A study conducted by UK researchers has found that patients hospitalized with coronavirus disease 2019 (COVID-19) were less likely to be current smokers than patients who had been admitted with other types of respiratory viral infections last year (2019).
The researchers also found that smoking prevalence among the patients hospitalized with COVID-19 was significantly lower than would be expected in the local general population.
Worryingly, the team reports that data on smoking status was poorly recorded, with the information in electronic health records (EHRs) deviating significantly from that available in medical notes.
Robin Bailey from London School of Hygiene and Tropical Medicine and colleagues say this poor recording is a concern, particularly for studies that rely solely on EHRs as the source of information on smoking status.
A pre-print version of the paper is available on the medRxiv* server, while the article undergoes peer review.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Whether smoking increases risk of COVID-19 hospitalization is uncertain
COVID-19 is a respiratory disease caused by the highly infective severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
To infect cells, SARS-CoV-2 uses a surface viral protein to bind to the human receptor angiotensin-converting enzyme 2 (ACE2) and fuse with the host cell membrane.
Some studies have suggested that ACE2 is expressed at higher levels in the airways of smokers, potentially increasing their likelihood of contracting the virus. However, other studies have suggested that smoking in fact decreases the expression of ACE2.
A review of 279 studies found that current smokers were at less risk of testing positive for SARS-CoV-2 than never smokers, while former smokers were at a greater risk of severe disease and hospitalization than never smokers.
However, most of these studies were limited by a lack of appropriate control groups, poor recording of smoking status, and insufficient adjustment for potential confounding variables, say Bailey and the team. Many studies also used routine EHRs to obtain individual-level data on demographic characteristics, comorbidities and smoking status.
“Previous research suggests that data on smoking status obtained via EHRs tend to be incomplete or outright inaccurate,” write the researchers.
Furthermore, since hospitalized populations differ from the general population in terms of age and sex, comparisons of current and former smoking prevalence in hospitalized and non-hospitalized populations are probably limited, they add.
“There is hence an urgent need for alternative study designs with relevant comparator groups (e.g., populations hospitalized with a similar type of respiratory viral infection) and adjustment for covariates to better understand the association of smoking status with COVID-19 disease outcomes,” says the team.
What did the researchers do?
In an observational, retrospective case-control study conducted at an NHS hospital trust in London, the team examined the association of former and current smoking with hospitalization for COVID-19 compared with hospitalization for other respiratory virus infections a year previously.
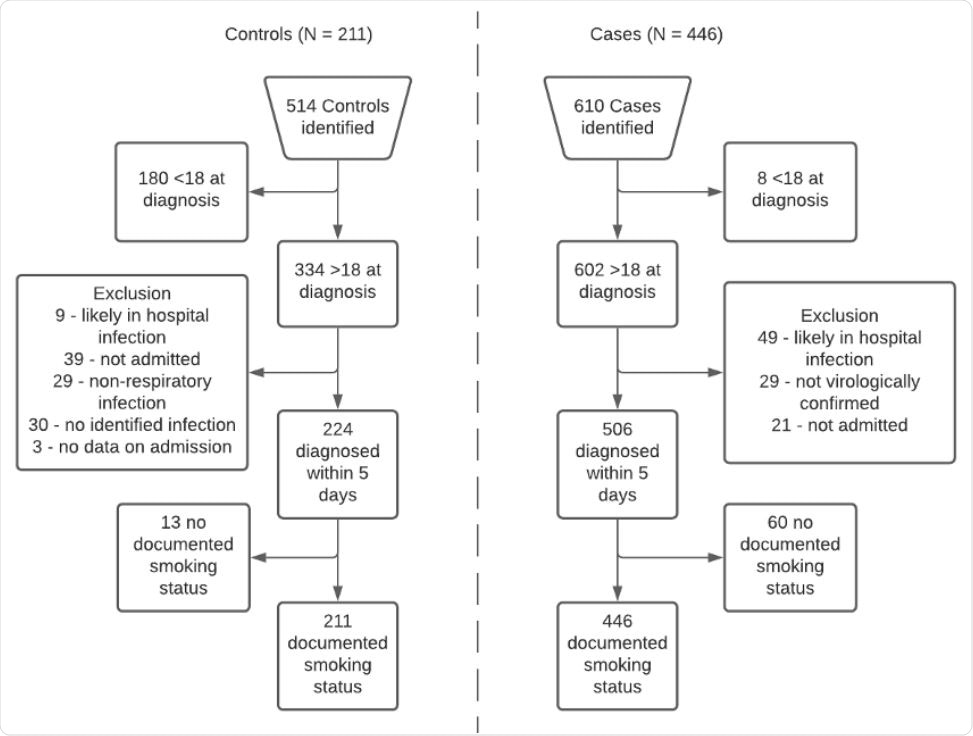
Eligibility flow diagram for controls (left hand side) and cases (right hand side).
The researchers also obtained London smoking prevalence data from the representative Annual Population Survey.
The data were analyzed using logistic regression analyses to adjust for age, sex, socioeconomic position, and comorbidities.
The study included 446 hospitalized COVID-19 patients (cases) where data was obtained between 1st March 2020 and 26th August 2020. These patients were compared with 211 patients admitted with other respiratory viral infections (controls) where data was obtained between 1st January 2019 and the 31st December 2019.
What did the study find?
Hospitalized COVID-19 patients were 45% less likely to be current smokers than patients who had been admitted with other respiratory viral infections the previous year.
No significant difference in the odds of being a former smoker was observed between the two groups.
The prevalence of current smoking among cases was significantly lower than would be expected based on age- and sex-matched local smoking prevalence, at 9.4% versus 12.9%.
The low prevalence of current smoking in cases appeared to be driven by current smokers being underrepresented among those aged 45- 59 years. In all other age groups (30-44 years, 60-74 years, and 75 plus years), the prevalence was similar to the expected London prevalence.
“It should be noted that cases aged 45-59 years were more likely to reside in less deprived areas than controls,” says Bailey and colleagues. “As smoking status is strongly associated with socioeconomic position, this may partly explain the lower smoking prevalence in this age group.”
Smoking status was poorly recorded
Smoking status was poorly recorded, with the status recorded on the summary EHRs significantly deviating from that recorded in medical notes.
This poor recording was more prominent among controls than cases, which the researchers say can likely be explained by the observation that discharged COVID-19 patients attended a follow-up clinic where they were specifically asked about their smoking status.
“The observed discrepancy between smoking status recorded on summary EHRs and the contemporaneous medical notes is a concern, particularly for studies relying solely on EHRs as the source of information on smoking status,” warn the researchers.
Longitudinal, representative population-level studies from multiple sites are needed
“To our knowledge, this is one of few studies specifically designed to examine the association between smoking status and hospitalization with COVID-19,” writes the team.
Bailey and colleagues say that to better understand the role of smoking as a risk factor for COVID-19 hospitalization, longitudinal, representative population-level studies from multiple sites are required.
“Purposeful acquisition of accurate smoking status is required to characterize the role of smoking in COVID-19 disease outcomes,” they add.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources