The binding responses and temporal dynamics of antibodies elicited against the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) due to vaccination must be fully understood to design future vaccination strategies.

Study: 6 month serologic response to the Pfizer-BioNTech COVID-19 vaccine among healthcare workers. Image Credit: Flowersandtraveling / Shutterstock.com
BNT162b2 vaccine
BNT162b2 is a messenger ribonucleic acid (mRNA) vaccine by Pfizer-BioNTech. The U.S. Food and Drug Administration (FDA) authorized the BNT162b2 vaccine for emergency use on December 11, 2020.
SARS-COV-2 binds and infects the host cells through the spike (S) protein receptor-binding domain (RBD) that is exposed on the surface of the virus. The BNT162b2 vaccine mRNA encodes a secreted trimerized SARS-CoV-2 RBD. The RNA is nucleoside-modified and enclosed within a lipid nanoparticle.
Six-month serologic response assessment
Healthcare workers were among the first individuals to receive COVID-19 vaccination. Therefore, the current observational study enrolled adult participants working in a large healthcare system.
The study participants received the BNT162b2 vaccine at week 0 and week three. Blood samples were collected on the day of vaccination (baseline), as well as two weeks, four weeks, three months, and six months after vaccination.
Anti-SARS-CoV-2 antibodies were analyzed using the Maverick SARS-CoV-2 multiantigen panel that detected nucleocapsid, spike S1 RBD, spike S1S2, spike S1, and spike S2 antigens.
The change in total antibodies, IgM, and IgG responses across all time points were evaluated.
Serology results
A total of 15 study participants completed all five blood collections. Among the 15 participants, six were office staff, three were nurses, one was a physician assistant, two were medical assistants, two were physicians, and one was with an unknown role in the healthcare system.
The average age of the participants was 44 years and 82% of participants were females. None of the participants reported prior symptoms of COVID-19 or prior COVID-19 polymerase chain reaction (PCR) test positivity.
Sera samples were analyzed to examine the humoral response to the BNT162b2 vaccine. Ten 10 different types of anti-SARS-CoV-2 antibodies were assayed, including four IgM and four IgG antibodies targeting each of four different spike protein epitopes, as well as one IgM and one IgG antibody targeting the nucleocapsid epitope.
All participants had a significant serologic response across time for total antibody. The serologic response across time was significant for both IgG and IgM antibody responses. The serologic response was largely driven by IgG antibodies.
Vaccination elicited an IgG-dominant antibody response. Most of the participants had an IgG response at two weeks after vaccination.
There were significant increases in mean response between baseline and week four for anti-SARS-CoV-2 IgG against spike S1, spike S1 RBD, spike S1S2, and spike S2 IgG. Thus, the IgG response was observed at two weeks following vaccination in most participants and continued to increase at week four. However, the IgG response against all spike protein epitopes significantly decreased starting at three months and up to six months.
The IgM response to all epitopes was minimal; however, one patient had pre-existing IgG antibodies against the nucleocapsid antigen. This confirmed a prior asymptomatic infection.
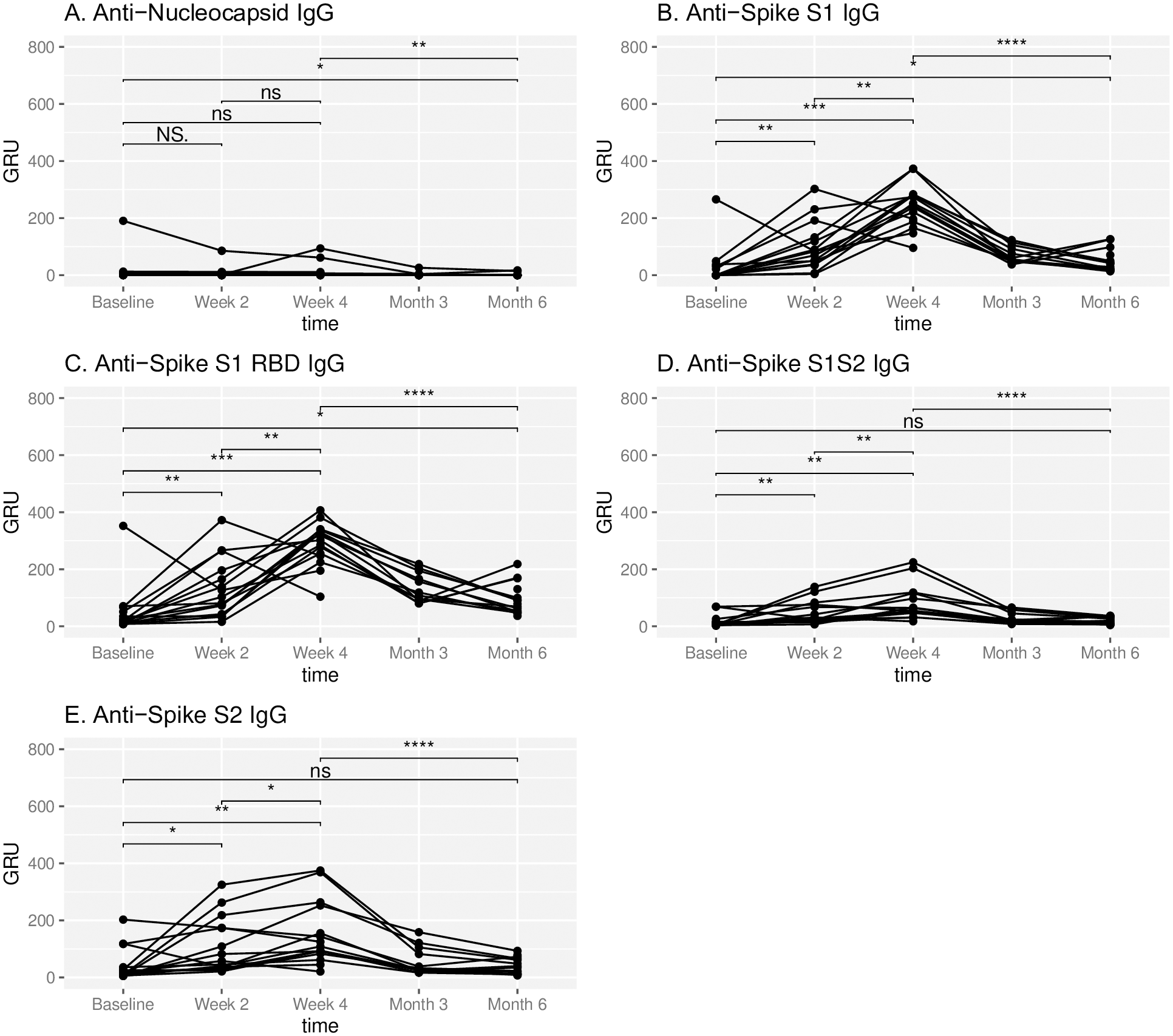
Temporal IgG response to SARS-CoV-2. IgG antibody response to respective SARS-CoV-2 epitopes at baseline, week 2, week 4, month 3 and month 6 in subjects administered Pfizer-BioNTech COVID-19 vaccine at week 0 and week 3. Antibody response is reported in Genalyte response units (GRU). NS represents a p-value >0.05, * represents a p-value ≤ 0.05, ** represents a p-value ≤ 0.01, *** represents a p-value ≤ 0.001, **** represents a p-value ≤ 0.0001.
Implications
The antibody response to the spike protein significantly decreases six months after vaccination with the BNT162b2 vaccine. However, it remains to be determined if this antibody decline correlates with waning immunity.
For this purpose, the change in infection risk with respect to time post-vaccination should be evaluated. The cellular response to vaccination should also be examined to identify the complete vaccine-directed immunity.
The current study provides data to inform current research investigating the potential of a booster dose to expand the level and duration of immunity. This is particularly important in the context of emerging SARS-CoV-2 variants.
This study also provides new insights into the response that can be expected for other mRNA vaccination targets. Furthermore, the study findings provide a comparison for assessing the humoral response in immunocompromised patients, as this population requires innovative strategies to enhance vaccine immunogenicity.
Conclusions
Vaccination with BNT162b2 elicits minimal anti-SARS-CoV-2 IgM response against the spike protein. This is contrary to natural SARS-CoV-2 infection.
Polyclonal IgG response against the spike protein is elicited by two weeks following vaccination and continues to increase at week four, but then declines at three months and continues to decline up to six months.
Journal reference:
- Cham, J., Pandey, A. C., New, J., et al. (2022) 6 month serologic response to the Pfizer-BioNTech COVID-19 vaccine among healthcare workers. PLoS ONE 17(4). doi:10.1371/journal.pone.0266781.