Researchers in the UK, United States, and Sweden have presented new findings that could help identify individuals at risk of "long COVID" – a protracted course of coronavirus disease 2019 (COVID-19) symptoms last for more than 28 days.

Study: Attributes and predictors of Long-COVID: analysis of COVID cases and their symptoms collected by the Covid Symptoms Study App. Image Credit: Tomas Ragina / Shutterstock
The findings come from an analysis of data available for more than 4,000 people with COVID-19 who reported their symptoms prospectively using the COVID Symptom Study app.
Claire Steves (King's College London) and the team found that long COVID was characterized by fatigue, headache, difficulty breathing (dyspnea), and a loss of sense of smell (anosmia).
They also found that long COVID was more likely to develop with increasing age, body mass index (BMI), and female gender.
Furthermore, a predictive model the researchers, developed showed that experiencing more than five symptoms in the first week of illness was a significant predictor of long-COVID.
"This model could be used to identify individuals for clinical trials to reduce long-term symptoms and target education and rehabilitation services," write Steves and colleagues.
A pre-print version of the paper is available on the server medRxiv*, while the article undergoes peer review.
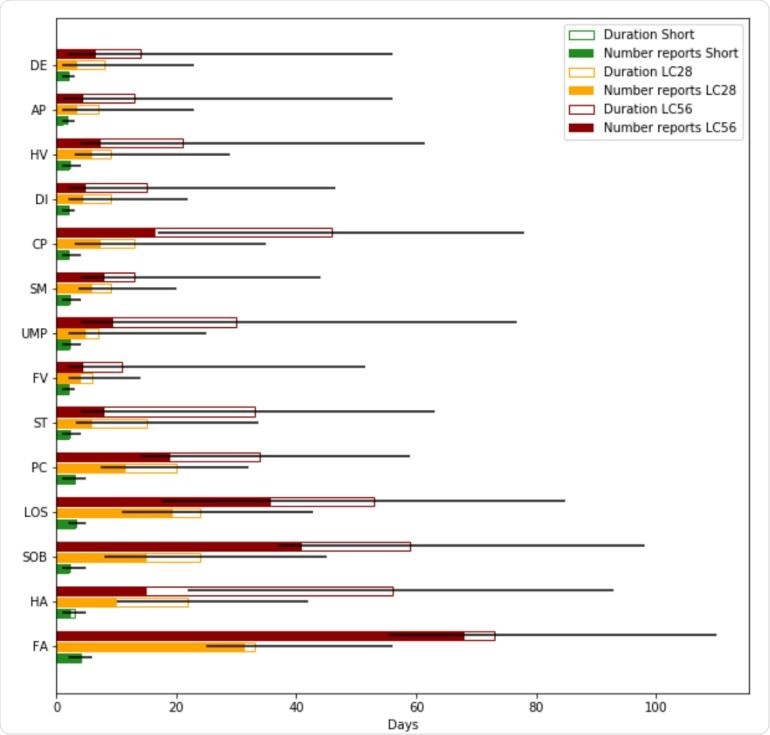
Symptoms by duration. For each symptom (ordered from top to bottom by increasing frequency of occurrence) the median duration of report is presented by the total (hollowed) bar height, with associated interquartile range represented by the black line, for the short, LC28 and LC56 durations. The filled bars represent the number of times a report has been given. This highlights the differences in the symptoms in terms of their intermittence throughout the course of the disease. (Abbreviations DE – delirium, AP – Abdominal Pain, HV – Hoarse Voice, DI – Diarrhoea, CP – Chest Pain, SM – skipped meals, UMP – Unusual Muscle pains, FV – Fever, ST – Sore Throat, PC – Persistent Cough, LOS – Loss of smell, SOB – Shortness of breath, HA – Headache, FA – Fatigue)
Reports of long COVID are increasing
An increasing number of long COVID-19 cases are being reported. Yet, little is known about the prevalence or risk factors for this protracted disease or whether it is possible to predict its development based on early symptoms.
Furthermore, "few studies capture symptoms prospectively in the general population to ascertain with accuracy the duration of illness and the prevalence of long-lasting symptoms," say Steves and team. "At the population level, it is critical to quantify the burden of long COVID to better assess its impact on the healthcare system and appropriately distribute resources."
What did the researchers do?
The team analyzed data available for a subset of 4,182 incident cases of COVID-19 who reported their symptoms prospectively using the COVID Symptom Study app.
More specifically, the subset was made up of individuals who had tested PCR-swab-positive for COVID-19 and reported "feeling physically normal" before the start of illness (up to 14 days before testing), helping the team to determine onset.
Of the 4,182 app users, 558 (13.3%) met the definition of long COVID (symptoms lasting more than 28 days), of whom 189 (4.5%) reported symptoms lasting more than eight weeks and 95 (2.3%) reported symptoms lasting more than 12 weeks.
In contrast, 1,591 (38.0%) met the definition for short COVID (symptoms lasting less than ten days).
What did the study find?
The most frequently reported symptoms among those with long COVID were fatigue (97%) and headache (91.2%), followed by anosmia and lower respiratory symptoms.
The team identified a significant association between age and the prevalence of long COVID, which increased from 9.9% among those aged 18 to 49 years to 21.9% among those aged more than 70 years.
Long COVID was significantly more common among women than among men, at a prevalence of 14.9% versus 9.5%, although this gender effect was not significant among the elderly.
Predicting long COVID based on early disease features
Next, the researchers assessed whether the risk for long COVID could be predicted based on early disease features.
Steves and colleagues found that individuals reporting more than five symptoms during the first week of illness were at a more than 3-fold greater odds of experiencing long COVID.
The team then created Random Forest Prediction models using a combination of symptoms reported in the first week, personal characteristics, and comorbidities.
When all features were incorporated, the model successfully distinguished between long COVID and short COVID, with the strongest predictor being age, followed by a number of symptoms during the first week, BMI, hoarse voice, shortness of breath, and gender.
When the researchers simplified this prediction model to only include symptom numbers in the first week, along with age and sex, they found it was still possible to accurately distinguish between individuals with long COVID and those with short COVID.
The findings were validated in an independent dataset
Importantly, the predictive findings were validated in an independent dataset of 2,472 people who reported being positive for COVID-19 antibodies from two weeks post symptom onset.
Again, the symptom number in the first week of illness was the strongest predictor of long COVID.
"This important information could feature in highly needed targeted education material for both patients and healthcare providers," say Steves and colleagues.
"Moreover, the method could help determine at-risk groups and could be used to target early intervention trials of treatment (for example, of dexamethasone and remdesivir) and clinical service developments to support rehabilitation in primary and specialist care to alleviate Long-COVID and facilitate timely recovery," concludes the team.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Steves C, et al. Attributes and predictors of Long-COVID: analysis of COVID cases and their symptoms collected by the Covid Symptoms Study App. medRxiv, 2020. doi: https://doi.org/10.1101/2020.10.19.20214494, https://www.medrxiv.org/content/10.1101/2020.10.19.20214494v1
- Peer reviewed and published scientific report.
Sudre, Carole H., Benjamin Murray, Thomas Varsavsky, Mark S. Graham, Rose S. Penfold, Ruth C. Bowyer, Joan Capdevila Pujol, et al. 2021. “Attributes and Predictors of Long COVID.” Nature Medicine 27 (4): 626–31. https://doi.org/10.1038/s41591-021-01292-y. https://www.nature.com/articles/s41591-021-01292-y.