Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) cases are increasing across the globe in a horrible second wave as of late 2020. Governments worldwide continue to struggle to contain the virus while protecting their economies at the same time. One controversial but effective method used widely for viral containment is strict lockdowns or stay-at-home orders.
While this strategy was successful in some Asian and European countries, lockdowns in the US have made policymakers question the long-term feasibility of this strategy. The effects of lockdowns go beyond the economic and political ramifications, and studies show stay-at-home orders affect physical and mental health of healthy individuals. However, there are no comprehensive and quantitative scientific studies on the long-term lockdowns to date.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
A precision fitness case study investigating the effect of lockdowns on daily activities of individuals
Researchers from the University of Texas, San Antonio and UT-Health Sciences, Texas, recently attempted to fill this knowledge gap by addressing how the COVID-19 pandemic and related stay-at-home orders are changing the daily habits of individuals. They investigated the effect of lockdowns on 61 individuals in San Antonio, Texas, by recording their daily activity and sleep data using wearable activity trackers for over 12 months from April to August 2020. Their study is published on the preprint paper medRxiv*.
The researchers assessed changes in six fitness parameters such as steps walked, sedentary minutes, resting heart rate, wake duration after sleep onset, total sleep duration, and rapid eye movement (REM) duration. They used cluster analysis and time course analysis to identify trends in activity before, during, and after stay-at-home orders. Quantitative measures of various activities were compared to participants' survey responses.
To assess whether stay-at-home orders or other pandemic-related events affected daily behavior in the city residents, the team focused on three key parameters. They were: the date on which the most significant inflection point was seen in daily behaviors, the demographic and health profile of individuals whose behavior improved or changed for the worse during the stay-at-home periods, and if self-evaluation is an effective measure of health during this period.
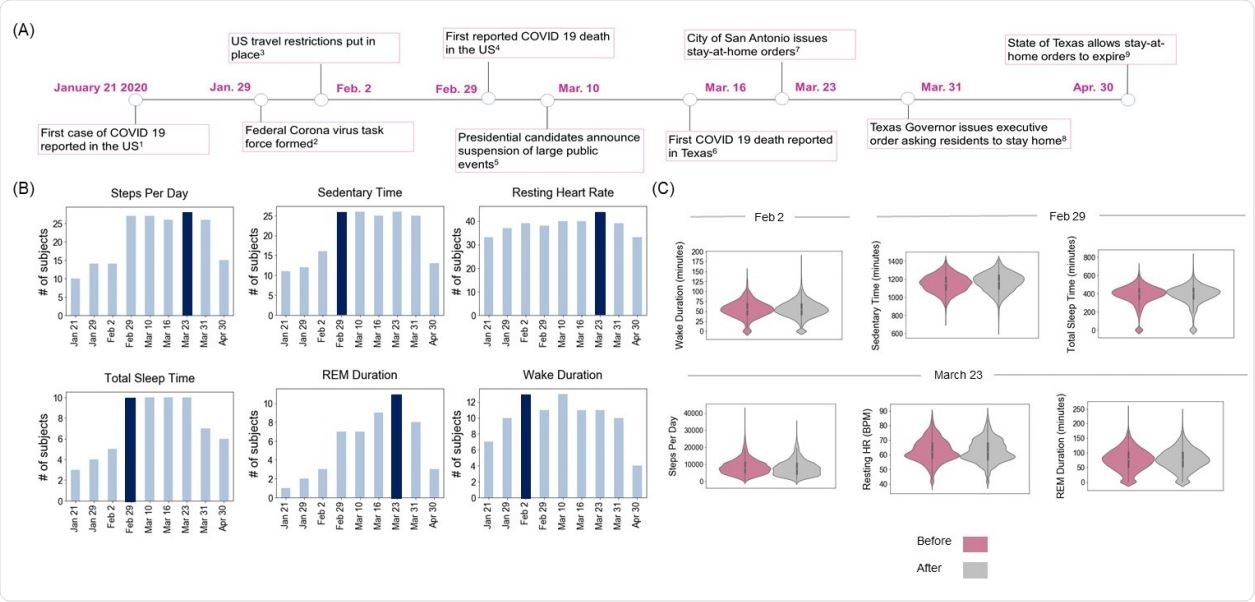
Events affecting daily activity during the COVID19 pandemic (A) Timeline of prominent COVID 19 events relevant to the subjects in Texas, January 2020 to April 2020. (B) The number of subjects (of 61 total subjects) with statistically significant changes for six daily activity metrics (steps, sedentary time, resting heartrate, total sleep time, REM duration and wake duration) at those dates. (C) Violin plots showing the probability density of the six activity metrics for subjects before (magenta) and after (gray) the date for which most people had a significant change in the variable.
Inflection points corresponded with the beginning of the pandemic and reporting of the first case
The results identified four behavior patterns in the individuals during stay-at-home periods. They found that most individuals suffered a decline in healthy daily habits during the pandemic-related lockdown times compared to their day to day activities in 2019 and early 2020. The identified inflection points corresponded with crucial dates relevant to the starting of the SARS-CoV-2 pandemic, including the reporting of the first case in the US on February 29 and the city-wide stay-at-home orders on March 23.
Pre-existing conditions such as diabetes and asthma were associated with a sharper than average decline in the quality of sleep during stay-at-home orders. Surprisingly, they also identified a group of predominately male participants who improved their daily fitness during the stay-at-home periods.
"An exciting, unexpected conclusion from this work is that there exists a subset of individuals whose health quantitatively improves – better sleep, more exercise, lower resting heart rate – in the midst of a devastating pandemic and the accompanying restrictions imposed by stay-at-home orders."
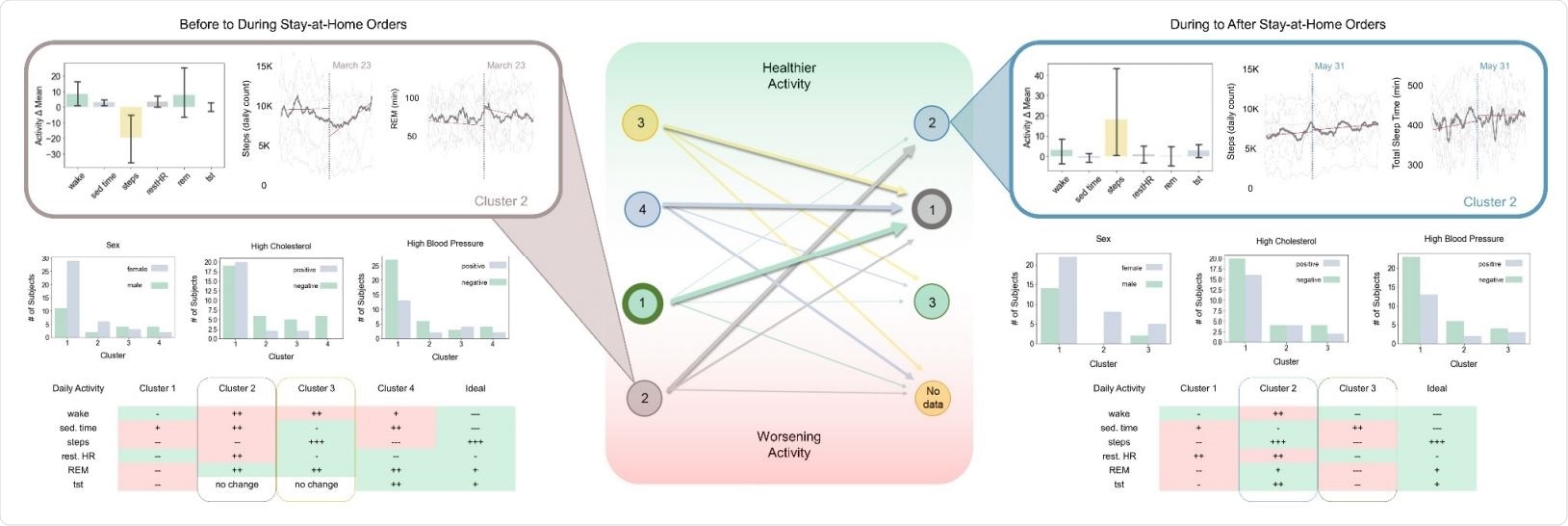
Activity Patterns Identified by Cluster Analysis Four clusters before/during (left) and during/after (right) stay-at-home orders were identified. Shifts in cluster membership during these two time periods are shown in the center. The width of outlines and arrows represent the relative number of subjects in that group. Clusters are rank ordered by the healthiness of the observed activity trend. Representative activity patterns are displayed in the inset images for Cluster 2, which contained subjects with the worst health trends during stay-at-home orders (left inset), and Cluster 2B, which included subjects with the healthiest activity after stay-at-home orders were lifted (right inset). Select demographic and health data for shown for all clusters. See Appendices B, D, E and F for additional details.
Fitness declined in most individuals and improved in a few individuals during the stay-at-home period
As per the study's findings, the objective measures of daily activity indicated that the fitness of most individuals suffered at the beginning of stay-at-home orders but slowly returned towards baseline as time progressed. Fitness levels quantitatively improved for a subset of individuals in terms of more exercise, better sleep, and lower resting heart rate during the stay-at-home period.
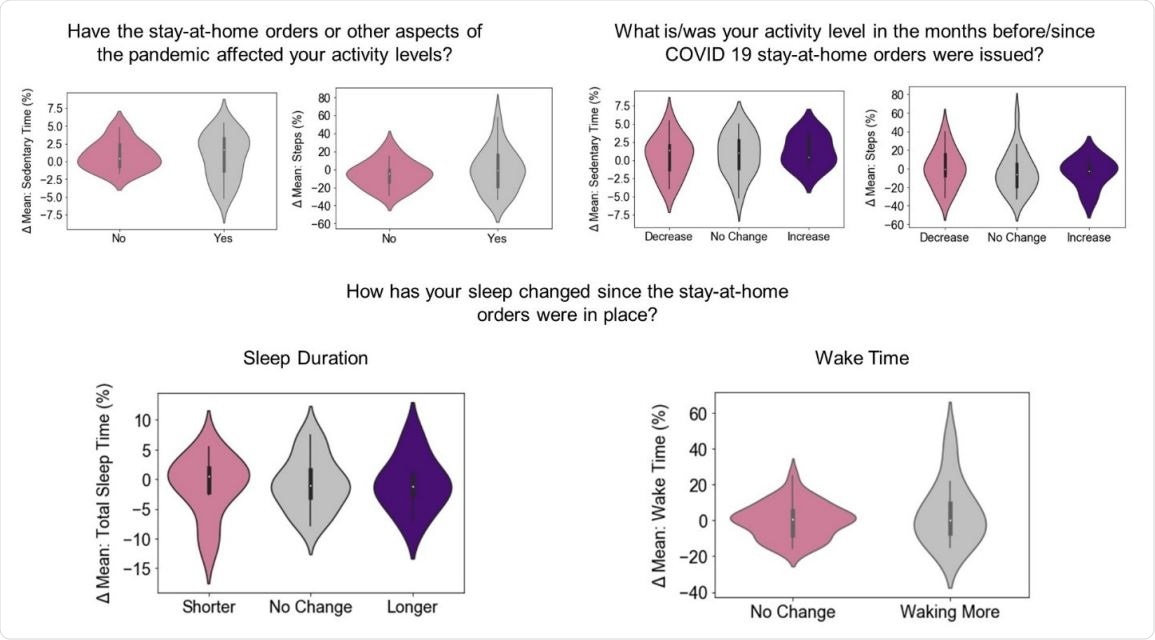
Quantitative vs. qualitative measures of daily activity Subjects’ recorded activity levels (y-axis) compared to the same subjects’ responses (x-axis) to three survey questions (titles).
The authors believe that these findings have the potential to guide policy-making by highlighting how the pandemic-related stay-at-home orders quantitatively impact the daily health of a population. The authors feel that further work on this in the future will help understand in detail the mitigation methods that are most effective in fighting a pandemic while maintaining optimal health.
"Benefits of this study include a data-rich, 16-month quantitative analysis of daily activity before and during the pandemic."

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.