The ongoing coronavirus disease 2019 (COVID-19) pandemic has put significant pressure on the healthcare and government sectors around the world. Through the use of robust data, both clinicians and policymakers are adopting diverse strategies to save the lives of people throughout the world.
Both observational cohort data that describe clinical characteristics, as well as the likelihood of severe outcomes, provide guidance in health policy development, the production of research hypotheses for clinical trials, and improvement of clinical guidelines for patient care.
Multiple cohort studies describing the clinical impact of the COVID-19 pandemic have taken place throughout the world. However, difficulties were faced while comparing diverse and fragmented datasets that were often found to differ in their inclusion criteria, outcome measures, and case definitions.
The Clinical Characterization Protocol (CCP) that was developed by the International Severe Acute Respiratory, along with the emerging Infection Consortium (ISARIC) and the World Health Organization (WHO), provided help to researchers across the globe for the collection and analysis of clinical data.
A new study published in the pre-print server medRxiv* discusses data acquired from an international cohort that contained almost half a million patients from 720 sites across 9 different countries. The study summarized the clinical presentation and demographic features of patients who were hospitalized with COVID-19 in low, middle, and high resource settings. The current study also characterized the variability in clinical features observed in these patients and explored the risk factors that were associated with mortality, mechanical ventilation, and intensive care.
About the study
The current study involved 439,922 patients who were hospitalized between January 2020 and May 2021 from 720 different sites across 49 countries. Most of the recruited patients belonged to the United Kingdom and South Africa, with 50.1 percent of the recruited patients being male with a median age of 60 years. The patients were regularly monitored until their discharge or death.
Cox proportional hazards models were used to determine the association of comorbidities, demographic variables, and symptoms with the risk of use of invasive mechanical ventilation (IMV), admission to intensive care unit (ICU), or high-dependency unit (HDU), or death. The individuals who were lost to follow-up or remained in the hospital on May 24, 2021, were censored.
The time from the onset of symptoms to censoring or death, whichever occurred earlier, was considered as the time scale. For ICU patients, the time scale was from the onset of symptoms to the admission to ICU, discharge, death, or censoring. For IMV, the time scale was from the onset of symptoms to IMV, death, or discharge.
Study findings
The results indicated that the most common symptoms associated with COVID-19 were fever, cough, and shortness of breath. However, some variations in symptoms occurred, depending on the country. Among older patients, the most common symptom was altered consciousness, while among younger patients often experienced gastrointestinal symptoms.
The data shows that about one-third of the patients do not meet one of the four international symptom-based case definitions, particularly those who belong to the younger and older age group. These differences were of importance during defining tests and isolation and also helped in the detection of new variants and clusters of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
The results of the study also confirm that there is a strong association between age and risk of death in individuals suffering from COVID-19. Moreover, individuals belonging to the older age group have greater chances of dying. The study showed that every decade of life added a 50% chance of death. Additionally, men were found to be at a higher risk of death than women.
The risk of admission to ICU and IMV increased in patients belonging to 20-30 years of age and started decreasing from age 60. Patients who were 80 years old were unlikely to be admitted to the ICU. Also, it was found that men were more likely to be admitted to ICU than women.
The study found that the presence of five comorbidities was strongly associated with the risk of death. The most prominent risk factor was high blood pressure, diabetes, and chronic heart disease. Other comorbidities that were associated with the risk of death included chronic kidney disease, transplantation, immunosuppression, and chronic pulmonary disease. Pregnancy, on the other hand, was associated with a lower risk of death in patients who were admitted to hospitals.
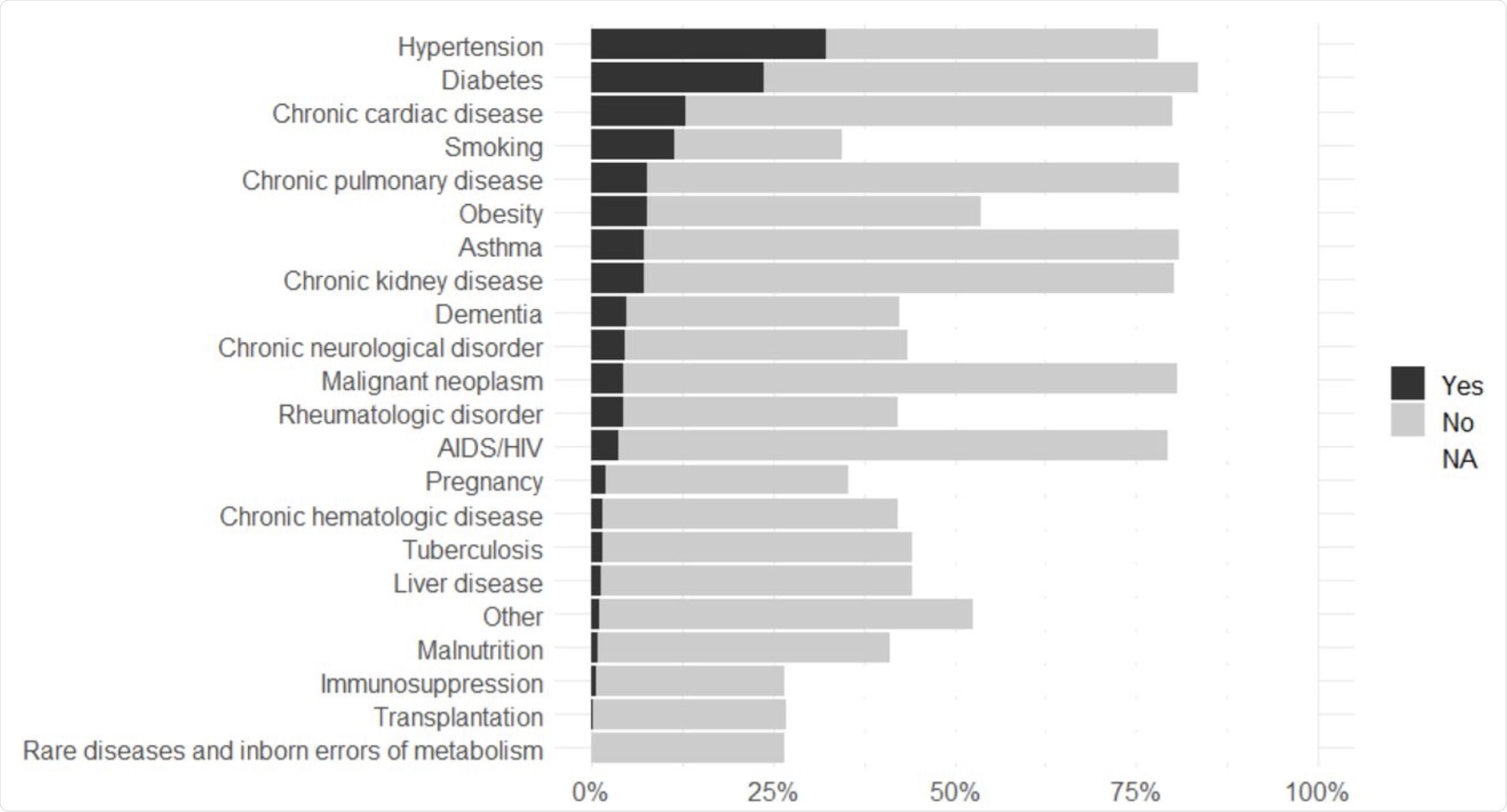 Prevalence of pre-existing comorbidities and risk factors.
Prevalence of pre-existing comorbidities and risk factors.
The global case fatality ratio (CFR) was found to be much higher in patients who were admitted to the ICU on the first day as compared to patients who required ICU admission at any point during their admission. The results also indicated that most of the patients admitted to the hospital required oxygen therapy delivered by a high-flow nasal cannula followed by non-invasive ventilation (NIV) and IMV.
Conclusion
The current study was able to overcome some of the traditional problems of observational studies and could be used as a crucial model for planning the health system. The ISARIC global collaboration continues to collect standardized data that will help in the improvement and implementation of treatment, vaccination, and public health control strategies.
The study had certain limitations. Although it involved a broad range of data from different countries, different sites were found to have different data completeness. Secondly, the study provided an insight into the risk factors associated with COVID-19; however, pandemics are dynamic and complex, which makes it difficult to monitor them. The study also did not include the new SARS-CoV-2 variants of concern.

 This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
This news article was a review of a preliminary scientific report that had not undergone peer-review at the time of publication. Since its initial publication, the scientific report has now been peer reviewed and accepted for publication in a Scientific Journal. Links to the preliminary and peer-reviewed reports are available in the Sources section at the bottom of this article. View Sources
Journal references:
- Preliminary scientific report.
Kartsonaki, C. (2021). Characteristics and outcomes of an international cohort of 400,000 hospitalised patients with Covid-19. medRxiv. doi:10.1101/2021.09.11.21263419 . https://www.medrxiv.org/content/10.1101/2021.09.11.21263419v1
- Peer reviewed and published scientific report.
Kartsonaki, Christiana, J Kenneth Baillie, Noelia García Barrio, Joaquín Baruch, Abigail Beane, Lucille Blumberg, Fernando Bozza, et al. 2023. “Characteristics and Outcomes of an International Cohort of 600 000 Hospitalized Patients with COVID-19.” International Journal of Epidemiology, February. https://doi.org/10.1093/ije/dyad012. https://academic.oup.com/ije/advance-article/doi/10.1093/ije/dyad012/7059267.