Negative pressure rooms, also called isolation rooms, are a type of hospital room that keeps patients with infectious illnesses, or patients who are susceptible to infections from others, away from other patients, visitors, and healthcare staff.
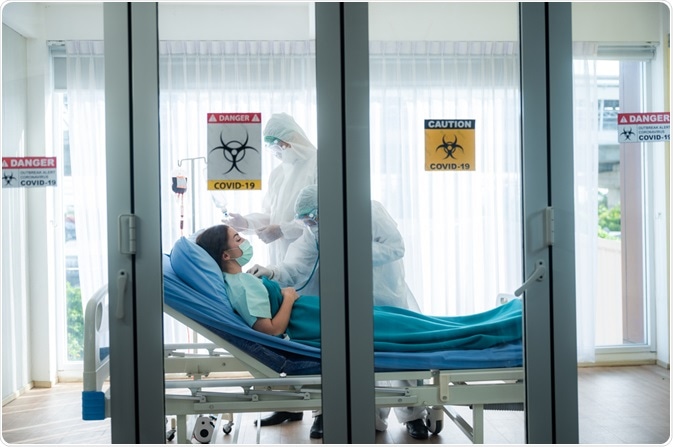
Image Credit: Chokniti Khongchum/Shutterstock.com
They are a common method of infection control and are used to isolate patients with contagious, airborne diseases such as measles, tuberculosis, SARS, MERS, and COVID-19.
How do negative pressure rooms ork?
They are called negative pressure rooms because the air pressure inside the room is lower than the air pressure outside the room. This means that when the door is opened, potentially contaminated air or other dangerous particles from inside the room will not flow outside into non-contaminated areas.
Instead, non-contaminated filtered air will flow into the negative pressure room. Contaminated air is sucked out of the room with exhaust systems, which are built with filters that clean the air before it is pumped outside of and away from the healthcare facility.
There are several ways that airflow within a room can be controlled.
These methods include:
- Controlling the quantity and quality of the air being put into and out of a room
- Controlling the air pressure between adjacent rooms or areas
- Designing specific airflow patterns for certain clinical situations or procedures
- Diluting infectious air or particles with large amounts of clean air
- Filtering the air with HEPA filters, among other types.
Some negative pressure rooms require an anteroom, which is an airlock room that provides a safe area for healthcare professionals to change into or out of protective clothing, transfer or prepare equipment and supplies, and can protect other rooms from contamination if pressure is lost within the negative pressure room.
The temperature and humidity in a negative pressure room must be monitored as the increased amount of air exchange within the room can create draughts that may be uncomfortable for a patient.
Negative pressure rooms do not have to be individual rooms for a single patient at a time. Common negative pressure environments in hospitals can include waiting areas, bathrooms, and triage areas, where infections can easily be spread.
The Different Types of Isolation Rooms
There are four types of isolation rooms, two of which are negative pressure rooms.
Class S
Class S isolation rooms are neutral or standard air pressure rooms, in which normal air conditioning is used. They are used for contact isolation, which is a type of infection control requiring the use of gloves, gowns, and masks to ensure no one comes into direct contact with a patient with an infectious illness. Class S rooms can be used for other means when not in use for patients needing isolation.
Class P
Class P rooms are positive pressure rooms. Patients who are immunocompromised are protected from becoming infected by potentially dangerous particles from other patients, visitors, or healthcare staff.
Class N
Class N rooms are negative pressure rooms in which people outside of the room are protected from any infectious airborne particles inside the room. Class N rooms should be at the front of an inpatient unit so any patients going into the room do not pass by other patients in different areas of the unit.
Class N rooms are equipped with an exhaust system that removes more air than the room is being supplied with. Anterooms are not always necessary for Class N rooms.
Class Q
Class Q rooms are negative pressure rooms that include additional infection control measures such as an anteroom and are used in situations requiring quarantine.
There are higher precautions taken with Class Q rooms, including alarms to alert staff to loss of pressure within the room, self-closing doors, a separate bathroom for the patient, and a ventilation system that does not allow any exhausted air to return into the room.
HEPA filters should be used for the exhaust air to control contaminated air entering the environment outside of the healthcare facility, and communication systems can be used to help staff to safely coordinate movements inside and outside of the room.
There are also Class A pressure rooms, but they are no longer built into new healthcare facilities and are not recommended for use in existing facilities. Class A rooms are alternating pressure rooms that can be used as either negative or positive pressure rooms. However, this increases the risk of human error when setting the airflow for the room, which can cause very serious complications for infection control.
How can room pressure be tested and monitored?
Although there are guidelines from the Centers for Disease Control and Prevention on how to properly monitor and maintain infection control in healthcare facilities, there are no set guidelines on how to monitor acute negative pressure rooms.
To test the pressure inside an acute negative pressure room, a smoke or tissue test can be performed.
To carry out these tests, a smoke capsule or tissue is placed at the bottom of the negative pressure room door. If the smoke or tissue is pulled underneath the door, the room can be seen to be negatively pressurized.
Although this is a simple and cost-effective test, it does not provide continuous monitoring of negative pressure rooms. It also does not show if a room is over or under-pressurized, only that the room is negatively pressurized to some degree.
Electronic monitors placed in the isolation room and the areas outside of the room do offer continuous monitoring of the room pressure. They are equipped with an alarm that will sound if the room becomes incorrectly pressurized.
However, a risk with electronic monitors is that they can become contaminated and provide false readings. Additionally, they are costly and healthcare staff have to be trained to use them.
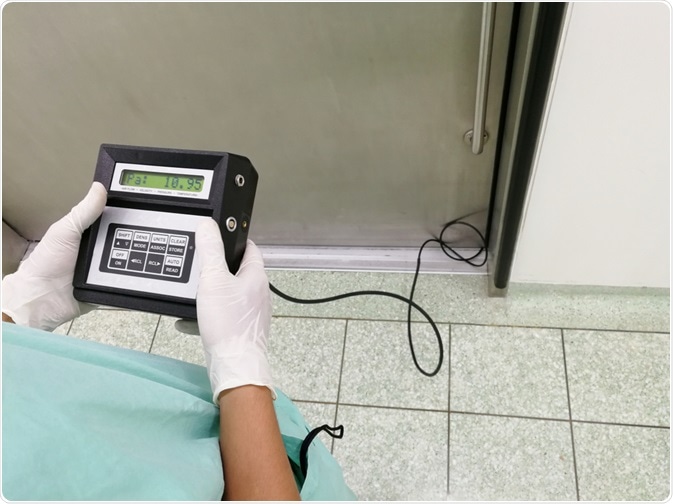
Image Credit: Sucharas Wongpeth/Shutterstock.com
References
Further Reading
Last Updated: Feb 18, 2021