The emergence of a novel coronavirus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) led to a group of pneumonia cases in Wuhan, China, in late 2019. SARS-CoV-2 caused coronavirus Disease 2019 (COVID-19), resulting in an epidemic in China followed by a global pandemic.
Recent reports indicate that SARS-CoV-2 has infected over 266 million individuals worldwide and claimed the lives of more than 5.26 million. COVID-19 is characterized by high transmissibility, variable clinical presentation, and symptom severity. Estimates range from 33 to 77 percent of individuals infected as asymptomatic. However, it has also been reported that few of the asymptomatic individuals may consist of unnoticed clinical abnormalities.
Reports also suggest that among the patients who test positive for COVID-19, 80 percent have mild disease, 15 percent have severe disease, and 5 percent have a critical disease. In addition, the overall fatality rate has been found to be 2 percent, while the fatality rate for hospitalized individuals was found to be 10 to 20 percent.
A new study by researchers at Northeastern University focused only on COVID-19 patients with type 1 diabetes, alopecia, and vitiligo. Alopecia is an autoimmune disorder that targets the hair follicles, vitiligo autoimmune/inflammatory disease that attacks the pigment cells on the epidermal layer, and diabetes affects the pancreas.
The study, published on the pre-print server medRxiv*, analyzed the specific linkages between the COVID-19 patients belonging to the three risk groups with the overall COVID-19 patients and compared symptoms between and within the risk groups.
The study also aimed to determine whether autoimmunity/inflammatory action had any impact on the severity of SARS-CoV-2 infections.
 Study: Assessment of correlations between risk factors and symptom presentation among defined at-risk groups following a confirmed COVID-19 diagnosis. Image Credit: GoodStudio / Shutterstock
Study: Assessment of correlations between risk factors and symptom presentation among defined at-risk groups following a confirmed COVID-19 diagnosis. Image Credit: GoodStudio / Shutterstock

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
About the study
The study was carried out in two phases. Phase I involved determining whether a significant difference existed between the occurrence of a particular symptom when compared with all other symptoms studied in COVID-19 patients who belong to the overall group and the risk group. Phase II helped determine whether significant differences existed in symptom presentation in COVID-19 patients with comorbid autoimmune disorders having different severity and location.
The study analyzed three experimental groups, type 1 diabetes, vitiligo, and alopecia patients and one control group. All the groups had to test positive for SARS-CoV-2 infection. The study data was obtained from the N3C Enclave, which is an endeavor led by the National Center for Advancing Translational Science (NCATS).
Furthermore, concept sets were created and utilized for the fourteen most common symptoms associated with COVID-19 infection. The study also determined COVID-19 positivity through laboratory tests and determined symptom occurrence in all patients who possessed at least one symptom defined in the concept set.
Study findings
The study results found no significant difference between symptom presentation in the risk groups compared to the overall groups. However, the results indicated a higher COVID-19 symptom percentage across all the immune groups except type 1 diabetes, where the percentages were found to be slightly lower than the overall group. Also, 0 percent of patients were found to fall under the rash group except for the alopecia group, where less than 1 percent of patients were found to develop alopecia within one month of symptom onset.
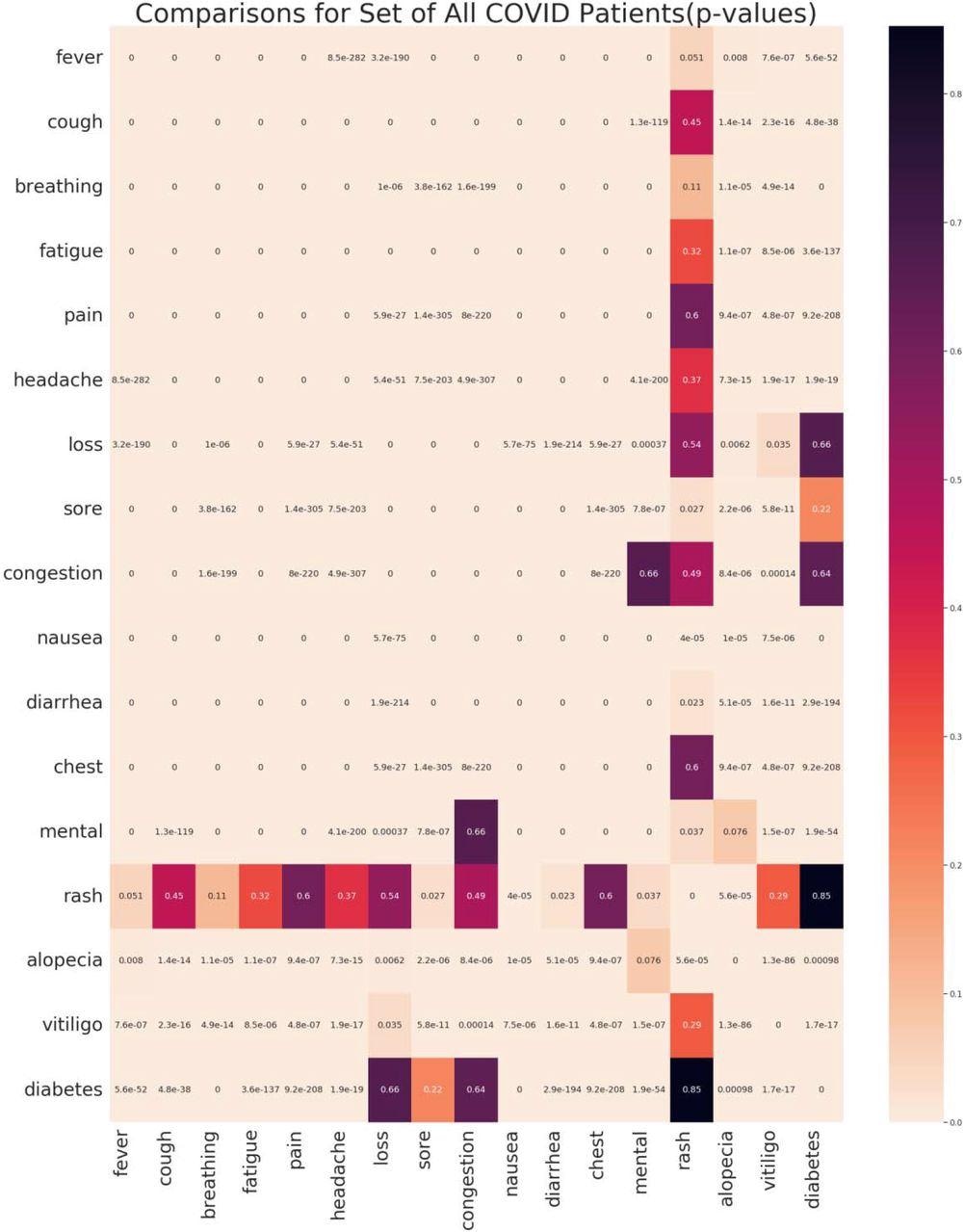 Heatmap of p-values in set of All COVID positive patients for comparison of all symptoms to every other symptom and comparison to each of the three immune groups (alopecia, vitiligo, and type 1 diabetes); color intensity increases with decreasing value; the following abbreviations were utilized: breathing (breathing abnormalities), loss (loss of taste/smell), chest (chest pain/pressure), mental (impairment of consciousness)
Heatmap of p-values in set of All COVID positive patients for comparison of all symptoms to every other symptom and comparison to each of the three immune groups (alopecia, vitiligo, and type 1 diabetes); color intensity increases with decreasing value; the following abbreviations were utilized: breathing (breathing abnormalities), loss (loss of taste/smell), chest (chest pain/pressure), mental (impairment of consciousness)
The results also indicated a significant relationship between the three immune groups and the fourteen symptoms included under the concept set. However, some exceptions existed, such as the alopecia group had a lack of significance for the mental (impairment of consciousness) symptom group, the type 1 diabetes group had a lack of significance for the rash, congestion, sore throat, and loss of smell/taste group, and the vitiligo group had a lack of significance for the rash group. Furthermore, symptom interactions among the three immune groups were found to be less significant as compared to the overall group.
Therefore, it can be concluded from the current study that the patients belonging to the three immune groups were more likely to be symptomatic as compared to patients belonging to the overall group. However, no variation in severity or symptomatology was observed in the three immune groups. Also, fewer associations between symptoms were observed in the three immune groups. Thus, more care needs to be taken while generating models and building diagnostic tools for COVID in people with pre-existing immune conditions. This study also calls for a more targeted assessment and treatment process for COVID-19 patients with immune comorbidities.

 *Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
*Important notice: medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.