The coronavirus disease (COVID-19) pandemic, caused by the severe acute respiratory syndrome virus (SARS-CoV-2), has infected over 37 million people, with over 1 million fatal cases to date. The disease causes fever, dry cough, tiredness, and in more severe cases, difficulty in breathing or shortness of breath, chest pain or pressure, loss of speech or movement. Physicians worldwide have observed that some patients seem unable to recover entirely from COVID-19-related complications, such as shortness of breath, weakness, brain fog, and fatigue.
The infection often leaves behind many complications that may last well past the recovery. In many cases, the symptoms are reported to be long-term. Recent research published as a preprint on the medRxiv* preprint server, Elizabeth T. Cirulli et al., studies the self-reported short and long-term symptoms in a large general adult population cohort.
This study throws light on the frequency of COVID-19 long-term symptoms at the population level. It demonstrates that while people with severe COVID-19 illness develop long-term complications post-recovery, even individuals with mild or asymptomatic infection are at an increased risk of long-term health issues related to the infection.
The authors characterize the frequency, duration, and other properties of long-term COVID-19 symptoms. The results of a prospective research study of the general population represented by participants in the Helix DNA Discovery Project (15,763 participants) and the Healthy Nevada Project (5,596 participants) are undertaken here.
The information was periodically collected between April 2020 and September 2020 on self-reported phenotypes to capture the occurrence and duration of COVID-19 symptoms, COVID-19 infection status, and other long-term outcomes in the general population.
The respondents were asked for longitudinal updates every 4-6 weeks.The study cohort consisted of 233 COVID-19+ cases, 3,652 SARS-CoV-2-negative controls, and 17,474 non-tested individuals - aged 18 to 89+, 63.6% are female, and 83.7% are of European ancestry.
Of the 233 COVID-19+ cases, only 8 (3.4%) were hospitalized. A high percentage of severely ill patients remain affected after 60 or 90 days, while the authors report that the vast majority of mild COVID-19 cases have recovered after 30-60 days. The prevalent long-term COVID-19 symptoms were fatigue, dyspnea, joint pain, chest pain, cough, anosmia, difficulty concentrating, headaches, difficulty sleeping, memory problems, and dizziness.
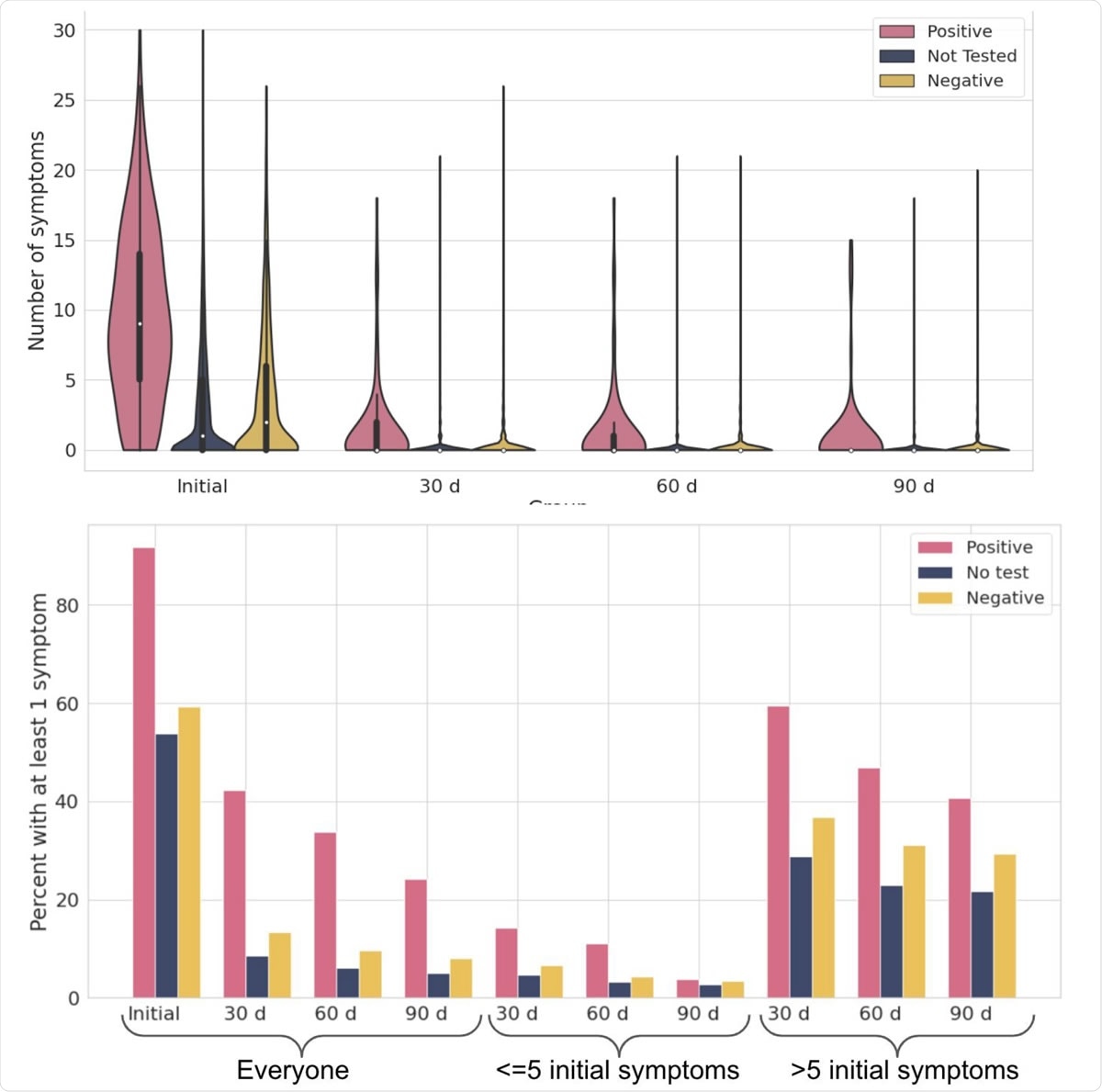
Frequency and duration of symptoms in study participants. A) Violin plot showing the number of symptoms reported in all individuals at each timepoint. B) Percent of participants with at least one symptom during the study period (initial), or at least one symptom that lasted longer than 30 days, 60 days, or 90 days. For the 30, 60, and 90-day timepoints, participants are split into those who initially had 5 or fewer symptoms and those who had more (>5). Individuals whose symptoms had started less than 30, 60 or 90 days ago were excluded from the 30, 60 and 90-day panels, respectively. The study period covered any illness over a nine month period (January - September 2020), and most participants reported at least one symptom occurring during that time frame.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
A high incidence of long-term fatigue in COVID-19 patients is not replicated in this study, possibly because the patients were neither suffering from severe illness nor were hospitalized. From this study, the authors highlight the importance of tachycardia (a rapid heartbeat that may be regular or irregular) and heart palpitations as long-term COVID-19 symptoms.
When compared to the controls, all the symptoms observed in COVID-19 cases were significant. However, only 4 were still significantly enriched when accounting for the level of illness: anosmia (partial or complete loss of smell), ageusia (loss of taste functions), fever, and decreased appetite. In contrast, at 30 days, the significantly enriched symptoms were in the specific subset of individuals who were sicker at the onset of the infection. This demonstrates that COVID-19-specific long-term symptoms are memory loss, anosmia, ageusia, headaches, and tachycardia.
It is important to note that this study takes into account the symptoms from COVID-19+ individuals as well as controls - with the statistical significance of symptoms associated with COVID-19. They have identified that the individuals who are severely ill endure long-term complications. Also, they report that those of the recovered patients who had dyspnea (difficulty in breathing) are at a high risk of suffering long-term complications.
In this study, a high frequency of long-term COVID-19 symptoms are identified, when only 8 of the participants have been hospitalized, and most of the people suffered relatively mild illness. The authors discuss the limitations and possible errors due to the online survey in this study.
This study provides a comparative symptom-information at the population-level: COVID-19 patients, those who tested negative for SARS-CoV-2, and untested individuals from the general population. It is a resource for the community on different COVID-19 symptoms, the prevalence of these symptoms over a period at the population level.
This is a scientifically rigorous study of the long-term effects of COVID-19 from the general population. This study helps us better understand the lasting health burden of SARS-CoV-2 in the overall population. The authors say this study also opens the door for future studies on factors disposing of long-term COVID-19 symptoms as well as genetic studies of susceptibility.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
Journal reference:
- Preliminary scientific report.
Long-term COVID-19 symptoms in a large unselected population, Elizabeth Cirulli, Kelly M Schiabor Barrett, Stephen Riffle, Alexandre Bolze, Iva Neveux, Shaun Dabe, Joseph J Grzymski, James T Lu, Nicole L Washington, medRxiv 2020.10.07.20208702; doi: https://doi.org/10.1101/2020.10.07.20208702, https://www.medrxiv.org/content/10.1101/2020.10.07.20208702v1