Jun 6 2017
To mark HS (hidradenitis suppurativa) Awareness Week from 5-11 June 2017, the Champions for Change campaign (developed and funded by AbbVie Ltd) calls for people who suspect they may have HS to go and see their GP without delay. In addition, it calls for the development of effective patient pathways, to ensure those living with HS see the right specialist at the right time to relieve unnecessary pressure on the NHS while improving patient outcomes.
HS has a prevalence of around 1% of the population, which means that approximately 600,000 people could be living with HS in the UK. However, as it is often misdiagnosed and poorly understood the actual number of people diagnosed is far less than this estimate. A recent survey, amongst 211 HS patients, found over half (52%) of those living with HS wait over four years for a diagnosis, with one in four waiting over ten years.
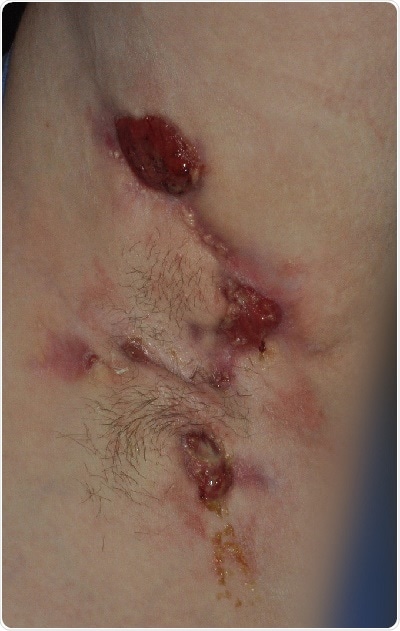
The current burden of unnecessary hospitalisations and associated high costs to the NHS of HS has been shown by new research published ahead of HS Awareness Week. The research, published in the British Journal of Dermatology, found that 3 in 4 (77%) patients with HS who accessed hospital care, presented at A&E departments on average five times over a six year period, often requiring surgical intervention as a result of the severity of their symptoms. The study was funded by AbbVie Ltd.
The cost of poor HS management is significant, with the research suggesting that hospital episodes cost £2,027 per patient per year. Based on the number of patients in the study (11,359) this equates to a cost of over £23 million a year to the NHS in hospital management of HS alone. However, it should be noted that patients selected to be included in the study were likely to be more severely affected.
Delays in diagnosis and referral are often compounded by the lack of investment in secondary care services and healthcare professional training, which can lead to convoluted management of this condition. A review of the crisis in dermatology care recently noted an estimated shortfall of 250 dermatologists in the UK. In addition, the typical undergraduate medical training in dermatology lasts no more than six days, even though 25% of GP appointments involve skin conditions.
Tara Burton, Founder of the HS Trust, says:
Through HS Awareness Week we are trying to bring this condition out into the open, to help the public understand how HS affects patients but also the challenges healthcare professionals face when managing patients with this chronic and debilitating condition. Many people living with HS will struggle to be referred to a dermatologist and even then they will face long waiting times. We need effective patient pathways in place to ensure HS patients are receiving the care they need and keep patients out of A&E. It’s also paramount that we look to find solutions to help overcome the huge capacity issues facing NHS dermatology services if we’re to improve the lives of people with HS.
Dr Brian Malcolm, Associate Specialist and Community Dermatologist, says:
If left undiagnosed and untreated the symptoms of HS can become painful, severe and have a significant impact on the quality of life of patients. It is imperative that this condition is properly treated, but the healthcare profession needs more support to increase access to specialist services for HS. Too many patients are currently in limbo and resorting to emergency services as a fall-back option to manage flare-ups.
 The Champions for Change campaign, developed by AbbVie Ltd, aims to raise awareness of HS in members of the general public and to provide information on the disease and its management.
The Champions for Change campaign, developed by AbbVie Ltd, aims to raise awareness of HS in members of the general public and to provide information on the disease and its management.