Researchers in Italy have demonstrated the efficacy of using modified outer membrane vesicles (OMVs) as a vaccine to protect against coronavirus disease 2019 (COVID-19) in an animal model.
These OMVs are bacteria-derived vesicles that can be engineered to incorporate different viral antigens to induce potent immune responses.
Now, Guido Grandi from the University of Trento and colleagues have shown that OMVs incorporating peptides derived from the spike protein of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) – the agent that causes COVID-19 – elicit an effective immune response when administered to mice.
Vaccination induced neutralizing antibody titers that were sufficient to protect mice that were challenged with the original SARS-CoV-2 strain that was identified in Wuhan, China (Wuhan-1 isolate).
Furthermore, the team showed that the OMVs could be successfully engineered to induce immunity against a different SARS-CoV-2 variant.
"Altogether, given the convenience associated with ease of engineering, production and distribution, our results demonstrate that OMV-based SARS-CoV-2 vaccines can be a crucial addition to the vaccines currently available," writes Guido Grandi from the University of Trento and colleagues.
A pre-print version of the research paper is available on the bioRxiv* server, while the article undergoes peer review.

 *Important notice: bioRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: bioRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
More about the vaccines available so far
The rapid rollout of vaccination protecting against SARS-CoV-2 infection represents the most promising approach to combatting the COVID-19 pandemic.
Given the continuous evolution of SARS-CoV-2 and the emergence of multiple variants of concern, an effective long-term strategy where vaccines are updated depending on the extent of antigenic drift is likely to be crucial.
More than 280 candidate vaccines are currently under different development stages, with more than 100 now being evaluated in phase 2 clinical trials.
While protein-based vaccines comprise the most significant portion of these products, messenger RNA- (mRNA) and viral vector-based vaccines were the first to receive emergency use authorization for mass rollout globally.
"As a result, the world witnessed an unprecedented technical and economical challenge, given the need to manufacture, distribute, store, and administer billions of doses of vaccines in every country," writes Grandi and colleagues.
To overcome such challenges, vaccine production needs to use easily scalable and low-cost processes to ensure immunization is available to all countries, irrespective of economic and climatic conditions.
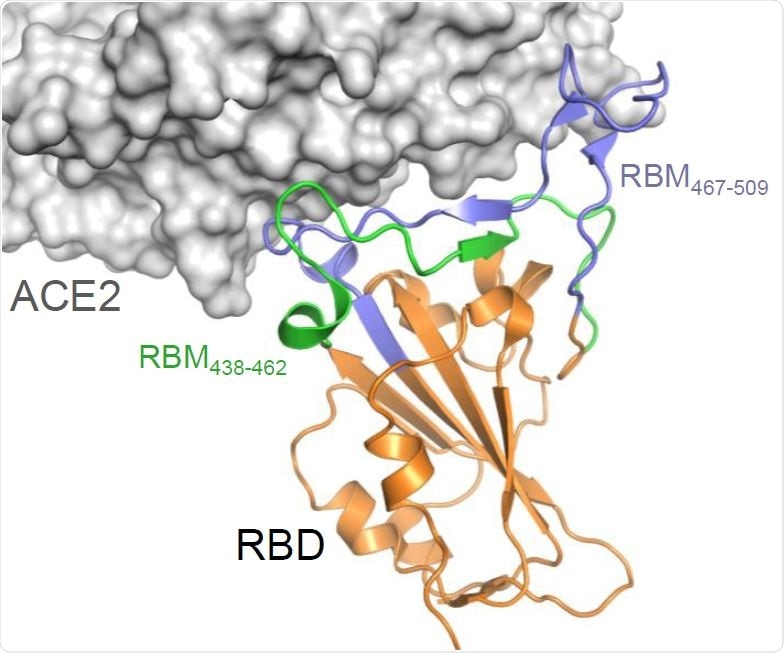
Construction and production of OMVs carrying SARS-CoV-2 RBM antigens (A) Topology of the interaction between SARS-CoV-2 RBD and ACE2 with the indication of the two RBM polypeptides tested in this study.
Where do OMVs come in?
Over recent years, OMVs have emerged as an attractive tool capable of coupling excellent built-in adjuvanticity with an easily scalable production and purification process.
"Crucially, in addition to the simple and cost-effective set-up required to produce and purify OMVs, the antigen-decorated vesicles are extremely stable for long-term storage at room temperature, making it a convenient vaccine to distribute all over the world," says Grandi and colleagues.
What did the researchers do?
The researchers engineered OMVs that incorporated peptides from the receptor-binding motif (RBM) of the SARS-CoV-2 spike protein. This spike RBM forms the interface with the human host cell receptor angiotensin-converting enzyme 2 (ACE2) during the initial stage of the infection process.
When the team administered the OMVs to CD1 mice, all sera collected from the animals contained high levels of RBM-specific immunoglobulin G (IgG) antibodies.
To test whether antibodies could also neutralize SARS-CoV-2 infection in vitro, the team performed a neutralization assay using a lentiviral vector pseudotyped with spike protein derived from the Wuhan-1 isolate.
The researchers found that the OMVs effectively neutralized these SARS-CoV-2 spike-pseudotyped vectors.
The vaccine protected mice infected with SARS-CoV-2
To test the vaccine's protective effect in vivo, the team immunized eight K18-hACE2 transgenic mice with a prime 10μg dose of the OMVs or phosphate-buffered saline (PBS), followed by a second dose of OMVs or PBS 14 days later. They then infected the mice intranasally with SARS-CoV-2.
By day four following infection, the PBS-treated mice had developed severe disease, while the mice treated with OMVs developed a much milder disease.
When the team tested samples taken from the lungs of the animals five days post-infection, they found that viral RNA and replicating virus could only be detected in one of four immunized mice, indicating the ability of the vaccine to prevent viral replication in the respiratory tract.
Finally, the researchers engineered OMVs incorporating RBM peptides derived from a different genetic variant of SARS-CoV-2. When mice were vaccinated with these OMVs, a similarly potent neutralization activity was observed.
A "promising candidate" for SARS-CoV-2 vaccination
Grandi and colleagues say the immunity induced by the OMV-based vaccine is sufficient to protect K18-hACE2 transgenic mice from intranasal challenge with SARS-CoV-2.
"Given the efficacy of the vaccine in the animal model, the ease of its engineering, the cost-effective production process, and the stability at room temperature, we propose the OMV-based vaccine as a promising candidate to continue the vaccination campaign against SARS-CoV-2," they conclude.

 *Important notice: bioRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: bioRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.