period of dominance of the SARS-CoV-2 Omicron variant, the relative difference in infection rates narrowed down, most likely because vaccine-induced protection wanes more rapidly as time elapsed post-vaccination increases. Also, Omicron evades all elicited immunity to cause breakthrough infections. However, by late 2022, the difference in infection rates also narrowed down between vaccinated and unvaccinated persons because both adopted nearly similar prevention behaviors.
Likewise, the incidence of index SARS-CoV-2 infection(s) was higher among younger vs. older persons and lower among Asian vs. other races and ethnicities; however, these differences among all evaluated groups also narrowed down with time. Intriguingly, the prevalence of hybrid immunity was the highest among Black and Hispanic populations vs. Asians and White people.
Conclusions
In this report, researchers detected that nearly 50% of people aged ≥16 years with immunity had hybrid immunity, and two-thirds contracted a natural infection. Both infection-induced and hybrid immunity increased during the study duration, but the prevalence of hybrid immunity remained low among adults aged 65 years or older. These results showed the positive, beneficial effects of more vaccination coverage and immediate availability of COVID-19 vaccines for the elderly population in the US and worldwide.
Moreover, the older adults, i.e., people aged 65 years or more, adhered to recommended behavioral practices to avoid SARS-CoV-2 infection more than the other three age groups monitored in this study. Nonetheless, as suggested by the present study results, for people at high risk of severe SARS-CoV-2 infection, even others, it is crucial to remain updated with recommended COVID-19 vaccination, including at least one bivalent dose.