A group of researchers from across the United States working in collaboration with their Swiss counterparts have conducted an extensive population-based serological survey to understand the transmission dynamics of severe acute respiratory syndrome coronavirus 2 (SARS CoV-2) – the novel agent that causes coronavirus disease 2019 (COVID-19).
Their study titled, "Household Transmission of SARS-COV-2: Insights from a Population-based Serological Survey," is available on the preprint server site medRxiv.*
The background and need for the study
With a high transmission rate between persons, over 50 million individuals have been infected with SARS CoV-2 around the world since it first emerged in Wuhan, China, in late December 2019.
Those in household contact with an infected person are thus at a greater risk of acquiring the virus. Studies looking at the transmission of the virus within household contacts are thus vital in better understanding COVID-19's transmission.
At present, studies looking at the household transmission of COVID-19 depend on detecting contact-based infections by using reverse transcription-polymerase chain reaction tests (RT-PCR), a nuclear-derived method that can detect the presence of SARS-CoV-2's genetic material in host cells. This is currently the most common form of testing and is usually conducted using nasal swab samples. Currently, those who have been in contact with individuals exhibiting mild symptoms or no symptoms may be missed in RT-PCR testing due to the limited time window in which virological testing may yield positive results. The study's authors explain that these limitations may underestimate the actual mild or asymptomatic cases among the household contacts and miscalculate the household secondary attack rates.
Serological surveys
Serological surveys search for the presence of antibodies against SARS-CoV-2 in a person's blood. The researchers suggest that this form of testing could be an effective alternative way to detect the virus's spread among household contacts. For one, these serological surveys yield positive results for an infected person for a longer duration compared to the RT-PCR test.
A recent large meta-analysis of other studies has shown that the household secondary attack rate is around 17 percent. Studies have thus missed several aspects in estimating household infection rates and so to help fill the knowledge gaps. This study was undertaken using serological surveys.
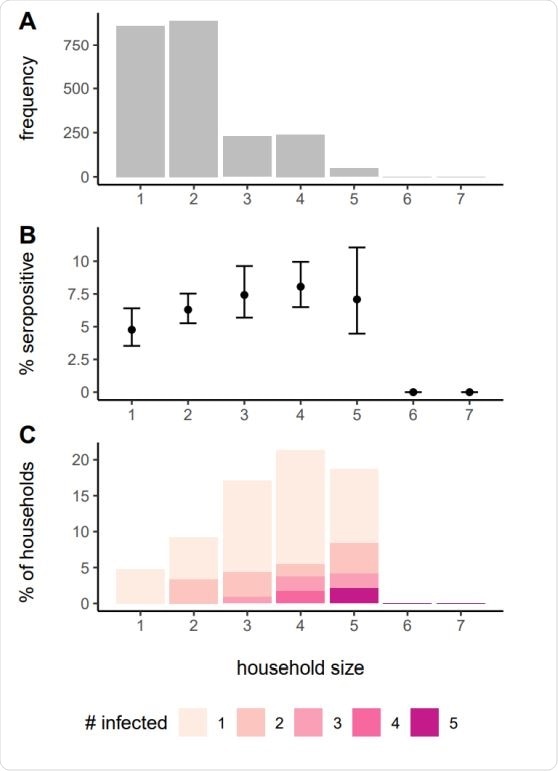
Frequency of households of different sizes in the study (A), proportion seropositive by house size (B) and distribution of the number of seropositive people in household by size (C).

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Importance of this study
This study was undertaken to clarify the transmissibility of asymptomatic infections as well as infections from household and community contacts among patients with COVID-19. This would help understand and design ways to control the spread of the infection, wrote the researchers. Serological studies helped detect all previously infected individuals, the team wrote.
Study design
This was the SEROCoV-POP study, which is a population-based study of individuals aged between 20 and 74 years from Geneva (Canton), Switzerland.
All the participants in the survey (10,587 in total) were invited to take part in the serological survey. Participants were asked to bring all the members in their household aged over 5 years. Within household and external household contacts were taken into account since January 2020.
All the participants of the study and household contacts were asked about any symptoms they may have, including cough, fever, shortness of breath, or loss of smell or taste since January 2020 up till 2 weeks prior to the serological blood test. For all the participants, anti-SARS-CoV-2 IgG antibodies were detected using enzyme-linked immunosorbent assay (ELISA) tests. The antibodies were against the S1 domain of the spike protein of SARS-CoV-2.
The team utilized chain-binomial models to assess the number of infections spread within the households and estimated the risk of transmission within the household and extra-household contacts.
Results
For this study, a total of 4,524 household members 5 years and older participated from 2,267 households between April and June 2020. The median age was 53 years, and 53.6 percent of the participants were female. Overall results were:
- The risk of infection from a single infected household contact was 17.2 percent (95% CrI 13.6-21.5 percent)
- The risk of infection from an extra-household contact was 5.1 percent (95% CrI 4.5-5.8 percent)
- With increasing age, the risk of getting infected from a household contact rose from 7.5 percent (95% CrI 1.3-20.3 percent) among children aged between 5 and 9 years to 30.2 percent (95% CrI 14.3-48.2 percent) among those over the age of 65 years.
- The risk of infection from an extra-household contact was greatest among the working-age group of individuals aged between 20 and 49 years.
- Household contacts who were positive for antibodies but did not have symptoms of COVID-19 had a 74.8 percent lower odds (95% CrI 43.8-90.3 percent) of infecting another household member when compared to a positive contact who had symptoms (19.6 percent 95% CrI 12.9-24.5 percent).
Conclusions and implications
This study shows that the risk of getting infected with SARS CoV-2 after exposure to a single infected household member was four-times greater than from an external positive contact. The team noted that younger children were at a lower risk of getting infected from household contacts compared to the elderly and asymptomatic cases are less likely to spread the infection among contacts within the household. The authors wrote, "While the small households in Geneva limit the contribution of household spread, household transmission likely plays a greater role in other settings."

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Qifang Bi, Justin Lessler and Isabella Eckerle et al. (2020) 'Household Transmission of SARS-COV-2: Insights from a Population-based Serological Survey' medRxiv preprint server; doi: https://doi.org/10.1101/2020.11.04.20225573, https://www.medrxiv.org/content/10.1101/2020.11.04.20225573v1
- Peer reviewed and published scientific report.
Bi, Qifang, Justin Lessler, Isabella Eckerle, Stephen A. Lauer, Laurent Kaiser, Nicolas Vuilleumier, Derek A. T. Cummings, et al. 2021. “Insights into Household Transmission of SARS-CoV-2 from a Population-Based Serological Survey.” Nature Communications 12 (1). https://doi.org/10.1038/s41467-021-23733-5. https://www.nature.com/articles/s41467-021-23733-5.