Researchers report that declining PPP2R5C levels in blood may signal early Alzheimer’s pathology, offering new insight into tau regulation and future diagnostic strategies
Study: Neuronal PPP2R5C in plasma is a potential biomarker for early diagnosis of Alzheimer’s disease
In a recent study published in the journal Cell Reports Medicine, researchers identified protein phosphatase 2 regulatory subunit B’β (PPP2R5C) as a potential early biomarker associated with Alzheimer’s disease (AD).
Alzheimer’s Disease Pathology and the Need for Early Biomarkers
AD is the most common form of dementia and disproportionately affects the aging population. Pathological changes in AD begin decades before symptom onset, highlighting the importance of identifying reliable early biomarkers to enable disease-modifying interventions at preclinical stages. Current diagnostic tools, including positron emission tomography (PET) imaging and cerebrospinal fluid (CSF) analysis, are costly and invasive, limiting widespread clinical implementation.
A central feature of AD pathology is tau protein hyperphosphorylation, which disrupts microtubule stability and promotes the formation of neurofibrillary tangles (NFTs), ultimately leading to neuronal dysfunction and cell death. Because tau phosphorylation plays a critical role in AD progression, regulators of tau phosphorylation may serve as diagnostic biomarker candidates.
Protein phosphatase 2A (PP2A) accounts for approximately 70% of total tau phosphatase activity in the human brain. PP2A is a heterotrimeric complex composed of scaffold and catalytic subunits associated with variable regulatory subunits. PPP2R5C is highly expressed in the brain, and prior research has linked a single-nucleotide polymorphism (SNP) in the PPP2R5C gene to AD risk. Whether PPP2R5C itself could function as a diagnostic biomarker remained unclear before this study.
Proteomic Identification of PPP2R5C in Neuron-Derived Exosomes
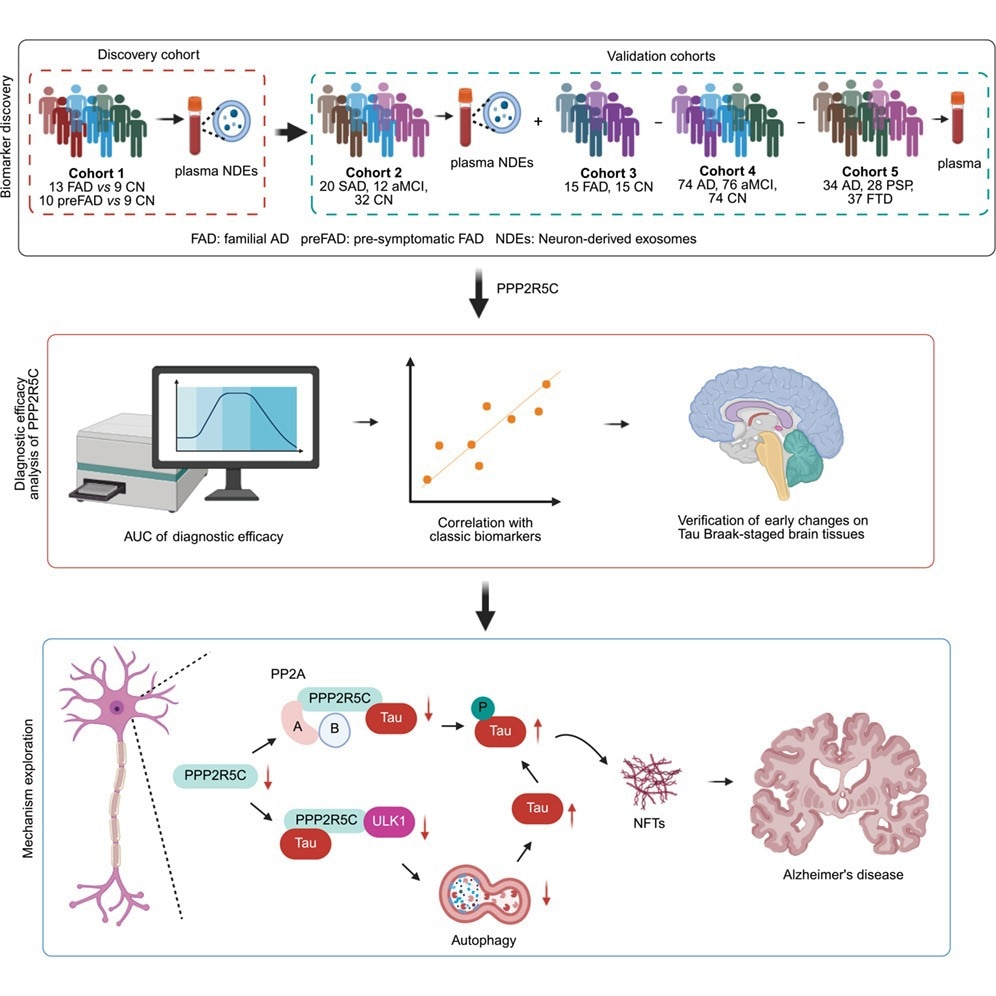
Researchers investigated PPP2R5C levels in neuron-derived exosomes (NDEs) isolated from plasma samples. The discovery cohort included 4 cognitively normal (CN) individuals, 4 presymptomatic familial AD (pre-FAD) participants, and 5 familial AD (FAD) patients. Label-free proteomic analysis showed that a PPP2R5C-specific peptide progressively decreased from presymptomatic FAD to FAD compared with cognitively normal controls.
This observation was validated in a second cohort consisting of 32 CN controls, 20 sporadic AD patients, and 12 individuals with amnestic mild cognitive impairment (aMCI) using targeted NDE analysis. Findings suggested reduced PPP2R5C expression may be associated with early AD pathological processes.
Plasma PPP2R5C as a Minimally Invasive Biomarker
Because isolating NDEs from plasma is technically challenging, researchers evaluated total plasma PPP2R5C as a more practical biomarker candidate. In a third cohort comprising 15 FAD patients and 15 CN controls, plasma PPP2R5C levels were significantly lower in AD patients.
Further analyses showed that plasma PPP2R5C levels were approximately 61.3% lower in aMCI and 31.6% lower in AD than in CN controls. The AD group exhibited 52.1% lower plasma PPP2R5C than the aMCI group.
Plasma PPP2R5C distinguished AD from CN controls with an area under the receiver operating characteristic curve (AUROC) of 0.8494 and differentiated aMCI from controls with an AUROC of 0.7360. Differentiation between aMCI and AD yielded an AUROC of 0.5931, indicating limited stage-discrimination capability.
Plasma PPP2R5C was positively associated with Mini-Mental State Examination (MMSE) scores and negatively correlated with plasma phosphorylated tau 181 (p-tau181), p-tau217, and p-tau231 levels, supporting relevance to tau pathology.
Brain Expression Patterns and Early Braak Stage Changes
Postmortem brain analyses revealed lower PPP2R5C levels in aged AD patients compared with young CN and aged CN individuals, suggesting aging alone does not substantially reduce PPP2R5C expression.
Immunohistochemical staining of Braak-graded AD brain samples showed PPP2R5C expression decreased as early as Braak stage II, when NFTs were still relatively limited. In Braak stages II and IV, PPP2R5C levels remained consistently low despite increased NFT accumulation, supporting the hypothesis that PPP2R5C reduction may precede extensive tau pathology.
Mechanistic Role of PPP2R5C in Tau Regulation
Co-immunoprecipitation experiments demonstrated interaction between PPP2R5C and tau. Increasing PPP2R5C expression reduced phosphorylated tau and total tau levels while enhancing PP2A enzymatic activity. Silencing PPP2R5C decreased PP2A activity, suggesting a regulatory role rather than a purely correlative association.
Pharmacological inhibitor experiments indicated PPP2R5C-driven tau degradation was blocked by autophagy-lysosome inhibitors, including chloroquine, leupeptin, and ammonium chloride, but not by the proteasome inhibitor MG132. These findings implicate the autophagolysosomal pathway in PPP2R5C-mediated tau clearance.
Because the unc-51-like kinase 1 (ULK1) complex regulates early autophagy induction, researchers assessed its involvement. Immunoblotting showed a negative correlation between PPP2R5C expression and phosphorylated ULK1. Molecular docking suggested PPP2R5C binds an accessible region on ULK1, and co-immunoprecipitation confirmed interaction, although binding affinity was not directly quantified.
Clinical Implications and Future Validation Needs
Collectively, findings suggest PPP2R5C may serve as a plasma biomarker candidate associated with early AD pathological processes. Reduced PPP2R5C appeared to precede tau hyperphosphorylation and was not observed in cognitively normal aged individuals.
Mechanistically, PPP2R5C interacts with tau, modulates PP2A activity, and promotes tau degradation via a ULK1-dependent autophagolysosomal pathway. However, the study does not establish PPP2R5C as a definitive diagnostic marker.
Larger, longitudinal, and ethnically diverse cohort studies are needed to validate these findings. Assay standardization and reproducibility studies will be essential before plasma PPP2R5C can be incorporated into routine clinical screening or early diagnostic workflows for Alzheimer’s disease.