What is vinegar?
Vinegar is an aqueous solution of acetic acid, produced by the fermentation of sugars or ethanol. The solution has been used for thousands of years as a common disinfectant.
The standard white vinegar, which is a clear solution, contains 4 to 7% acetic acid and 93 to 96% water. Some types of white vinegar have up to 20% acetic acid, but this is not safe for human consumption and has been used for cleaning purposes.
Vinegar is the acidic liquid formed through fermentation of carbohydrates. In the past, people made vinegar by fermenting foods like potatoes, sugar beets, and milk whey.
People can also make vinegar using various other ingredients such as diluted alcohol products such as beer, wine, champagne, rice, cider, and distilled grain alcohol.
Nowadays, vinegar is manufactured by the fermentation of grain alcohol or ethanol. But, this type of vinegar doesn’t contain many nutrients. Other ingredients may be added to promote bacterial fermentation, such as phosphates and yeast.

Apple Cider Vinegar. Image Credit: Michelle Lee Photography / Shutterstock
Does vinegar kill bacteria?
Vinegar can kill microorganisms such as bacteria and viruses and treat yeast infections. Due to its antimicrobial properties, vinegar has been used for the treatment of ear infections, warts, and nail fungus. It has also been used to treat certain skin infections and burns.
Vinegar on burn wounds
Many studies support the antimicrobial properties of vinegar. A team of researchers from the University of Birmingham and the National Institute for Health Research (NIHR) examined the antimicrobial property of acetic acid against organisms that cause infection in burn wounds.
The results of the study show that highly diluted acetic acid can inhibit the growth of key burn wound pathogens. The scientists suggested that acetic acid applications offer great promise as an effective and affordable treatment of infections among burn patients.
Vinegar on tuberculosis
Scientists at the Albert Einstein College of Medicine found that acetic acid efficiently kills Mycobacterium tuberculosis, the causative agent of tuberculosis (TB). Vinegar is a nontoxic and affordable treatment for one of the most contagious diseases worldwide. Tuberculosis affected 10 million people across the world in 2017. In the same year, there were 1.3 million tuberculosis-related deaths.
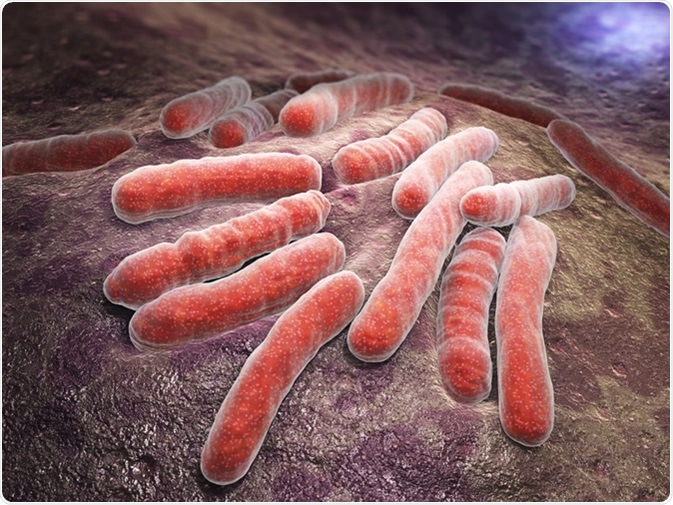
Mycobacterium tuberculosis is a pathogenic bacterial species in the family Mycobacteriaceae and the causative agent of most cases of tuberculosis - Illustration Credit: Tatiana Shepeleva / Shutterstock
Vinegar on antibiotic-resistant chronic wounds
Vinegar has also been effective in killing Pseudomonas aeruginosa, a common bacterium found in chronic wounds. Pseudomonas also causes infections in people with weakened immune systems and those confined in hospital for prolonged periods.
One study found that dilute acetic acid, which is easily available and cheap, is effective in treating chronic wounds. Pseudomonas infections are known to be resistant to many antibiotic treatments. But the topical application of 3 to 5% acetic acid to wounds 2 to 12 times successfully eliminated the bacteria from the wounds.
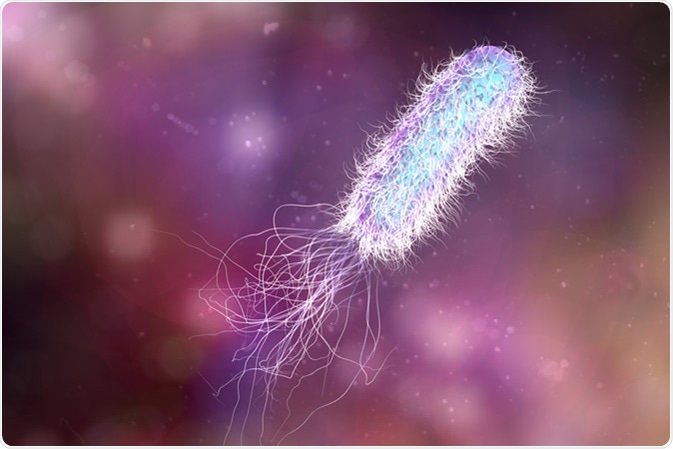
Bacterium Pseudomonas, antibiotic-resistant nosocomial bacterium. Illustration shows polar location of flagella and presence of pili on the bacterial surface - Illustration Credit: Kateryna Kon / Shutterstock
Vinegar on fungus
Aside from its antibacterial properties, vinegar has been effective in treating fungal infections. In one study, the researchers wanted to examine the antifungal activity of apple cider vinegar on certain Candida species. Candida albicans is an opportunistic pathogenic yeast that causes infection of the skin, nails, and mucous membranes. Candidiasis is a common infection affecting the vagina, skin, oral cavity and esophagus.
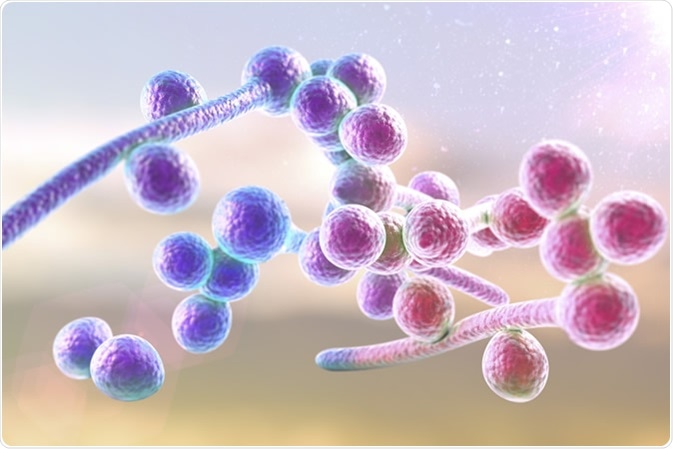
3D illustration of fungi Candida albicans which cause candidiasis - Illustration Credit: Kateryna Kon / Shutterstock
The results of the study show that apple cider vinegar is the most economical product to treat Candidiasis and other fungal infections. Besides its promising effects, it produces no adverse reactions, compared to antifungal drugs.
Vinegar is inexpensive, accessible, and effective in killing microbes, including bacteria and fungus. It can also be used as a safer alternative to bleach for some applications, such as cleaning.
Sources
- Cortesia, C., Vilcheze, C., Bernut, A., Contreras, W., Gomez, K., de Waard, J., Jacobs, W., Kremer, L., Takiff, H. (2014). Acetic acid, the active component of vinegar, is an effective tuberculocidal disinfectant. mBio. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3940030/
- Yagnik, D., Serafin, V., Shah, A. (2018). Antimicrobial activity of apple cider vinegar against Escherichia coli, Staphylococcus aureus and Candida albicans; downregulating cytokine and microbial protein expression. Scientific Reports. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5788933/
- Halstead, F., Rauf, M., Moiemen, N., Bamford, A., Wearn, C., Fraise, A., Lund, P., Oppenheim, B., and Webber, M. (2015). The antibacterial activity of acetic acid against biofilm-producing pathogens of relevance to burns patients. Plos One. journals.plos.org/plosone/article?id=10.1371/journal.pone.0136190
- Madhusudhan, VL. (2015). Efficacy of 1% acetic acid in the treatment of chronic wounds infected with Pseudomonas aeruginosa: prospective randomized controlled clinical trial. International Wound Journal. http://www.bioline.org.br/pdf?gm08019
- Centers for Disease Control and Prevention (CDC). (2016). Disinfection of Healthcare Equipment. www.cdc.gov/.../healthcare-equipment.html
- United States Environmental Protection Agency. (2013). Green cleaning, sanitizing and disinfecting: a toolkit for early care and education.www.epa.gov/.../green_cleaning.pdf.
Further Reading
Last Updated: Jun 13, 2019